Aims and objectives
Still considered the Achiles heel in hepatic transplantation,
biliary complications canremain a major source of morbidity.
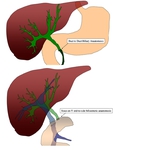
Biliary strictures (which can be either anastomotic or non anastomotic) can be treated percutaneously or via endoscopy (in selected cases),
decreasingthe need for subsequent surgical intervention.
Our main objective was to determine the efficacy and long term results of percutaneous treatment in patients with biliary strictures or cholangitis following liver transplantion (LT) and to establish the suitable interventional therapeutic modality forthese patients
Our secondary objectives were the presentation of...
Methods and materials
Patients:
Between 1st of January 2011 and 1st of January 2015,
in the Fundeni Clinical Institute,
225 liver transplantations were performed.
We analyzed retrospectively the clinical data,
imaging findings and interventional radiology protocols of 34 consecutive patients with biliary strictures or cholangitis following LT,
treated with percutaneous interventional techniques.
The mean age was 47 years (range 3-62 years),
with 21 male patients included (male:female ratio= 1:1,6).
In our study group,
living donor split grafts (n=23) or deceased donor grafts were performed (n=11).
The biliary anastomosis...
Results
The demographic and clinical features of the study group arepresented in Table 1 .
Almost a third of the patients presented with clinical signs of cholangitis; in this subset,
7 patients had no US signs of biliary tract dilatation,
but presented with jaundice and fever.
According to the imaging diagnosis, we divided our group in patients with anastomotic strictures (n=25) and patients with non anastomotic strictures (n=9).
Biliary anastomotic strictures were more frequently found in patients with bilioenteric anastomosis (8/12 cases).
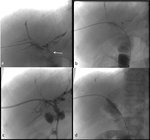
PTBD was succesfully placed...
Conclusion
PTBD followed by bilioplasty or stenting can be a viable option in the treatment of biliary complications after LT,
increasing the quality of life and decreasing the associated morbidities.
Low complication rates,
make these procedures safe to perform in these patients,
but the added dificulty of the posttransplantation setting increases the difficulty of the initial procedures.
An accurate and rapid imaging diagnosis is essential to the treatment options available.
Personal information
Radu Dumitru- assistent lecturer,
phD,
senior radiologist
SPITALUL CLINIC FUNDENI BUCURESTI
ROMANIA,
Bucharest,
Sos.
Fundeni nr.258,
sector 2
[email protected]
References
1. Buis CI,
Verdonk RC,
Van der Jagt EJ,
et al.
Nonanastomotic biliary strictures after liver transplantation,
part 1: Radiological features and risk factors for early vs.
late presentation.
Liver Transpl.
2007;13:708–718.
2. Pascher A,
Neuhaus P.
Biliary complications after deceaseddonor orthotopic liver transplantation.
J Hepatobiliary Pancreat Surg.
2006;13:487–496.
3. Guichelaar MM,
Benson JT,
Malinchoc M,
Krom RA,
Wiesner RH,
Charlton MR.
Risk factors for and clinical course of nonanastomotic biliary strictures afterliver transplantation.
Am J
Transplant.
2003;3:885–890.
4. Walid S.
Ayoub,
Carlos O.
Esquivel,...