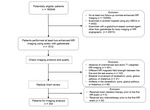
Patient Inclusion (Figure 1)
Patients were evaluated with routine laboratory tests before the MR examinations.
Patient data were obtained from electronic medical record,
including the sex and age of the patients,
indication for MR imaging,
renal and hepatic function,
and a history of chemotherapy or radiation therapy.
Abnormal renal function was defined as an estimated glomerular filtration rate (eGFR) ≤ 60mL/min/m².
Severely impaired renal function was defined as an estimated glomerular filtration rate of 45 mL/min/1.73 m2 or acute renal failure.
Abnormal hepatic function was defined as abnormal serum concentrations of aspartate aminotransferase,
alanine aminotransferase,
γ-glutamyl trans-peptidase,
and total bilirubin.
Radiation therapy was categorized as whole-brain irradiation and localized irradiation,
excluding the DN or GP.
Patients who received any chemotherapy prior to the first MR imaging were excluded (n = 34) because MR imaging with an unknown GBCA is likely and the effect of gadoterate could be diluted by including the remote therapy.
No patient received brain radiation therapy prior to the first unenhanced MR imaging.
Thus,
all patients who were indicated for MR imaging for brain tumors or metastasis received an intervening chemo- or radiation therapy and continued imaging exclusively in our hospital.
Imaging Acquisition
MR imaging was performed primarily with a 3.0-T MR scanner (Achieva or Ingenia; Philips Medical Systems,
The Netherlands,
or Skyra; Siemens Healthcare,
Germany) or a 1.5-T MR scanner (Achieva; Philips),
using an eight-channel head coil.
The brain MR protocol with a spin-echo sequence included T1-weighted imaging (T1WI),
T2-weighted imaging,
fluid-attenuated inversion recovery imaging,
and contrast-enhanced T1WI.
The range of axial unenhanced T1-weighted spin echo images were obtained using the following parameters: repetition time (TR)/echo time (TE),
450 – 550 msec/7.3 – 11 msec; section thickness,
5 – 7 mm; field of view (FOV),
20 – 25 cm; and matrix,
200 × 256.
Contrast enhancement was achieved using gadoterate meglumine (Dotarem; Guerbet,
Paris,
France) after unenhanced scan.
The interval between the injection of gadoterate and the beginning of contrast-enhanced MR imaging acquisition was less than 3 minutes.
A standardized single dose of 13 ml of gadoterate was exclusively applied in most adult patients in contrast-enhanced MR examination.
For perfusion MR including dynamic susceptibility contrast imaging or dynamic-contrast enhanced imaging,
a double injection of GADOTERATE was applied.
The number of gadoterate administrations and the interval between the first and the last examinations were recorded.
The mean interval between gadoterate administrations was calculated by dividing the time (in days) between the first and last MRI examinations by the total number of examinations minus 1.
Image Analysis
Two radiologists (J.E.P.
and J.Y.L.,
with 4 and 2 years of experience in neuroradiology,
respectively) blinded to the clinical data independently measured the SI in the anatomic structures by drawing regions-of-interest (ROIs) on the unenhanced T1-weighted images of each patient.
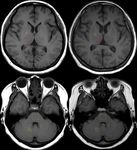
Quantitative analysis of the relative T1 SI was performed as previously described by placing square ROIs (minimum,
100 -mm²) on the right dentate nucleus (DN),
central pons (P),
right globus pallidus (GP),
and right thalamus (Th) (Figure 2).
To avoid any possible bias,
the order of ROI placement was randomly arranged in each patient (i.e.
GP à DN à Th à P in patient 1 and DN à Th à P à GP in patient 2).
When drawing the ROIs,
T2-weighted images were used to guide ROI placement.
If artifacts or structural distortion due to pathology were present on the right side,
ROIs were placed on the left side.
Structural distortion included local effects (i.e.
radiation change or tumor infiltration) and distant effects of Wallerian degeneration in the DN or GP from interconnected ipsilateral pathology.
The side of ROI placement was determined by an independent neuroradiologist (H.S.K.,
12 years of experience) who independently reviewed all MR images and did not participate in any other image review in the study.
The side of ROI placement was separately recorded for subsequent analysis.
The SIs of the DN,
P,
GP,
and Th from the 2 readers were then averaged.
The mean SI ratios for the first and the last examinations were calculated: the mean DN/P SI ratios were estimated by dividing the mean SI of the DN to that to the P,
and the GP-to-Th SI ratios by dividing the mean SI of the GP to that of the Th.
Thereafter,
the mean DN/P or GP/Th SI ratio difference was calculated between the first and the last examinations.
Statistical Analysis
All continuous variables were initially assessed for normality using the Kolmogorov-Smirnov test.
Interobserver agreement between the 2 readers was assessed using the intraclass correlation coefficient (ICC) with 95% confidence intervals.
The strength of agreement was classified according to common criteria as excellent (ICC > 0.75),
fair to good (ICC = 0.40 – 0.75),
and poor (ICC ≤ 0.40) .
A one-sample t test was used to determine whether the mean SI ratio difference between the first and last examinations differed from 0.
Stepwise regression analysis was performed to evaluate the predisposing factors associated with the mean DN/P and GP/Th SI ratio difference.
The nominal predisposing factors included sex,
type of magnetic field strength,
abnormal renal and hepatic function,
a type of brain radiation therapy and chemotherapy,
and the side of ROI placement.
The numeric predisposing factors included age,
number of gadoterate administrations,
mean time interval,
number of radiation therapy sessions,
and number of chemotherapy sessions.
Predisposing factors with possible multi-collinearity were excluded before a multivariate analysis.
The statistical models were built and analyzed using SAS 9.3 software (SAS Institute; Cary,
NC).
A P value of < 0.05 was considered statistically significant.