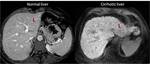
A non invasive diagnosis of cirrhosis can be done at CT and MRI by identifying hepatic and extrahepatic signs of cirrhosis.
HEPATIC SIGNS
At earlier stages of cirrhosis,
the liver can appear normal or show only subtle heterogeneity.
With disease progression,
characteristic regional changes in hepatic morphology are seen,
such as hypertrophy of the caudate and left lobes and atrophy of the segment IV.
Enlarged hilar periportal space
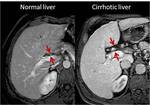
An enlarged hilar periportal space (defined as a distance between the right portal vein and the posterior edge of segment IV greater than 10 mm) may be the only morphological sign at earlier stages of cirrhosis (Figure 1).
This sign is consequence of segment IV atrophy.
Although the exact mechanism remains unclear,
it is thought to be related to portal venous hypoperfusion.
Normally,
segment IV receives less portal venous blood than other segments.
Cirrhosis cause a decrease of portal venous flow and a consequent atrophy of segment IV.
Caudate-right lobe ratio
The caudate-right lobe ratio (C/RL) is an useful tool to differentiate normal and cirrhotic liver.
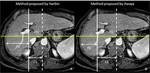
Harbin reported that a C/RL greater than 0.65 was suggested a diagnosis of cirrhosis using the main portal vein bifurcation as a landmark between the two lobes (Figure 2a).
More recently,
Awaya noted that the hypertrophied caudate lobe extended beyond the main portal vein bifurcation,
and proposed a modified C/RL,
which uses the bifurcation of the right portal vein as a landmark (Figure 2b).
A ratio greater than 0.55 suggested a diagnosis of cirrhosis.
Right posterior hepatic notch sign
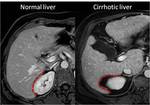
Hypertrophy of caudate lobe is also responsible for the right posterior hepatic notch sign (Figure 3).
In normal liver,
the right postero-inferior liver surface is concave.
In cirrhotic liver,
a sharp indentation (“notch”) in the right medial posterior liver surface can be observed.
The “notch” corresponds to the boundary between the atrophied right posterior segments and the hypertrophied caudate lobe.
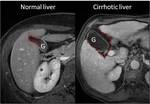
Enlarged gallbladder fossa
In normal liver,
the gallbladder fossa is delimited laterally by the right lobe and medially by the segment IV,
and contains little fat. In cirrhotic liver, the gallbladder fossa can be enlarged (Figure 4).
This sign is the consequence of a combination of the following factors: 1) hypertrophy of the caudate lobe; 2) hypertrophy of the left lobe; 3) atrophy of segment IV; 4) atrophy of right posterior segments and right lobe.
The enlarged gallbladder fossa is considered to be present only when the gallbladder fossa is delimited laterally by the right lobe and medially by the segments II and III.
Nodular margins
Nodule formation and distortion of hepatic architecture have variable effect on liver surface.
Configuration of hepatic margins correlates with gross appearance of cirrhosis.
Smooth margins suggest micronodular cirrhosis (RNs < 3 mm).
Nodular margins suggest macronodular cirrhosis (RNs > 3 mm) (Figura 5).
Irregularities are typically more evident on the surface of the enlarged left lobe.
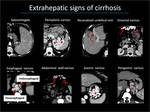
EXTRAHEPATIC SIGNS
Extrahepatic signs include splenomegaly (splenic length greater than 13 cm) and sequelae of portal hypertension (Figure 6).
Portal hypertension in cirrhosis is the consequence of increased portal pressure at level of sinusoids and compression of central vein by perivenular fibrosis.
At earlier stage of portal hypertension,
portal system dilates and a main portal vein diameter of greater than 13 mm is usually observed.
With disease progression,
portal venous blood reverses direction (from hepatopetal to hepatofugal),
and pass into the low pressure systemic circulation through portosystemic collateral pathways.
The most common portosystemic pathways are gastroesophageal varices,
paraumbelical vein,
abdominal wall varices,
perisplenic varices,
rectal varices,
and splenorenal shunts.
Among theses,
esophageal varices are the most clinically important because of the risk of rupture and massive bleeding.
Other sequaelae of portal hypertension are ascites and portal vein thrombosis.
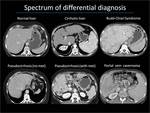
MIMICS OF CIRRHOSIS
Several conditions can cause liver morphology changes,
and mimic liver cirrhosis (Figure 7).
Knowledge of these conditions is crucial to avoid misinterpretations.
Budd-Chiari syndrome
Budd-Chiari syndrome is characterized by hypertrophy of the caudate lobe and variable atrophy/hypertrophy of the remaining portions of the liver.
Focal nodular regenerative hyperplasia has been primarily reported in long-standing Budd-Chiari syndrome.
Pseudocirrhosis
Chemotherapy can cause liver toxicity and alterations of liver morphology.
Typical findings include capsular retraction,
segmental volume loss,
lobular hepatic contours and enlargement of the caudate lobe.
Liver metastases are sometimes absent.
Portal vein cavernoma
Cavernous transformation of the portal vein can cause atrophy of the left and right liver lobes and hypertrophy of segment I and IV.
These changes were described as the atrophy-hypertrophy complex.