Patients:
Between 1st of January 2011 and 1st of January 2015,
in the Fundeni Clinical Institute,
225 liver transplantations were performed.
We analyzed retrospectively the clinical data,
imaging findings and interventional radiology protocols of 34 consecutive patients with biliary strictures or cholangitis following LT,
treated with percutaneous interventional techniques.
The mean age was 47 years (range 3-62 years),
with 21 male patients included (male:female ratio= 1:1,6).
In our study group,
living donor split grafts (n=23) or deceased donor grafts were performed (n=11).
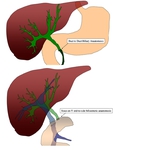
The biliary anastomosis was either duct-to duct(n=19) or bilio enteric (Y en Roux anastomosis) (n=15) Fig. 1.
In our study group,
the most frequent indication for transplantation was liver failure due to viral or alcoholic cirrhosis (n=25),
with 1 case known with primary biliary cirrhosis.
Definitions:
Biliary stricture was diagnosed when the stenosis of the bile duct and the dilatation of the intrahepatic duct proximal to the stricture were observed on magnetic resonance cholangiography (MRCP),
and the liver biochemical parameters,
such as serum bilirubin,
γ-glutamyltransferase,
and alkaline phosphatase were abnormal,
whether or not the patient had symptoms of abdominal pain and fever.
A nonanastomotic biliary stricture was diagnosed when the intrahepatic bile ducts proximal to the anastomotic site show strictures or irregularities,
with coresponding clinical and biochemical parameters sugesting cholangitis.
The reccurence of the biliary complications was defined as reccurence of clinical symptoms (jaundice,
cholestasis),
associated with imaging findings suggestive of biliary strictures or cholangitis.
The end point of the percutaneous transhepatic biliary drainage (PTBD) was placement of an internal drainage,
followed by definitive repair with bilioplasty (dilatation or cutting balloon) or stent placement.
The patients were followed for a mean period of 1 year after suppression of the biliary drainage.
Investigation protocol:
All patients with clinical signs of cholestasis were reffered to ultrasound imaging to determine the presence of a mechanical obstacle or to define the presence of an arterial hepatic thrombosis.
In the presence of biliary dilatation,
the patients were reffered to magnetic resonance cholangio pancreatography (MRCP) or to endoscopic retrograde cholangio pancreatography (ERCP); in case of failure of ERCP,
a direct percutaneous cholangiography was performed to asses the biliary complications Fig. 2.
Percutaneous transhepatic cholangiography protocol
- Conscious sedation
- 10 mL of 1% lidocaine HCl was locally infiltrated at the skin surface of the prepared puncture site.
- Ultrasound guided puncture of the biliary tree (either right or left branches),
using a 21G Chiba needle,
followed by injection of contrast media; a 0.018-inch microwire is passed in the biliary tree,
which is used for the placement of a 5 F sheath and a 0.035-inch hydrophilic guidewire is introduced.
- Navigation with a 4F RDC catheter (Cook) through the stenosis and placement of a stiff Amplatzer type guidewire,
progressive dilatation with 6 and 8F dilatators with placement of an internal-external 8,5F drain (Cook).
If the stricture is not passed,
an 8F external drain is placed and 2 weeks after a new procedure for internalization of the drain was scheduled.
- 2 weeks after succesful placement of the internal drainage,
bilioplasty sessions were started or stenting was performed (either percutaneously or with ERCP rendez vous technique). The bilioplasty sessions were performed with either cutting balloons (Flextome- Boston Scientific,
4x10mm) or with regular dilatation balloons (Cook,
8x10mm).
The stents were either plastic or bare metal.
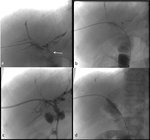
A typical placement of a percutaneous transhepatic biliary drainage,
followed by dilatation sessions is presented in Fig. 3.
Exclusion criteria:
- Irreversible coagulopathies (INR >1,5,
PLT<50.000)
- Renal failure (serum creatinine >2mg/dl)
- Presence of ascites