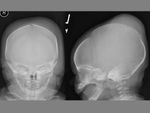
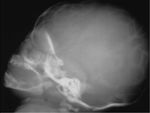
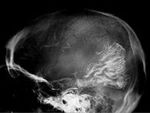
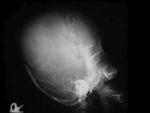
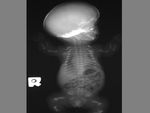
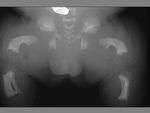
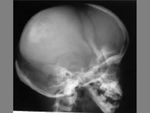
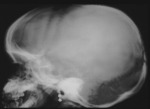
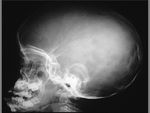
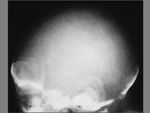
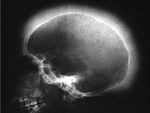
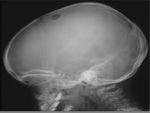
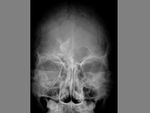
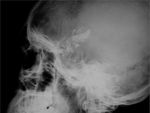
CEPHALHEMATOMA
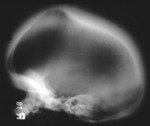
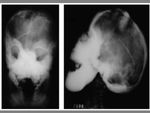
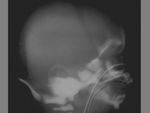
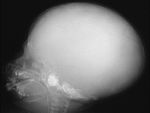
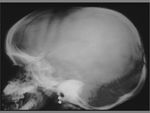
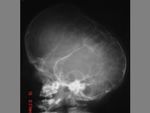
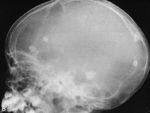
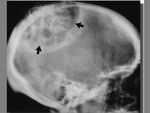
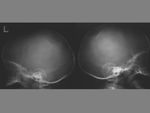
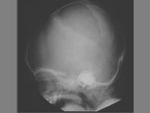
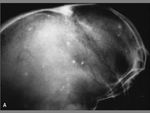
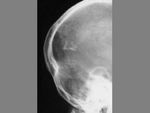
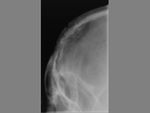
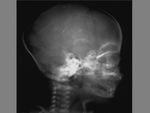
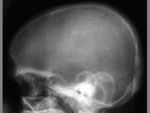
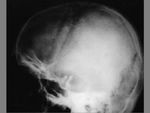
The term cephalohematoma signifies a traumatic subperiosteal hematoma of the calvaria.
Because the cephalohematoma is bounded by the outer layer of the periosteum and the sutures,
it cannot cross the midline.
This restriction distinguishes it from subgaleal hematoma,
which does cross the midline deep to the galeal aponeurosis.
Cephalohematomas occur in approximately 1%–2% of live births,
are almost twice as common in males than in females,
and are more common in children of primiparous mothers.
The incidence increases after forceps extraction.
Cephalohematomas manifest as firm,
tense soft-tissue masses that usually increase in size after birth.
They resolve spontaneously.
Most calcify peripherally and gradually incorporate into the calvaria.
Cephalohematomas may be unilateral or bilateral.
ARNOLD CHIARI MALFORMATION
Synonyms:
Type I: tonsillar herniation or tonsillar ectopia.
Type II: none.
Description:
In 1891 Chiari and later Arnold (1894) described the morphologic changes of the hindbrain that now bear their names,
the Arnold-Chiari malformation.
The brain changes are characterized by downward displacement or elongation of the brainstem and cerebellar tonsils through the foramen magnum.
Hydrocephalus is variably present and mild.
There are two main presentations.
SKULL:
Normal membranous bone formation of the cranial vault requires distention of the cranial vault requires distension of the underlying brain and ventricular system that is lacking in Chiari II malformation.
Radial growth of the developing calvarium is profoundly altered.
This results in the so called lacunar skull / luckenschandel.
The gross pathology and plain film radiographic appearance are striking.
Focal calvarial thinning and a scooped-out appearance are typical.
These skull changes are most striking at birth but diminish with age.
Although the most obvious manifestation of lacunar skull resolve by about 6 months,
subtle calvarial thinning and scalloping may persist into adulthood.
Other findings include:
SKULL AND DURA (Cross sectional findings):
- Small posterior fossa with low lying with low lying transverse sinuses.
- Fenestrated falx
- Heart shaped inscisura with hypoplastic tentorium
- Gaping foramen magnum
- Concave clivus and petrous ridges.
BRAIN
- Inferiorly displaced vermis
- Medullary spur
- Beaked tectum
- Interdigitated gyri
- Cerebellum “ creeps” around brainstem and “tower” through wode tentorial incisura
- Associated anomalies: Callosal dysgenesis,
heterotropias,
polymicrogyria,
stenogyria.
VENTRICLES:
- Whole system: Hydrocephalus
- Fourth: Elongated,
inferiorly displaced
- Third: Large massa intermedia: May be high riding if callosum is absent.
- Lateral: Colpocephaly
SPINE:
- Myelomeningocoele in nearly 100%
- Syringomyelia 50-90%
- Diastomatomyelia
- Segmentation anomalies in <10%
- Incomplete C1 arch
STURGE WEBER SYNDROME
Sturge Weber syndrome (encephalotrigeminal angiomatosis) is a sporadically occuring phakomatosis characterised by a port wine vascular nevus flammeus in the trigeminal nerve nerve distribution (the first division is most frequently affected) leptomemningeal venous angiomatosis,
seizures demetia,
hemiplegia,
hemianopsia,
buphthalmos and glaucome.
The precise etiology of sturge weber syndrome is unknown but it is probably due to faulty development of cortical venous drainage.
Pathologic findings are those of a plexus of multiple small thin walled telengiactic capillaries or venules that lie along the brain along the subarachnoid space between the pia and aranchnoid membranes.
A paucity of normal cortical draining veins results in venous stasis and vascular congestion with hypoxia of the affected cortex.
Slowly progressive atrophy of the brain underlying the angioma occurs,
with dystrophic calcification in the middle layers of the cortical gray matter.
The angioma itself is not calcified.
Intracranial calcification is thee most common raediologic manifestation of SWS.
Detectable calcification before 2 years of age is uncommon.
Skull films demonstrate the suggestive of-called tram track pattern of calcification,
caused by calcification in apposing gyri on either side of an intervening dilated sulcus.
On CT,
curvilinear calcifications in a gyral pattern are observed.
These are most prominent in the occipital and posterior parietal lobes ipsilateral to the facial angioma.
Progressive cortical atrophy is commonly seen with secondary manifestations such as ipsilateral calvarial thickening and enlargement of the oparanasal sunisus and mastoid.
Associated abnormalities:
About one third of the patients with SWS have ocular abnormalities.
Congenital glaucoma with buphalmos is seen in 10% to 30%; scleral and choroidal angiomata have also been reported.
SWS can also be associated with the angio-osteo-hypertrophy of Klippel-Trenuanay syndrome.
APERTS SYNDROME
Apert syndrome is named for the French physician who described the syndrome acrocephalosyndactylia in 1906.
Apert syndrome is a rare autosomal dominant disorder characterized by craniosynostosis,
craniofacial anomalies,
and severe symmetrical syndactyly (cutaneous and bony fusion) of the hands and feet.
SKULL:
Skull radiography can be performed to evaluate for craniostenosis,
which usually involves coronal sutures and maxillary hypoplasia.
Abnormalities include sclerosis of suture line,
bony bridging and beaking along the suture line,
an indistinct suture line,
turribrachycephaly,
shallow orbits,
and hypoplastic maxillae.
Other findings include:
SPINE:
Spinal fusions,
most commonly at the levels of C3-4 and C5-6,
appear to be progressive and occur at the site of subtle congenital anomalies.
They may not be apparent as congenital features.
Small-sized vertebral body and reduced intervertebral disc space are indicators of subsequent bony fusion.
LIMBS:
Radiographs of the limbs depict multiple epiphyseal dysplasia,
short humeri,
and glenoid dysplasia.
Radiography of the hands can be performed to evaluate for cutaneous and osseous syndactyly.
The characteristic finding is complete syndactyly involving the second and fifth digits (mitten hands).
Multiple progressive synostosis involves distal phalanges,
proximal fourth and fifth metacarpals,
capitate,
and hamate.Symphalangism of interphalangeal joints is progressive.
Radiography of the distal phalanx reveals shortened and radial deviation.Radiography of the proximal phalanx of the thumbs reveals delta-shaped deformity.
Radiography of the feet can be performed to evaluate for cutaneous and osseous syndactyly.
The characteristic finding is complete syndactyly involving the second and fifth digits (sock feet).
Fusion of tarsal bones,
metatarsophalangeal and interphalangeal joints,
and adjacent metatarsalsDelta-shaped proximal phalanx of the first toesOccasional partial or complete duplication of the proximal phalanx of the great toes and first metatarsals
THANATOPHORIC DYSPLASIA
Thanatophoric Dysplasia (TD) is a congenital,
sporadic,
usually lethal skeletal dysplasia characterized by shortening of the limbs,
small conical thorax,
platyspondyly and macrocephaly.
Its incidence is 1 in 64000 to 1 in 100000 of the total live births.
It is of two major subtypes viz.
a short curved femur characterizes type 1,
while a straighter femur with clover leaf skull characterized type 2. It was first described by Maroteaux et al in 1967. The term ‘clover leaf skull’ has been used synonymously to Kleeblattschlader syndrome.
Thanatophoric Dysplasia is a condition of unknown etiology with the majority of case reports being sporadic.
Some authors have reported a dominant gene mutation to be associated with this condition.
Maternal Rubella infection has been proposed to be a probable etiological factor.
Molecular analysis of the fibroblast growth factor III receptor gene (FGFR 3) in both subtypes suggest that this is a genetically homogenous disorder.
This usually leads to in-utero death of the fetus; the longest survival however has been reported to be of 9 years. Males are affected more than females.
The case reported here was a male fetus delivered by Caesarean section and remained alive for twenty four hours only.
Short limb dwarfism is usually of two types: type 1 presenting with polyhydramnios,
macrocephaly,
short limbs,
narrow thoracic cage and curved short femur (the typical telephone receiver appearance) but without a cloverleaf skull.
Type 2 is characterized by short limbs,
narrow thoracic cage,
straight short femora,
hydrocephalus,
and cloverleaf skull.
However the other reported varieties are Torrance,
San-Diego,
and Luton types.
The present case belongs to type 1 with the ‘telephone receiver appearances’ of both the humerii and femora.
The thorax was narrow with horizontally placed ribs along with brachydactyly and absent carpals and tarsals.
Association of soft tissue syndactyly of fingers and toes was for the first time reported by Brodie et al.
Other associated anomalies are accessory pelvis ossification centers,
skin disorders,
like acanthosis nigricans and cerebral anomalies including that of temporal lobe gyri and hippocampus,
neuroglial heterotopias,
fibre tract hypoplasia,
dysplasia of deep nuclei etc.
Kyphosis and lordosis has also been observed.
Bowing of tubular bones may be explained by diminished mechanical stability.
Impaired endochondral ossification is more prominent towards the periphery of the metaphysis leading to tongue shaped osseus cones directed towards the epiphyses.
The perichondral spurs and linguiform endochondral growth plates result in ‘Maple leaf like’ contour of metaphyses of tubular bones and acetabular roof.
Death usually occurs either as a result of conical thorax and pulmonary hypoplasia (as seen in the present case) or due to cervical cord compression at a narrowed foramen magnum associated with posterior arch anomaly.
Antenatal sonography in second trimester not only confirms the diagnosis but also differentiates it from the other non lethal dysplasias.
Three dimensional ultrasound is able to visualize the thickened redundant skin fold,
limb and craniofacial anomalies more clearly. Nevertheless X-ray examination must be performed after birth to confirm various findings which along with the autopsy diagnosis helps in counseling of the parents.
PYKNODYSOSTOSIS
Defined in 1962 by Maroteaux and Lamy,
pyknodysostosis is thought to be the dysplasia that afflicted the French painter Toulouse-Lautrec.
This condition is transmitted by an autosomal recessive trait and is characterized by increased bone density,
dwarfism,
and skeletal fragility.
It has also been described as an autosomal dominant trait.
Though considered a distinct entity by most,
similarities with osteopetrosis and cleidocranial dysplasia do exist.
A generalized increase in bone density is seen,
with preservation of the medullary canal.
This osteosclerosis is most prominent in the long bones,
which are subject to transverse pathologic fractures.
Stress fractures of weight-bearing bones,
as well as fractures of the clavicle and mandible,
are often seen.
SKULL:
Numerous abnormalities are found in the skull.
The cranial sutures remain open,
with a wide anterior fontanelle; also,
numerous Wormian bones are seen.
The facial bones and sinuses are hypoplastic.
Mandibular hypoplasia with an obtuse angle results in a receding jawRetention of the deciduous teeth is often present,
with unerupted or malformed permanent teeth.
Osteomyelitis of the jaw is a frequent complication.
Platybasia is frequent.
Other findings include:
LONG BONES:
Hypoplasia or absence of the lateral ends of the clavicles and terminal tufts of the fingers and toes (acroosteolysis) is a consistent finding.
Bowing and overgrowth of the radius (Madelung’s deformity) contribute to abnormal radioulnar articulations.
SPINE AND PELVIS:
In the pelvis there may be shallow and obliquely roofed acetabula and coxa valga.
Spinal abnormalities include hyperlordosis,
scoliosis,
kyphosis,
and block vertebrae,
especially at the craniovertebral and lumbosacral regions.
Spool-shaped vertebrae and persistence of anterior infantile notching are frequently present.
Primary spondylolysis of C2 has been reported.
Spondylolisthesis of the lower lumbar vertebrae is also seen.
The lack of anemia and the preservation of the medullary canal help distinguish pyknodysostosis from osteopetrosis.
The short stature and dense bones of pyknodysostosis are absent in cleidocranial dysplasia
OSTEOPETROSIS
Osteopetrosis is a rare hereditary and familial bone abnormality characterized by the lack of resorption of normal primitive osteochondrous tissue.
The persistence of this tissue inhibits the formation of normal mature adult bone with a medullary canal containing marrow tissue.
There appear to be at least four forms: (a) a benign heterogenous form that is autosomal dominant,
(b) a severe malignant form that is autosomal recessive,
(c) an intermediate recessive type,
and (d) a recessive type with tubular acidosis (also known as carbonic anhydrase II deficiency syndrome).
Consanguinity apparently plays a role in the severe malignant form.
Recently,
clinical differences and progress in genetic understanding have now enabled identification of two distinct autosomal dominant types.
Synonyms include Albers-Schönberg disease,
osteosclerosis,
osteopetrosis generalisata,
osteosclerosis generalisata,
marble bones,
and chalk bones.
SKULL:
Skull changes include calvarial and basilar thickening and sclerosis,
with poor sinus development.
Endobones are frequently seen in the occipital and sphenoid bones with CT scanning.
The skull changes may produce macrocephaly and hydrocephalus.
The cranial manifestations of osteopetrosis have been evaluated and outlined with MRI.
Involvement of the mandible may result in prognathism.
Other findings include:
There is generalized sclerosis of the skeleton,
and there may be a homogeneous appearance of increased density,
without trabeculation,
and little or no differentiation between cortical and medullary regions.
Frequently,
however,
there are striations producing a bone within a bone appearance,
also referred to as endobones.
The endobones represent fetal vestiges and contain embryonic strata that are normally removed.
LONG BONES AND PELVIS:
The long bones have flared and elongated metaphyses; occasionally,
the shafts may be widened.
Involvement of the hands and feet parallel changes in the long bones,
and tuftal erosion has been reported.
Characteristically,
the ilium demonstrates multiple,
dense curved lines paralleling the iliac crest.
SPINE:
In the spine a number of presentations are seen.
The vertebrae may be uniformly dense or,
more commonly,
there are dense bands adjacent to the endplates,
with a more normal appearing midbody—the sandwich vertebra. The bone within a bone appearance is also commonly seen in the vertebral bodies.
Spinal stenosis with myelopathy in the cervical spine has been reportedSpondylolysis may be seen in the lumbar spine.
Differential diagnosis includes idiopathic hypercalcemia and heavy-metal poisoning.
CRANIO METAPHYSEAL DYSPLASIA
Craniometaphyseal dysplasia is a rare genetic bone remodeling disorder characterized by undertubulation of the long bones,
especially in the lower extremities,
causing deformities of the metaphyses of the long bones,
and sclerosis of the skull base or cranial bone hyperostosis.
Craniometaphyseal dysplasia (CMD) is a rare genetic bone remodeling disorder.
Its main characteristics are undertubulation of the long bones,
especially in the lower extremities causing deformities of the metaphyses in association with sclerosis or hyperostosis of the bones of the skull base.
Broadening of the short tubular bones with metaphyseal and diaphyseal abnormalities and,
sometimes,
diaphyseal expansion and widening of the ribs and clavicles may also be observed in this syndrome.
Craniometaphyseal dysplasia (CMD) is a rare congenital bone dysplasia characterized by sclerosis of the skull bones,
hyperostosis of skull base,
frontal,
facial and occipital bones and widening of the metaphyseal region of long bones.[1] Abnormal bony overgrowth leads to characteristic facial features and cranial nerve compression
Craniometaphyseal dysplasia is an extremely rare genetic disorder characterized by distinctive abnormalities of the head and facial (craniofacial) area,
impairment of certain nerves (cranial nerves) that emerge from the brain,
and malformations of the long bones of the arms and legs.
In infants and children with craniometaphyseal dysplasia,
there may be overgrowth and/or abnormal hardening of certain bones of the skull (cranial hyperostosis and/or sclerosis) and overgrowth (hypertrophy) of craniofacial bones,
resulting in widely-spaced eyes (ocular hypetelorism),
an abnormally wide nasal bridge,
an enlarged lower jaw (mandible),
and a "leonine" facial appearance (leontiasis ossea).
Compression of certain nerves emerging from the brain (cranial nerves) may result in loss of some motor function (paralysis) in the facial area (cranial nerve palsy) and hearing loss (conductive and/or sensorineural hearing impairment).
In addition,
in individuals with the disorder,
the long bones of the arms and legs may develop abnormally,
resulting in unusual "club-like" flaring or broadening of the end portions (metaphyses) of the bones (metaphyseal dysplasia).
In some cases,
craniometaphyseal dysplasia may be inherited as an autosomal dominant genetic trait; in other cases,
the disorder may have an autosomal recessive mode of inheritance.
FRONTO-METAPHYSEAL DYSPLASIA
Frontometaphyseal dysplasia (FMD) is an uncommon genetic syndrome affecting bone and connective tissue.
This condition is characterized by hyperostosis of the skull and prominence of the supraorbital ridges; long bones have flared metaphyses.
Frontometaphyseal dysplasia is an X-linked dominant trait with more severe.Clinical manifestations include childhood onset,
short trunk with long extremities,
prominent supraorbital ridges micrognathia and joint contractures.
Imaging features calvarial hyperostosis,
prominent supraorbital ridge,
absent frontal sinuses,
hypoplasia of angle and condylar processes of mandible,
antegonial notching of body of mandible,
flaring of the iliac wings with widening of ischial bones.
Changes in tubular bones include fibular waviness and bowing,
tibia recurvatum,
elongation of metacarpal bones,
and phalanges with erosion and fusion of carpal and tarsal bones.
OSTEOGENESIS IMPERFECTA
Osteogenesis imperfecta is a bone dysplasia characterized by osteoporosis and osseous fragility.
Dominant-negative mutations within the COL1A1 and COL1A2 genes cause molecular defects in type I collagen,
resulting in decreased collagen matrix in the skin and bones.
Four distinct subgroups of osteogenesis imperfecta are now defined,
according to severity and inheritance.
The autosomal dominant types I and IV are the least severe forms.
The autosomal recessive type III is more severe and manifests in early infancy.
The autosomal dominant type II is a lethal condition that manifests at birth.
Most cases of type II osteogenesis imperfecta arise as new mutations.
The cardinal roentgen features of osteogenesis imperfecta are a diffuse decrease in bone density,
pencil-thin cortices,
and multiple fractures.
Fairbank subdivided osteogenesis imperfecta into three groups based on radiographic findings: thin and gracile bones; short,
thick bones; and cystic bones.
The thin and gracile type is most frequent and these are generally osteogenesis imperfecta tarda patients.
Patients with the congenita form often have the thick bone radiographic appearance.
This description,
however,
is misleading because although the bone is wider than normal owing to fracture deformity,
the cortices are paper thin and the overall density is diminished.
The cystic type is rare and is characterized by osteopenic,
flared metaphyses.
This flared,
cystic appearance may extend into the diaphyses.
The radiographic subtypes are purely descriptive,
and patients may be seen to change from one type to another.
Others have developed another classification,
types A through F,
based on six radiologic criteria: (a) vertebral contours,
(b) bowing of long bones,
(c) trefoil-shaped pelvis,
(d) cystic changes in long bone metaphyses and epiphyses,
(e) thickness of long bone cortices,
and (f) thickness of rib cortices. This classification defines a narrower spectrum of disease than previous classifications and allows for determination of prognosis regarding spinal deformities,
ambulation,
and life span.
This classification also aids in the treatment of scolioses in affected individuals.
SKULL:
Skull radiographs reveal persistent Wormian bones and enlarged sinuses.
The calvaria is lucent and thin.
Platybasia is a frequent finding and may be accompanied by basilar impression.
Other findings include:
Multiple fractures,
often transverse and in the lower extremities,
are the radiographic hallmarks of osteogenesis imperfecta.
Subsequent healing with tumoral callus leads to shortening (the result of telescoping),
bowing deformities,
and pseudo-arthroses.
The excessive callus formation (called pseudo-tumors) has been mistaken for osteosarcoma.
Kyphoscoliosis is common,
resulting from ligamentous laxity,
osteoporosis,
and fracture deformity.
The vertebral bodies may be anteriorly wedged and often appear evenly flattened or biconcave (creating the biconcave lens vertebra).
Protrusio acetabuli may occur,
and a shepherd’s crook deformity of the proximal femur has been noted.
Premature degenerative joint disease results from ligamentous laxity and multiple fractures of the articular surfaces.
The differentiation of child abuse from osteogenesis imperfecta is generally readily accomplished based on other clinical findings.
However,
in those rare cases of type IV (perhaps Glorieux type V),
who present with no blue sclera and mild skeletal changes,
biopsy for collagen analysis may be helpful.
ACHONDROPLASIA
Achondroplasia,
the most common congenital dwarfism,
is an autosomal dominant disturbance in epiphyseal chondroblastic growth and maturation.
The name achondroplasia was first used in 1878 by Parrot.
Other synonyms that have been used include chondrodystrophia fetalis,
chondrodystrophic dwarfism,
and micromelia.
SKULL:
The base of the skull (which is formed by enchondral ossification) is small,
often with a stenotic foramen magnum.
Basilar impression is frequent.
The cranium is large,
though short in its anteroposterior (AP) dimension (brachycephaly).
The frontal bones are prominent and the nasal bones are small.
The mandible forms normally and,
therefore,
gives the impression of prognathism.
Other findings include:
LIMBS:
Symmetric shortening of all long bones,
with the proximal portions being most affected.
The bone ends are often splayed,
with metaphyseal cupping.
Because periosteal ossification proceeds normally,
there is relative widening of the shafts.
The ulna and tibia are often shorter than the radius and fibula.
The tubular bones of the hands and feet are short and thick.
The fingers are all the same length,
with separation of the middle and ring fingers (trident hand).
THORAX:
The ribs are quite short and often do not extend around the thorax.
The scapulae may be squared inferiorly,
with shallow glenoids.
PELVIS:
The entire pelvis is small.
The ilia are shortened caudally and flattened,
with small sciatic notches.
The acetabula are horizontally oriented,
and there is excessive thickening of the Y cartilage.
The pelvis assumes a characteristic champagne glass appearance.
SPINE:
The length of the spinal column is generally normal at birth,
though mild platyspondyly may be seen.
The amount of cartilage is increased,
causing the height of the discs to equal that of the vertebral bodies.
Posterior scalloping of the bodies is common.
The interpedicular spaces decrease caudally in the lumbar region,
whereas they increase from L1 to L5 in the normal individual.
The pedicles are short and thick.
The lumbar lordosis is often exaggerated,
complicated by a horizontally oriented sacrum.
An angular kyphosis often develops at the  thoracolumbar junction,
resulting from anteriorly wedged or bullet-nosed vertebrae.
thoracolumbar junction,
resulting from anteriorly wedged or bullet-nosed vertebrae.
CLEIDOCRANIAL DYSPLASIA
Cleidocranial dysplasia is an uncommon autosomal dominant disorder that affects 0.5/100,000 live births.
It is caused by a mutation on chromosome 6 and is characterized by faulty ossification of the intramembranous and enchondral bones.
Skull and clavicular anomalies,
as well as midline defects,
are classic features of this dysplasia.
According to Soule,
the first case was described by Cutter in 1870.
In 1898 the condition was recognized as an entity by Marie and Sainton and given the name cleidocranial dysostosis.
SKULL:
Early in infancy there is delayed or absent ossification of the calvaria.
With time,
multiple Wormian bones are formed in the sutures and often the metopic suture persists.
Widening of the principal sutures (sagittal and coronal) gives a hot cross bun appearance.
There is marked brachycephaly,
with a widened interparietal diameter.
The supraorbital region,
temporal squama,
and occipital bone are frequently thickened.
The foramen magnum is deformed and enlarged,
and there may be platybasia.
The small face is the result of underdeveloped facial bones.
Frequently,
the nasal bones fail to ossify,
and the paranasal sinuses are hypoplastic.
Although the maxilla is small,
the mandible is large and the mandibular suture closes late.
A high arched or cleft palate is not uncommon.
Delayed and defective dentition is a prominent and often symptomatic finding.
Dental panoramic radiography is effective in identifying features pathognomonic for cleidocranial dysplasia.
Other findings include:
THORAX:
Anomalous clavicular development is a nearly constant finding.
The clavicle is formed from three separate ossification centers (sternal,
middle,
and acromial).
Because one or more of these centers can be affected,
there is considerable variation in the clavicular involvement.
In 10% of cases the clavicle is completely absent.
A pseudo-arthrosis may develop when the middle portion is missing.
The scapulae are often small,
winged,
or elevated.
The shoulder girdle deformities allow great mobility of the shoulders.
While the ribs are usually normal,
the chest is narrow and cone shaped.
PELVIS:
The bones of the pelvis are small and underdeveloped,
forming a small pelvic bowl.
Commonly,
there is a midline defect at the pubic symphysis,
where the rami fail to approximate anteriorly.
Early coxa valgus develops into coxa varus,
possibly secondary to weight-bearing stresses on the poorly mineralized femoral neck.
Many patients with cleidocranial dysplasia have an unusual shape of the femoral head,
reminiscent of a chef’s hat.
Lateral notching of the capital femoral epiphysis has been reported.
SPINE:
The vertebrae often show delayed mineralization,
biconvex bodies,
and spina bifida occulta,
especially in the cervical and upper thoracic segments.
There is an increased incidence of spondylolysis in the lumbar spine.
Hyperlordosis,
excessive kyphosis,
and scoliosis are secondary to the neural arch defects and hemivertebrae.
EXTREMITIES:
The most marked changes are found in the hands,
where an accessory epiphysis for the base of the second metacarpal occurs,
creating an elongated digit.
The distal phalanges are hypoplastic and often pointed.
Similar changes may be found in the feet but are less common.
The long tubular bones are less frequently involved,
but occasionally shortening of the radius with an abnormal wrist articulation is seen.
HYPOPHOSPHATASIA
Hypophosphatasia is a heterogeneous disorder characterized by low or absent serum alkaline phosphatase activity caused by deficient activity of tissue-nonspecific alkaline phosphatase (TNSALP).
The gene for TNSALP is located at chromosome 1p34–36.1.
There are two modes of genetic transmission.
The congenital form is inherited as an autosomal recessive and is lethal.
The autosomal dominant form is milder and manifests later in life.
Hypophosphatasia typically appears as decreased ossification of the skull and vertebrae or as isolated plates or islands of unusually thin calvarial bone The skull may be boneless and represented by a caput membranaceum.
Other skeletal changes of hypophosphatasia include short tubular bones that are poorly and irregularly ossified and frayed metaphyses that resemble those of rickets.
THALASSEMIA
Thalassemia (Cooley’s anemia,
Mediterranean anemia) is the world’s most common hereditary disorder.
It is characterized by abnormal hemoglobin synthesis that produces variable degrees of anemia.
The first description was by Cooley and Lee in 1925.
The different genetic varieties of thalassemia produce a series of disorders known collectively as the thalassemia syndromes.
However,
three general groups have been identified,
classified according to the severity of the disease: thalassemia major,
thalassemia minor,
and thalassemia intermedia.
The most severe form is thalassemia major,
which has the poorest prognosis.
The effects on the skeleton can be severe and manifest radiographically as signs of increased marrow hemopoiesis.
SKULL:
Of all the anemias,
thalassemia creates the most pronounced changes in the skull.
In the calvaria,
there is a distinct lack of changes below the inferior occipital protuberance owing to the lack of marrow in this area.
The frontal bones reveal the earliest and most severe changes.
Three patterns of involvement may be visible: granular osteoporosis,
widened diploe,
and vertical radiating spicules of new bone (hair-on-end appearance) with loss of definition of the outer table.
Circumscribed lytic lesions of the calvaria up to 5 cm are occasionally seen.
The vascular impressions from the middle meningeal arteries are often enlarged and prominent.
In the facial bones,
the effects of erythroid hyperplasia may be severe,
a feature rarely seen in sickle cell anemia.
The major abnormalities are lack of pneumatization of the frontal,
maxillary,
sphenoid,
and mastoid air cells but not the ethmoids,
which remain aerated.
The orbits may be displaced laterally,
and the upper incisors may be displaced forward,
producing malocclusion (rodent facies).
Other findings include:
LONG BONES:
Manifestations of erythroid hyperplasia are best exemplified in the appendicular skeleton.
The medullary cavity is widened,
cortices are thinned,
and trabeculae are sparse but coarsened (honeycomb).
Nutrient foramina may be enlarged.
Generally,
the tubular bones are osteoporotic and lack the normal metaphyseal-diaphyseal concave constriction,
at times producing the Erlenmeyer flask deformity.
Organized medullary infarcts are uncommon,
in contrast to sickle cell anemia.
Partial premature closure of growth plates may be evident as deformity or alteration in length,
especially in the proximal humerus and distal femur.
Avascular necrosis of the femoral heads does occur,
although it is less common than in sickle cell anemia.
SPINE:
The most prominent changes in the spine consist of osteopenia,
coarse vertical trabeculae,
thin cortical outlines,
and involvement of both the body and neural arch of each segment.
These features will also be visible in the sacrum and pelvis.
Slight,
generalized concavity of the endplates may be visible,
but the discrete,
central endplate depression typical of sickle cell anemia is invariably absent.
Additional findings may include exaggeration of the anterior body vascular notch,
growth arrest lines,
enlargement of the dens,
and small ring apophyses.
It is notable that the spinal and pelvic lesions persist and even increase in prominence with increased age,
in contrast to regression of the peripheral bone changes.
Extra-medullary hematopoiesis affecting the spinal cord or nerve roots may exist but is rare.
MUCOPOLYSACCHARIDOSES
The mucopolysaccharidoses (MPS) are a group of inherited metabolic disorders that result in widespread skeletal,
visceral,
and mental abnormalities.
A defect in metabolic degradation leads to the storage of mucopolysaccharide macromolecules in the nervous system and other body tissues.
There is also excessive urinary excretion of mucopolysaccharides,
which are components of connective tissue.
Brante was the first to use the term mucopolysaccharidosis in 1952 while describing a patient with gargoylism.
Further investigation has shown that the absence of certain enzymes causes the clinical and radiologic features that characterize the mucopolysaccharidoses.
The MPS are classified into various types,
and there are additional diseases,
such as the mucolipidoses and a gangliosidosis,
that demonstrate similar clinical and radiologic findings.
McKusick classified these entities into six distinct syndromes:
- MPS-I (MPS-I-H): Hurler’s syndrome.
MPS-I-S: Scheie’s syndrome.
MPS-I-H-S: Hurler-Scheie syndrome.
- MPS-II: Hunter’s syndrome.
- MPS-III (subtypes A,
B,
C,
and D): Sanfilippo’s syndrome.
- MPS-IV: (subtypes A and B) Morquio’s syndrome.
- MPS-VI: Maroteaux-Lamy syndrome.
- MPS-VII: Sly’s syndrome.
MPS-I: HURLER’S SYNDROME
Hurler’s syndrome is a rare autosomal recessive disorder of mucopolysaccharide metabolism that leads to excessive lipoid accumulation in the central nervous system and other viscera.
It occurs in approximately 1/100,000 births.
The excessive mucopolysaccharides excreted in the urine are dermatan sulfate and heparin sulfate.
Synonyms include lipochondrodystrophy,
gargoylism,
osteochondrodystrophy,
and dysostosis multiplex.
Hurler’s syndrome represents the classical prototype of mucopolysaccharide disorder.
SKULL:
Changes seen in the skull include macrocephaly,
frontal bossing,
calvarial thickening,
and premature closure of the sagittal and lambdoid sutures.
Hydrocephalus is common.
The sella turcica is enlarged and J shaped.
Often,
the facial bones are small and the mandibular angle is widened.
Other findings include:
SPINE:
Spinal changes are fairly typical.
A thoracolumbar kyphosis develops secondary to vertebral body hypoplasia.
The lower thoracic and upper lumbar bodies are small in their anterosuperior aspect and may be beaked inferiorly.
The remaining vertebral centra may be oval owing to convexity of the upper and lower surfaces.
The pedicles are often long and slender.
Atlantoaxial subluxation has been reported as well as upper cervical instability.
THORAX:
The ribs are overly wide,
with tapered ends,
producing a paddle or spatulated appearance.
The ilia are flared,
with obliquely directed acetabular roofs.
Coxa valga or vara is common.
Varus deformity of the humerus is characteristic.
LONG BONES:
The tubular bones have widened diaphyses; this is more obvious in the upper extremities than in the lower.
Often,
the metacarpals and phalanges are short and wide,
producing a trident hand.
Osteoporosis is a frequent finding.
Differential diagnosis from Morquio’s syndrome is easily accomplished by observing the spinal differences,
as well as the lack of hepatosplenomegaly in MPS-IV patients.
While some resemblance to achondroplasia exists,
the Hurler’s syndrome patient is normal at birth,
and achondroplasia is easily discerned in the infant.
HISTIOCYTOSIS X
Histiocytosis X is a disease of unknown origin that encompasses a wide spectrum of clinical,
pathologic,
and radiologic features.
The hallmark of the disease is an abnormal proliferation of reticuloendothelial cells,
predominantly the histiocyte from which the disease derives its name.
The term histiocytosis X was first proposed by Lichenstein in 1953.
In more recent times a name change to Langerhans’ cell histiocytosis has been suggested because Langerhans’ cell is the major cell type.
The disease is a disorder of immune regulation rather than a neoplastic process and may occur as a solitary lesion,
primarily affecting the bones,
or be a multisystem entity.
The skin is affected in 40% of cases,
and in 10% of cases,
skin lesions represent the only manifestation.
The typical skin manifestations include papules,
vesicles,
nodules,
erosions,
ulcerations,
crusting,
and/or purpura.
The disease is generally considered a childhood or juvenile disease but may progress into adult life
Three entities are encompassed under this term: Letterer-Siwe disease (10%),
Hand-Schüller-Christian disease (15-40%),
and eosinophilic granuloma (60-80%).
Although these are designated as separate entities,
they frequently overlap and may transform into each other.
The only laboratory findings may be a slightly elevated erythrocyte sedimentation rate (ESR)—20-50 mm at 1hr—and a slight leukocytosis.
EOSINOPHILIC GRANULOMA
Eosinophilic granuloma is the least severe but most common (60-80%) of all the histiocytoses.
Peak incidence comes between the ages of 5 and 10 years,
and 75% of cases occur in individuals < 20 years of age.
Symptoms primarily are localized pain and swelling of < 2 months’ duration.
Eosinophilic granuloma typically lacks the systemic features of Hand-Schüller-Christian or Letterer-Siwe disease.
Occasionally,
pathologic fracture will be the presenting problem.
Vertebral involvement is characterized by pain,
and in some cases complicating myelopathy may ensue secondary to cord and nerve root compression.
Temporal bone involvement may produce otitis medialike symptoms,
and the diagnosis of eosinophilic granuloma should be suspected when patients with suspected otitis media do not respond to traditional medical treatment.
More than 50% of cases involve the skull,
mandible (25%),
spine (6%),
pelvis (20%),
and ribs (7%).
Of the long bones,
the femur (15%),
tibia,
and humerus (8%) are involved most often.
The bones of the hands and feet are affected rarely.
Monostotic presentations are three times more common than polyostotic presentations.
Monostotic lesions progress to lesions elsewhere in 20% of cases.
Pain may be the primary symptom,
and the diagnosis often requires histopathologic analysis of the lesions as well as the detection of S-100 CD1 antigens on imunohistochemical analysis of the tissues.
Response is usually excellent,
with little difference in outcome no matter what method is employed and even without treatment.
Radiotherapy or injection into the lesion of corticosteroid can enhance healing of the lesion.
Removal by either en-bloc excision or curettage is curative.
Chemotherapy is sometimes employed in polyostotic forms.
The time for healing to occur is usually 6-24 months; however,
reoccurrence may occur and is more common in adults than in skeletally immature patients.
Spinal lesions usually do not require treatment,
unless the cord is affected.
SKULL AND MANDIBLE
A round to oval osteolytic lesion of 1-4 cm is characteristic.
It is sharply demarcated and may involve one table greater than the other to produce a double contour (beveled edge sign,
hole within hole).
Within the lesion a central focus of bone may remain isolated,
which may be identified only on CT examination (button sequestrum).
The lesion does not respect suture lines and readily infiltrates into adjacent parts of the calvaria.
In the mandible,
pain is the primary symptom in 92% of cases.
Radiographically,
the lesion is osteolytic,
may be expansile,
and does not involve the teeth except to leave them displaced and isolated (floating teeth sign).
Early lesions typically begin in the vicinity of the last molar and enlarge predominantly forward but do not destroy the lower mandibular border.
Other findings include:
SPINE:
More than 50% of cases involve the thoracic spine; 35%,
the lumbar spine; and < 15%,
the cervical spine.
Solitary vertebral involvement is more common,
though multiple levels are occasionally involved.
With cervical involvement,
C2 is the primary target in adults,
whereas the middle cervicals are normally affected in children.
The vertebral body is usually involved with relative sparing of the neural arch structures.
In contrast,
cases have been reported of lesions affecting the posterior arch and lateral masses in the absence of vertebral body involvement; however,
this is rare.
An osteolytic lesion is the expected radiographic appearance.
Neural arch involvement,
when present,
destroys the internal matrix but preserves the cortical outline,
which has been described as a ghostly appearance.
The most prominent feature in the lumbar and thoracic spine is pathologic fracture,
with dramatic loss of vertebral height as thin as 2 mm involving both the anterior and posterior vertebral body surfaces (vertebra plana,
silver dollar vertebra,
coin-on-edge vertebra).
This is rare in the cervical spine.
Areas of destruction within the centrum may be observed before collapse.
A short-segment kyphosis usually accompanies thoracic vertebral involvement.
Paravertebral swelling can be prominent and is more likely to be associated with increased risk to the cord.
On CT examination osteolytic destruction can be seen,
which simulates aggressive neoplasm; occasionally a sequestrum may be visible.
Bracing is the treatment of choice,
and surgical intervention is rarely necessary.
Restoration of height with healing is to be expected in at least 90% of cases and can be rapid over 1 year.
The majority of cases reconstitute to 48-95% of normal height,
especially in patients < 15 years of age at the time of onset.
Residual sclerosis and trabecular accentuation always remain.
Rarely,
interbody fusion may occur after radiotherapy,
and occasionally there is a bone-within-bone appearance.
Healed lesions do not appear to increase the risk for long-term back disability in adulthood.
PELVIS:
The ilium is the most frequent component afflicted,
especially within the supra-acetabular region.
The lesion can be relatively large,
slightly expansile,
and usually exhibits a sclerotic beveled edge.
Initially,
small moth-eaten-permeative, multiple lesions may be seen,
which rapidly become confluent,
producing large geographic defects.
Invasion across the triradiate cartilage is unusual.
In the pubis,
the lesions are smaller and can be associated with a laminated periosteal response along the superior pubic ramus.
Ischial lesions similarly may provoke periosteal new bone.
multiple lesions may be seen,
which rapidly become confluent,
producing large geographic defects.
Invasion across the triradiate cartilage is unusual.
In the pubis,
the lesions are smaller and can be associated with a laminated periosteal response along the superior pubic ramus.
Ischial lesions similarly may provoke periosteal new bone.
HYPOTHYROIDISM
Hypothyroidism in the newborn (cretinism) exerts a considerable growth and developmental-inhibiting factor to the skeleton.
Manifestations of cretinism include delayed closure and fragmented epiphyses (cretinoid epiphyses),
occasional wormian bones,
and a wedged thoracolumbar sail vertebra.
Bilateral slipped capital femoral epiphysis,
although rare,
has been associated with hypothyroidism and other endocrinopathies.
CROUZON SYNDROME
Is an autosomal dominant genetic disorder known as a branchial arch syndrome.
Specifically this syndrome affects the first branchial arch,
which is the precursor of the maxilla and mandible.
Since the branchial arches are important developemental features in a growing embryo,
disturbances in their development create lasting and widespread effects.
This syndrome is named after Octave Crouzon,
a French physician who first described this disorder.
Now known as Crouzon syndrome,
the disease can be described by the rudimentary meanings of its former name.
What occurs in the disease is that an infant’s skull and facial bones,
while in the development,
fuse early or are unable to expand.
Thus,
normal bone growth cannot occur.
Fusion of different sutures leads to different patterns of growth of the skull.
TUBEROUS SCLEROSIS
Tuberous sclerosis is a rare,
autosomal dominant,
multisystem disorder of neuroectodermal origin.
The disorder is often associated with a chromosome 9 abnormality,
although up to 60% of cases occur spontaneously.
Tuberous sclerosis occurs in 1/100,000 to 1/10,000 births.
It belongs to a unique group of diseases known as the phakomatoses.
This group of neuroectodermal disorders is characterized by tumors of the skin and central nervous system.
The most frequently seen phakomatosis is neurofibromatosis.
Tuberous sclerosis was first described by von Recklinghausen in 1862.
Bourneville,
in 1880,
coined the term tuberous sclerosis after providing a detailed description of the clinicopathologic features.
Myriad clinical and radiographic features have been reported in association with this disorder.
The classic clinical triad consists of mental retardation,
epileptic seizures,
and skin lesions,
but one or more of these characteristics may be lacking.
Synonyms include Bourneville’s disease
SKULL:
Intracerebral calcifications are found on x-ray examination in 50-80% of cases.
The most common locations are in the basal ganglia and paraventricular regions.
The incidence increases with the patient’s age.
Cortical tubers and subependymal nodules (hamartomas) are common near the ventricles and may calcify.
The calcifications may be multiple or singular and appear as discrete nodules or,
occasionally,
as linear conglomerates.
Cerebellar calcifications are found in 10-15% of patients.
( 15,
15, 16) MRI has enhanced the ability to detect otherwise unseen brain lesions.
(
16) MRI has enhanced the ability to detect otherwise unseen brain lesions.
( 7) The MRI appearance of intracranial manifestation in tuberous sclerosis varies with age.
7) The MRI appearance of intracranial manifestation in tuberous sclerosis varies with age.
 Skeletal lesions occur in approximately 50% of cases and have a varied presentation.
In addition to the intracranial calcifications,
generalized thickening and hyperostosis of the cranial vault may be evident.
The multiple cortical tubers are a hallmark of tuberous sclerosis complex.
Skeletal lesions occur in approximately 50% of cases and have a varied presentation.
In addition to the intracranial calcifications,
generalized thickening and hyperostosis of the cranial vault may be evident.
The multiple cortical tubers are a hallmark of tuberous sclerosis complex.
CUTANEOUS MANIFESTATIONS:
The most widely recognized skin change is adenoma sebaceum (a hamartoma),
which is present in 80-90% of cases.
This is frequently evident in childhood but may not manifest until puberty or pregnancy.
The earliest skin manifestations are thought to be hypopigmented macules that occur on the legs and trunk.
These are oval or leaf-shaped,
with irregular margins,
and may be evident at birth.
The presence of hypopigmented macules in infants makes the diagnosis of tuberous sclerosis probable,
while their occurrence with seizures makes it highly probable.
Other cutaneous lesions include café au lait spots,
shagreen,
or peau-chagrin patches (20-50% of cases),
gingival and periungual fibromas,
and skin tags.
Ocular abnormalities such as retinal phakomas (white patches) are seen at birth in ~ 52% of cases.
Other findings include:
LONG BONES:
The tubular bones of the hands and feet frequently have cortical manifestations.
Irregular subperiosteal new bone formation and nodules are common.
Small,
well-defined cysts are seen in the small tubular bones of the hand,
particularly in the distal phalanges.
The trabecular pattern may be coarsened.
SPINE:
The spine and innominate bones are often involved,
with osteoblastic deposits of varied size and contour.
The reactive new bone may be in response to osseous hamartomas .
.
The areas of increased density may be diffuse or seen as discrete islands and are most common in the vertebral bodies and pedicles and along the pelvic brim.
The regions of increased density on plain radiographs correspond to regions of increased uptake on bone scintigraphy.
Cortical excrescences affecting the tibia in tuberous sclerosis patients have been referred to as periosteal warts.
Enlargement and sclerosis of a rib has been reported in association with tuberous sclerosis.
In a series of 12 patients with tuberous sclerosis,
6 had scoliotic curves ranging from 12° to 78°.
VISCERAL:
The fatty component of most renal hamartomas may allow for their detection on plain radiographs,
accompanied by kidney enlargement and contour irregularities.
When present,
the interstitial changes that occur in the lungs are apparent radiographically.
Complications of tuberous sclerosis include urinary tract infection,
pulmonary disease (e.g.,
pneumothorax,
hemoptysis,
dyspnea,
aspiration pneumonia),
cor pulmonale,
and neoplastic degeneration of the hamartomatous lesions.
HEMANGIOMA
Hemangioma,
a primary benign neoplasm,
is a slowly growing lesion of bone composed of newly formed capillary,
cavernous,
or venous blood vessels.
Most lesions are clinically silent.
Hemangiomas represent about 1% of all primary bone tumors and 2-3% of all radiographically perceptible spinal tumors.
Schmorl and Junghans found asymptomatic vertebral hemangiomas in 11% of 3829 consecutive,
serially sectioned vertebral columns removed at autopsy.
Many of these lesions are not demonstrated on radiographs but are frequently seen on MRI.
Hemangioma is the most common benign bone tumor of the spine.
SKULL:
Although hemangioma may occur anywhere in the skull,
it is most commonly found in the frontal bone.
The lesion varies from 1 to 7 cm in diameter and is a round or oval radiolucency when viewed en face.
The lytic defect often has dense,
fine spicula radiating from its centrum,
creating a sunburst or spoked-wheel appearance.
The intense nature of the radiating spicules of bone can mimic osteosarcoma,
particularly in tangential or profile views.
Ordinarily,
the hemangioma extends outward,
well beyond the normal contour of the bone.
Often accompanying this external bulging is an erosion or disappearance of the outer table of the skull,
while the integrity of the inner table is usually preserved.
The profile view frequently discloses vertical striations,
which produce the characteristic sunray effect.
GROWING FRACTURE
Growing skull fracture is a rare complication of head injury in which 90% of the cases occur among children less than 3 years old.
There is progressive enlargement of the skull fracture,
generally with involvement of the underlying brain in the defect with resultant neurologic symptoms.
The lesion is thought to arise from a skull fracture with an associated dural tear,
almost always occurring during childhood.
As a result,
repeated pulsations of brain and CSF are thought to cause erosion of adjacent calvarial margins.
Although the exact reason for the nearly exclusive occurrence in the young pediatric age group is not known,
active skull growth as well as firm attachment of dura to the skull are probably responsible.
The defect is typically irregular in contour and elliptical in shape.
These lesions generally exhibit scalloped margins and some degree of sclerosis of the adjacent bone; both inner and outer tables are involved,
the inner table to a greater extent.
In some instances,
the old fracture line may be clearly seen at either end of the elliptical defect.
NEUROCYSTICERCOSIS
The larval form of the pork intestinal tapeworm Taenia solium is the agent responsible for NCC.
Humans are the definitive host for T.
Solium and usually harbor the adult tapeworm in the small intestine as an asymptomatic infestation.
Fecal shedding of eggs by the definitive host (i.e.
man) leads to ingestion of eggs- usually in contaminated food or water-by the intermediate host,
typically pig or man.
Once inside the intestinal tract the eggs are released and produce oncospheres,
the primary larvae.
These larvae bore the intestinal mucosa and enter the circulatory system.
Hematogeneous spread to neural muscular and ocular tissue occurs.
Once inside the brain,
the oncospheres develop into secondary larvae the neurocystcerci.
Because pathologic findings vary with lesion stage,
these are discussed in concert with imaging manifestations of NCC.
The brain parenchyma is the most commonly affected site in NCC,
seen in more than half of all cases.
The cortico-medullary junction is the primary location.
Intraventricular cysticercosis cysts are seen in 205 to 505 of the cases.
With the fourth ventricle a common site.
Only 105 of NCC cases have isolated sub arachnoid disease.
More than one anatomic compartment is often involved.
Morbidity with NCC results from dead larvae that typically incite an intense host inflammatory response.
NCC has a broad spectrum of clinical manifestations.
Epilepsy is the most frequent symptom and is seen in 50% to 70% of cases.
The pathologic manifestations of parenchymal neurocysticercosis have been classified into the following four stages: vesicular,
vesicular colloidal,
granular nodular and nodular calcified.
TORCH Spectrum
Congenital TORCH infections are acquired transplacentally in utero or during birth.
Congenital cytomegalovirus infection is associated with microcephaly,
microgyria,
and intracranial calcifications.
Affected infants are small for dates and present with petechial rash,
hepatosplenomegaly,
chorioretinitis,
deafness,
and developmental delay.
Babies who acquire a TORCH infection at birth are not yet microcephalic; microcephaly at birth signifies an earlier infection in utero.
Congenital rubella is associated with cataracts,
middle ear and cardiac malformations,
and skeletal features such as metaphyseal linear “celery stalk” striations.
Congenital rubella and other TORCH infections are now rare because of childhood immunization and prenatal screening.
CRANIOPHARYNGIOMA
Craniopharyngioma is a histologically benign,
extra-axial,
slow-growing tumor that predominantly involves the sella and suprasellar space.
Despite its histologic appearance,
craniopharyngiomas occasionally behave like malignant tumors.
They can metastasize,
and patients can have severe symptoms that usually require surgery and/or radiation therapy (with intracystic chemotherapy in some pediatric patients).
Recurrences,
both local and along surgical tracts,
have been reported,
as has meningeal seeding.
Characteristic radiographic findings help in differentiating craniopharyngiomas from other tumors that can occur in the same anatomic region.
Zenker first described craniopharyngioma in 1857.
A lateral radiogram of the skull may demonstrate calcifications in either the sella turcica or suprasellar space (see the first image below),
or it may demonstrate sellar expansion or erosion of clinoid process or dorsum sella.
These calcifications can be confused with curvilinear calcifications observed with large aneurysms (occasionally referred to as eggshell calcifications).
An aneurysm may be differentiated on contrast-enhanced CT,
which demonstrates characteristic enhancement of the remainder of the lumen of the aneurysm,
and on MRI,
which shows heterogeneity of signal intensity and misregistration artifact from turbulent or pulsatile flow in the aneurysm.
MRA further helps to elucidate the diagnosis in questionable cases.
The degree of confidence for a negative result is low because small calcifications can be missed easily.
When observed,
calcifications are a nonspecific finding.
Soft tissue visualization on plain radiography is poor; therefore,
differentiation of the type of tumor present is not possible without further imaging.
LEUKEMIA
Acute leukemia is the most common malignancy in children that comprises about 41% of the malignancies in children younger than 15 years old.
It is the second most common malignancy in children under one-year-old.
Acute lymphocytic leukemia (ALL) is the most common malignancy under 15 years age.
ALL is responsible for approximately 23% of all cancers and 76% of leukemia in this age group.
However,
only 20% of acute leukemia in adults is ALL.
The peak age of involvement is 2-6 years and boys are slightly more involved than girls.
Chromosomal abnormalities such as Down,
Bloom and Fanconi Syndrome and also ataxia telangiectasia are prone to this malignancy.
Although leukemia may present with pallor,
petechia,
ecchymosis in skin and mucus membranes,
growing skeleton is an important site for proliferation of leukemic cells; therefore,
during the course of disease,
tenderness and multiple areas of bone destruction and repair due to infiltration of leukemic cells in the bone marrow may be seen.
More common radiographic findings which have been reported in the literature are generalized reduced bone density,
metaphyseal lucent band,
lytic bone lesions,
metaphyseal cortical bone erosions,
collapsed vertebra and widening of sutures and periosteal reactions which have been seen in our cases with variable frequencies
SKULL:
The skull has been an uncommon site of involvement; however,
periosteal reaction and osteolytic lesions have been reported at various ranges by different investigators 4-11% for periosteal reaction and 13-23% for osteolytic lesions.
HYPERPARATHYROIDISM
Hyperparathyroidism is the general term applied to overactivity of the parathyroid gland,
of which there are many causes.
The gland’s mode of action is primarily related to the release of the strong osteoclastic hormone parathormone (PTH).
The skeletal effects are widespread and frequently specific enough for a definitive radiologic diagnosis to be given.
There are three basic forms of hyperparathyroidism: primary,
secondary,
and tertiary.
Primary hyperparathyroidism:This is the most common cause of hypercalcemia and may be owing to a parathyroid adenoma (90% of cases),
carcinoma,
hyperplasia,
or ectopic tumors,
producing a parathormone type of substance.
Characteristically,
there are elevated levels of parathormone,
hypercalcemia,
and hypophosphatemia.
Secondary hyperparathyroidism:This is one of the most common complications of chronic renal disease,
allowing for persistent loss of calcium and phosphorous and thus stimulating parathormone release.
Tertiary hyperparathyroidism: In dialysis patients,
the parathyroid gland may act independently of serum calcium levels.
RADIOLOGIC FEATURES:
The radiologic differentiation between primary and secondary hyperparathyroidism is usually not possible.
In the era previous to dialysis therapy,
brown tumors were more common in the primary form,
but they are now found just as commonly in the secondary variety owing to the increased life span of the patient.
One notable difference is the greater tendency to produce osteosclerosis in the secondary form.
GENERAL FEATURES
BONE:
The major changes consist of bone resorption with decreased density,
accentuated trabecular pattern,
loss of cortical definition,
subperiosteal resorption,
and brown tumors. Additional infrequently encountered features include pseudo-fractures,
fractures,
and deformities.
SUBPERIOSTEAL RESORPTION:
Stimulation of the inner periosteal layer precipitates bone resorption in predictable locations.
This is the single most definitive radiologic sign of hyperparathyroidism.
The most characteristic sites include the radial margins of the middle and proximal phalanges of the second and third digits of the hand,
medial metaphysis of the humerus and tibia,
undersurface of the distal clavicle,
trochanters,
and tuberosities.
This outer cortical erosion produces an irregular,
frayed,
and lace-like appearance of the external bone surface.In addition,
resorption of subarticular bone produces apparently widened joint spaces and osteolysis,
particularly at the acromioclavicular,
symphysis pubis,
and sacroiliac articulations.
DECREASED BONE DENSITY:
All skeletal structures show diffuse rarefaction.
The bones can appear quite granular,
as best seen in the skull (salt and pepper or pepper pot skull).
ACCENTUATED TRABECULAR PATTERNS:
As non-essential trabeculae are resorbed,
those that remain will appear more prominent.
LOSS OF CORTICAL DEFINITION:
A combination of endosteal,
intracortical,
and subperiosteal resorption produces a cortex that lacks the normal radiologic borders.
The cortex and medullary cavity merge imperceptibly into each other,
whereas the outer surface appears blurred and often irregular.
Evidence of intracortical resorption within Haversian canals is seen especially in the second metacarpal cortex,
where subtle longitudinal striations can be observed.
SUBLIGAMENTOUS BONE RESORPTION:
At attachments of ligaments and tendons,
focal resorption of cortical bone can be observed.
The most frequent sites are at the trochanters,
humeral and ischial tuberosities,
inferior aspect of the distal clavicle,
and inferior surface of the calcaneus.
BROWN TUMORS (OSTEOCLASTOMA):
Brown tumors are visible as distinct geographic radiolucencies.
They are usually central,
slightly expansile,
and lightly septated,
mimicking a destructive neoplasm.
These may heal,
as evidenced by their dense sclerotic appearance.
The most common sites of occurrence include mandible,
pelvis,
ribs,
and femora,
although any bone can be affected.
Brown tumors are usually a marker of primary hyperparathyroidism,
though now they can be encountered in the secondary form.
Although brown tumors are rare,
MRI investigations of brown tumors may reveal a fluid-fluid level.
JOINTS:
A destructive arthropathy—dialysis-related arthropathy (DRA)—involving the axial and appendicular joints can complicate long-term dialysis.