INTRODUCTION
• An epileptic seizure is defined as “an excessive burst of abnormally synchronized neuronal activity affecting small or large neuronal networks that results in clinical manifestations that are sudden,
transient,
and usually brief’.
• Epilepsy is characterized by recurrent seizures secondary to a predisposition to generate abnormal electrical discharges from cortical grey matter,
and is complicated by subsequent neurobiological,
cognitive,
psychosocial and occupational consequences.
• Up to 10% of the population will have at least one seizure in their lifetime,
but only about 2% of the population will develop epilepsy.
• Worldwide,
50 million people have epilepsy,
and the World Health Organization estimates an associated morbidity of nearly 7.5 million disability-adjusted life years (health years lost) by 2015.
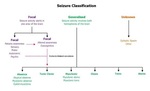
TYPE OF SEIZURES
The type of seizure depends on which part and how much of the brain is affected and what happens during the seizure.
Seizures can be divided into three major groups: focal (Partial),
generalised and unknown.
(1) Focal (partial) seizures
About 60% of people with epilepsy have focal (partial) seizures.
These seizures can often be subtle,
and may go unnoticed or may be mistaken for anything from intoxication.
Seizure activity starts in one focal area of brain.
Types of focal (partial) seizures are:
• Focal seizure- awareness retained (Formerly simple partial seizures)
• Focal dyscognitive seizures- awareness altered (Formerly complex partial seizures)
• Focal seizures evolving to a bilateral convulsive seizure (Formerly secondarily Tonic Clonic)
(2) Generalised seizures
• Generalised seizures are the result of abnormal activity in both hemispheres of the brain simultaneously.
Because of this,
consciousness is lost at the onset of the seizure.
• There are many types of generalised seizures-
• Absence
- Typical
- Atypical absence
- Absence with special features
- Myoclonic absence
- Eyelid Myoclonia
• Tonic-Clonic
• Clonic
• Tonic
• Atonic
• Myoclonic
- Myoclonic
- Myoclonic atonic
- Myoclonic tonic
(3) Unknown
This is a grouping of seizures that cannot be diagnosed as either a focal or generalised seizure and are thus grouped as unknown.
• Epileptic spasms
• Other
DIAGNOSIS TOOLS
• Electoencephalography (EEG) is accepted as a gold standard,
however only 50% of the patients are safely diagnosed.
• Magnetic Resonance Imaging -morphologic changes in 80% of patients.
It is the mainstay of imaging in epilepsy considering its better ability in detection,
characterization,
diagnosis of the epileptogenic focus and identifies surgical candidates.
The neuroimaging role in the study of an epileptic patient will be:
1.
To detect the structural lesions.
2.
To make an etiologic or syndromic diagnosis.
3.
To assess the relationship of the lesions with the adjacent brain structures.
4.
To determine the functional areas.
5.
In post-surgical studies detect- Complications and cause of surgical treatment failure (Recurrence or residual lesion)
It is important to note that the abnormality detected on imaging tests should becorrelated with clinical symptoms and electroencephalogram findings (EEG) in order toavoid false positives of the neuroimaging that lead to surgical failure.
In the structuralstudy of a patient with seizures,
MRI is the technique of choice for the detectionof epileptogenic abnormalities with a high sensitivity,
superior to other techniques.
Used MRI protocol:
Conventional MRI is not enough to detect the most common anatomicalabnormalities like epileptogenic mesial sclerosis or certain cortical dysplasias.
A "high spatial resolution" MRI is required (not less than 1.5 T MRI),
and a specific protocolhas to be performed which provides a good gray matter and white matter contrast,a high resolution images of the hippocampus and sequences sensitive to magneticsusceptibility.
In a basic protocol of epilepsy,
intravenous contrast administration is notneeded and it is only used in specific clinical situations (as meningitis) or to characterizefindings in the initial study (as neoplasia).
MRI protocol used in epilepsy is:
A.
Localizer
B.
T1 weighted image (Sagital and axial sections)
C.
Axial T2,
FLAIR,
T2 GE Sequence
D.
Diffusion weighted imaging (DWI)
E.
Fine (3mm) coronal oblique T2,
FLAIR,
T1 IR (Perpendicular to the hippocampus)
F.
Susceptibility weighted images.
G.
MR Intravenous contrast (Gadolinium) use,
in routine,
is not necessary.
H.
MRS if necessary.
Significance of various sequences
T1- Superior for cortical thickness and the interface between grey and white matter.
On T1WI look for grey matter occurring in an aberrant location as in gray matter heterotopia.
FLAIR- Sensitive for cortical and subcortical hyperintensities.
SWI- haemoglobin breakdown products in posttraumatic changes,
cavernomas,
calcifications intuberous sclerosis,
Sturge-Weber,
gangliogliomas.
High resolution T2W coronal oblique- Performed perpendicular to axis of hippocampus in imaging of mesial temporal sclerosis.
• Functional imaging modalities (PET and SPECT) are highly important in the pre surgical evaluation of patients with medically refractory complex partial seizures.
• The real power of SPECT lies in the opportunity of ictal examinations,
with a sensitivity ranging from 90 to 97%.
• Interictal PET studies using 18F-FDG measure regional glucose metabolism,
have been investigated for their value as non-invasive focus-localizing techniques.
These studies have sensitivity ranging from 80 to 85%.
• Blood tests (such as blood sugar,
complete blood count,
electrolytes and liver and kidney function tests)
• Lumbar Puncture to see if there is an infection or other problems.