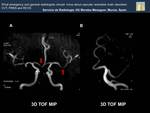
Fig. 17
References: Department of Radiology, Hospital General Universitario Morales Meseguer

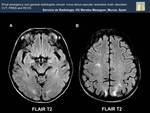
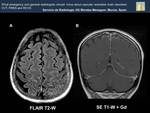
Fig. 18: Bilateral and simmetrical subcortical hyperintensities in occipital lobes (Image A), and precuneus, (Image B) , are noted. A small hyperintense lesion is shown in right frontal lobe. The appearance and distribution of the lesions suggests a possibility of PRES.
References: Department of Radiology, Hospital General Universitario Morales Meseguer

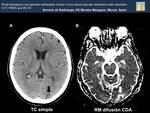
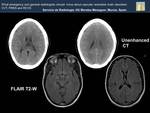
Fig. 19: Hypodensity with finger morphology in left occipital subcortical white matter (black arrow , Image A) . Increase of ADC value in left occipital lobe (white arrow, Image B). These findings are due to vasogenic edema.
References: Department of Radiology, Hospital General Universitario Morales Meseguer
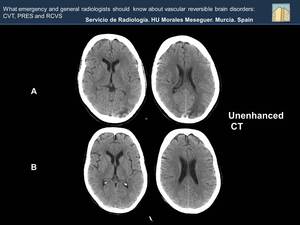
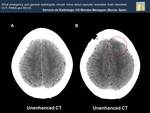
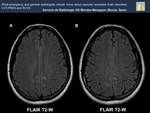
Fig. 20: What characterizes PRES is the reversibility of the lesions. Hypodensity of subcortical white matter in left posteriorvasculary territoriy (Image A), has disappeared as we see in the CT carried out a few month later (Image B).
References: Department of Radiology, Hospital General Universitario Morales Meseguer
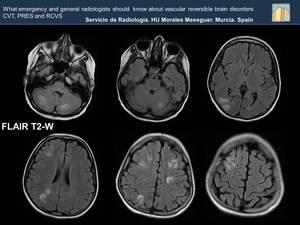
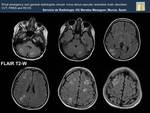
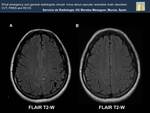
Fig. 22: The FLAIR sequence shows multiple , bilateral and rather symmetric hyperintense lessions affecting cerebellar hemispheres, right occipital, parietal and frontal lobes.
References: Department of Radiology, Hospital General Universitario Morales Meseguer

Fig. 21
References: Department of Radiology, Hospital General Universitario Morales Meseguer
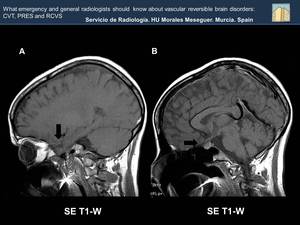
Fig. 23: Increased intracranial pressure causes a descent of frontal lobe (black arrow, figure A) , and a narrowing of the sellar cistern (black arrow, Figure B).
References: Department of Radiology, Hospital General Universitario Morales Meseguer

Fig. 24: At first the CT may be normal (Image A) . As time passes you can see edema (red circle, Image B).
References: Department of Radiology, Hospital General Universitario Morales Meseguer
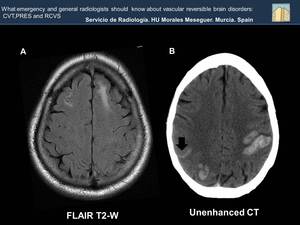
Fig. 25: FLAIR sequence shows hyperintensity in subcortical white matter of both frontal lobes due to edema (Image A). Increasing density on the back of the superior sagital sinus (SSS) because of thrombosis (Image B). The involvement of the SSS is related to bilateral intraparenchymal hemorrhages as seen in this patient. A subarachnoid hemorrhage (black arrow) is also noted.
References: Department of Radiology, Hospital General Universitario Morales Meseguer
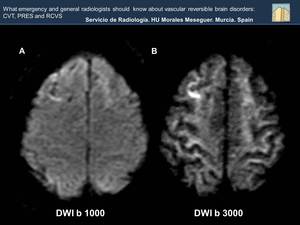
Fig. 26: Diffusion MRI is not the best technique to evaluate venous thrombosis, because it may be normal. Sometimes you can see a restriction in the diffusion sequence. The best technique for diagnosis is the gradient echo MRI sequence
References: Department of Radiology, Hospital General Universitario Morales Meseguer
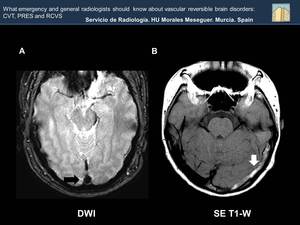
Fig. 27: The blooming sign (black arrow, Image A) in the early days , in more conspicuous than T1, T2 and FLAIR hyperintensity in the veins /sinus thrombosis . Transverse sinus thrombosis (white arrow, Image B).
References: Department of Radiology, Hospital General Universitario Morales Meseguer
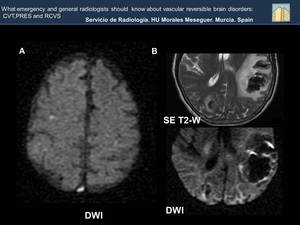
Fig. 28: Image A: Restricted diffusion in the posterior portion of the superior sagital sinus because of thrombosis. Image B: Hemorrhage in the left parietal and right occipital lobes secondary to thrombosis.
References: Department of Radiology, Hospital General Universitario Morales Meseguer
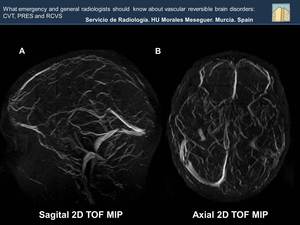
Fig. 29: The absence of flow of the venous venous sinuses is well assessed in MR venography sequences.
References: Department of Radiology, Hospital General Universitario Morales Meseguer
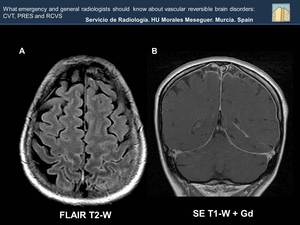
Fig. 30: The absence of flow of the venous venous sinuses is well assessed in MR venography sequences.
References: Department of Radiology, Hospital General Universitario Morales Meseguer

Fig. 31
References: Department of Radiology, Hospital General Universitario Morales Meseguer
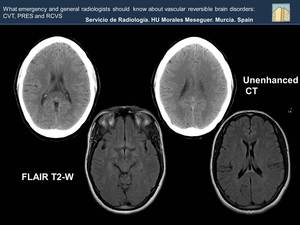
Fig. 32: At the beginning studies may be normal, so if there is a high clinical suspicion you cannot rule out a RCVS.
References: Department of Radiology, Hospital General Universitario Morales Meseguer
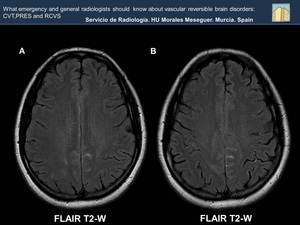
Fig. 33: In both T2 weighted images( Image A and B) occupancy of the sulci of the middle convexity with hyperintense lineal material compatible with subarachnoid hemorrhage is shown
References: Department of Radiology, Hospital General Universitario Morales Meseguer
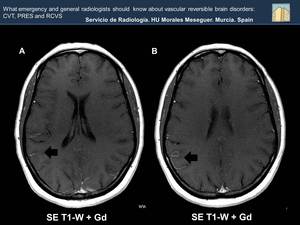
Fig. 34: In both images (A and B) vessesls engorgement related to vascular slowdown is observed (Black arrows).
References: Department of Radiology, Hospital General Universitario Morales Meseguer
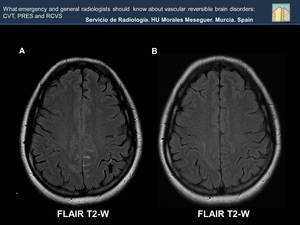
Fig. 37: Occupancy of the sulci of the middle convexity with hyperintense linear material, compatible with subarachnoid hemorrhage and a vascular slowdown (black arrow) are displayed ( Image A). These findings have disappeared as we see in the MRI carried out a few month later (Image B)
References: Department of Radiology, Hospital General Universitario Morales Meseguer

Fig. 35: Linear hyperintensity of gyriform morphology with hypointensity of the adjacent white subcortical matter (Image A). A more obvious edema-ischemic of the cortical white matter (Image B). The findings are compatible with a cortical bleeding and edema-ischemic in surrounding subcortical white matter.
References: Department of Radiology, Hospital General Universitario Morales Meseguer
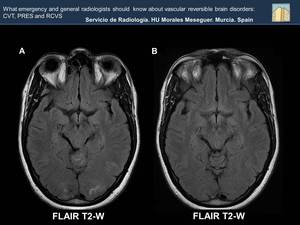
Fig. 36: Bilateral hyperintensity with a finger-morphology in the subcortical occipital white matter suggestive of vasogenic edema, more obvious on the left side (Image A). In a posterior control, the resolution of edema is shown (Image B). Imaging findings secondary to reversible cerebral edema, wich has a similar distribution of the PRES.
References: Department of Radiology, Hospital General Universitario Morales Meseguer
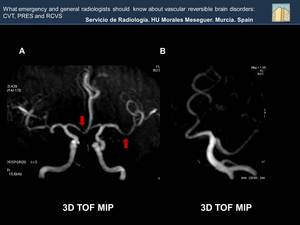
Fig. 38: In both images scattered bilateral small foci of vascular stenosis are identified (red arrows).
References: Department of Radiology, Hospital General Universitario Morales Meseguer