Learning objectives
After reviewing this education exhibit you will be able to:
Understand the physiopathology of MWS
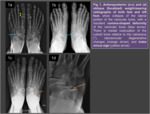
Review the classic radiologic signs of MWS in plain radiographs (Rx),
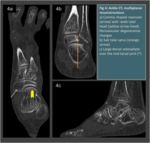
computed tomography (CT) and magnetic resonance imaging (MR)
Understand the limitations and strengths of the diagnostic tests
Approach to the differential diagnosis
Background
Spontaneous osteonecrosis of the navicular in adults,
also known as Müller-Weiss disease (MWD) is a rare syndrome,
that historically refers to spontaneous adult-onset tarsal navicular osteonecrosis.
It was initially described by Schmidt in 1925,
renamed after W.
Müller when he postulated the physiopathology of this condition; and K.
Weiss recognised the classic radiographic findings.
MWD is a separate entity from Köehler disease,
which refers to childhood osteocondrosis of the navicular,
thought to reflect either an ossification variant or osteonecrosis.
MWD is caracterized by progressive navicular...
Findings and procedure details
1.Physiopathology
Most patients present with chronic mid andhindfoot pain in the fourth or fifth decades,as the navicular collapses andsecondary osteoarthrosis develops.
With furthernavicular collapse,
pes planovarus develops,and tibia is forced to external rotation,which may lead to altered biomechanicsand osteoarthrosis of the knee.
Swelling andtenderness over dorsomedial aspect of themidfoot and heel varus can appear.
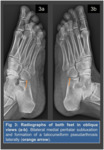
The medial longitudinalarch can be markedly flattened depending onthe severity of the disease.
This combinationof pseudohindfoot valgus and pes planusdeformity is also known as paradoxicalpes planovarus.
2 .
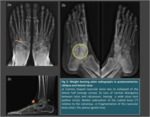
Radiologic Findings
Weight-bearing...
Conclusion
Müller-Weissdiseaseis a multifactorialconditionof the tarsal navicular in a suboptimally ossified bone withchronic lateral overloading,that is predisposed tocentral ischemia.
Remembering MWSas a mid-foot pain cause is important as it canresult in disability and deformity.Knowingthe physiopathology of the disease and the ongoingresearch on the static and dynamicsoft-tissue stabilizers involved in MWS may provide further insightand improved treatment of this disease.
Personal information
Andrea I Fuentealba Cargill,
MD.
Radiology Resident.Radiology Department,
Clínica INDISA; Santiago,
Chile.
[email protected]
Sebastian Butrón Bavestrello,
MD.
Radiology Department,
Clínica INDISA; Santiago,
Chile.
[email protected]
Jaime Drewes Araneda,
MD.
Radiology Department,
Clínica INDISA; Santiago,
Chile.
[email protected]
Natalia Rossel Bustamante,
MD.
Radiology Resident.Radiology Department,
Clínica INDISA; Santiago,
Chile.
[email protected]
Juan Pablo Durán Rodríguez,
MD.
Radiology Resident.Radiology Department,
Clínica INDISA; Santiago,
Chile.
[email protected]
Alvaro Provoste Soto,
MD.
Radiology Department,
Clínica INDISA; Santiago,
Chile.
[email protected]
Marcelo Castro Salas,
MD.
Radiology Department,
Clínica INDISA; Santiago,
Chile.
[email protected]
References
Nelson EW,
Rivello GJ.
Müller-Weiss disease of the tarsal navicular: an idiopathic case.
J Foot Ankle Surg.
2012 Sep-Oct;51(5):636-41
Doyle T,
Napier RJ,
Wong-Chung J.Recognition and management of Müller-Weiss disease.
Foot Ankle Int.
2012 Apr;33(4):275-81
Mohiuddin T,
Jennison T,
Damany D.
Müller-Weiss disease - review of current knowledge.
Foot Ankle Surg.
2014 Jun;20(2):79-84
Samim M,
Moukaddam HA,
Smitaman E.Imaging of Mueller-Weiss Syndrome: A Review of Clinical Presentations and Imaging Spectrum.
AJR Am J Roentgenol.
2016 Aug;207(2):W8-W18
Bartolotta RJ,
McCullion JC,
Belfi LM,
Hentel KD.Mueller-Weiss syndrome:...