The demographic and clinical features of the study group are presented in Table 1 .
Almost a third of the patients presented with clinical signs of cholangitis; in this subset,
7 patients had no US signs of biliary tract dilatation,
but presented with jaundice and fever.
According to the imaging diagnosis, we divided our group in patients with anastomotic strictures (n=25) and patients with non anastomotic strictures (n=9).
Biliary anastomotic strictures were more frequently found in patients with bilioenteric anastomosis (8/12 cases).
PTBD was succesfully placed in 32 cases in the first session,
in 2 cases a second attempt was necessary in 5-7 days.
In n=3 patients,
the passage through the stricture was not achieved (even with multiple internalization attempts),
hence an external drain was placed- see Fig. 4
In the n=31 cases with internal/external drainage,
a definitive solution for the treatment of the strictures was attempted.
Hence,
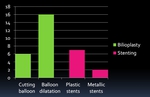
n=22 patients followed several dilatation sessions (mean 5; min 4-max 8 sessions),
of which 6 patients with cutting balloon and 16 with dilatation balloons.
In the other n=9 cases,
a stent was placed: plastic stents with ERCP rendezvous technique (n=7) and bare metalic stents (n=2) (see Table 2 ).
A case with bare metallic stent is presented in Fig. 5 and a patient which benefited from ERCP rendezvous technique is presented in Fig. 6 ; a pediatric case with cutting balloon dilatation is presented in Fig. 7 .
The 6 month and 1 year reccurency rates are presented in Table 3 .
The aggregate 6 months and 1 year reccurency rate in the bilioplasty group was 32% and 45% respectively; in the stenting group was 0% at 6 months and 33% at 1year.
Catheter displacement with choleperitoneum (n=4) was the most frequent complication,
which necessitated catheter repositioning and upsizing (8-10F catheters)- see Fig. 8 .
Other complications encountered were hemobilia (n=2 cases),
which required only conservative treatment and 1 case of septic shock.
Discussions
• The risk of occurrence of a specific biliary complication is related to the type of biliary reconstruction performed at the time of liver transplantation,
so a thorough knowledge of the anatomy is essential to the procedure’s success (1). The coledoco-coledocian anastomosis (duct-to duct) is the most common biliary reconstruction procedure performed during OLT; the procedure is technically easier,
it preserves the function of Sphincter of Oddi and allows easy endoscopic access to the biliary system after the surgery.
Also the use of T-tubes is controversial,
since it has been associated with bile leak and cholangitis at the time of their removal.
The bilioenteric anastomosis is usually recommended in patients with pre-existing biliary disease (such as primary sclerosing cholangitis,
or prior biliary surgery) when there is a size mismatch between donor and recipient ducts; it also is a contraindication to ERCP due to lack of access (2,3).
In our study there was predominance of the duct-to-duct anastomosis (favored in both OLT and LDLT)
• By comparison with OLT,
complication rates (from bile leaks and strictures) are higher with LDLT (high as 35% in certain series).
The biliary leaks reported in LDLT are from the cut surface and at the site of the anastomosis and the incidence ranges from 10 to 25%.
(4) The incidence of strictures ranges from 8 to 35%.
Preservation of the liver beyond 12 hours may result in a higher incidence of diffuse or non anastomotic strictures (5). In our study,
the incidence of biliary strictures was comparable to the previously published studies
• Although the biliary catheter itself maintains the patency of the anastomosis while allowing repeated access to the stricture for evaluation and dilatation,
due to high rate of complications and lack of patient compliance,
a definitive solution is needed (6).
These catheters also offer an advantage in management of strictures complicated by significant debris,
as daily flushing can get rid of most debris.
In patients who develop cholangitis,
the catheter can be opened for gravity drainage to allow external decompression of the biliary system and resolution of symptoms (7).
• Although a low sample size was used,
our study shows the superiority of stent placement over bilioplasty; of course a larger sample and longer evaluation intervals are needed for a better evaluation of the response.
Li et al (8) have shown that PTBD with stenting and bilioplasty have good results on long term followup (mean followup 452 days),
with less efficacy in the treatment of multifocal nonanastomotic strictures which are better treated with retransplantation
• In our study,
several patients had non dilated biliary tree,
which proved to be a technical challenge,
due to the added dificulty of accesing the biliary tract.
In general,
due to ischemic fibrosis,
the technical difficulty of biliary punctures is increased (9).
The complications met in our study group were mostly related to catheter depositioning (due to patient noncompliance) and one case of septic shock in a patient with severe cholangitis.
• There are several factors impacting the succes of the interventional techniques,
such as prolonged ischemia which can lead to rapid biliary complications,
often severe.
In these cases a quick diagnosis and treatment of these cases (with endovascular or surgical techniques),
lead to a significant decrease in morbidity (10).
Other limiting factors are the presence of non anastomotic strictures,
which require the placement of several drainage catheters and treatment of the local and general septic complications (11).
The development of chronic biliary sepsis and calculous disease further hinder the success of our treatment (12).