Keywords:
Interventional vascular, Liver, Catheter arteriography, Fluoroscopy, Chemoembolisation, Cancer, Endocrine disorders
Authors:
K. Mahmoud, H. El Khudari, S. Moawad, S. Saddekni, N. Ertel, R. Oser, N. A. Aboueldahab, B. Hamed, A. M. K. Abdel Aal; Birmingham, AL/US
DOI:
10.1594/ecr2018/C-0190
Results
The study included 9 males (53%) and 8 females (47%) with a mean age of 64.6 (SD=11.5) years.
Most of the primary tumors were from gastrointestinal tract in 11 patients (64.7%),
pancreas in 2 patients (11.8%),
lungs in 2 patients (11.8%),
ovary in 1 patient (5.9%) and unknown in 1 patient (5.9%).
Tumor burden ≥50% was seen in 5 patients (29.4%) (Fig. 1).
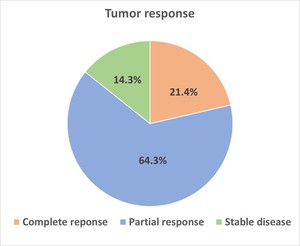
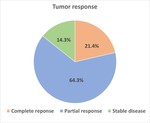
Fig. 1: The chart shows percentage of tumor response after transarterial chemoembolization of neuroendocrine tumor liver metastases according to m-RECIST criteria.
Imaging follow-up was available for 14 out of 17 patients (82.3%).
Complete response was seen in 3 patients (21.4%),
partial response was 9 patients (64.3%),
stable disease was 2 patients (14.3%) and no progressive disease was observed (Table 1) .
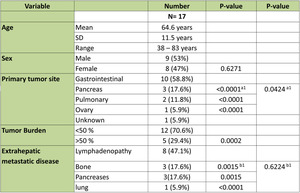
Table 1: Patients Demographic and Tumor characteristics.
At baseline,
14 patients (82.3%) were symptomatic.
After DEB-TACE,
11 patients (78.6%) and 3 patients (21.4%) had complete and partial symptom relief respectively (Table 2).
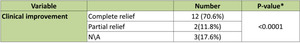
Table 2: Clinical symptoms improvement after transarterial chemoembolization for neuroendocrine tumor liver metastases.
Only two patients had grade 3 toxicity,
including 1 patient (5.9%) with liver abscess and 1 patient (5.9%) with persistent vomiting.
There was no grade 4 or 5 toxicity.
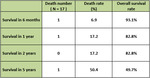
Survival was significantly higher in patients with tumor burden <50% (p=0.005) compared with those of ≥50%.
The overall survival at 6 months,
2 years and 5 years was 93.1%,
82.8% and 50% respectively (Table 3).
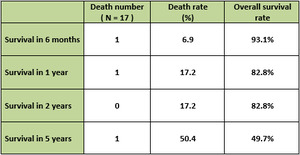
Table 3: Overall survival after transarterial chemoembolization for neuroendocrine tumor liver metastases.