The surgical technique most conventionally used is choledocus-choledochotomy.
Kher tube is placed to protect the bile duct from strictures and tears and allow easy access for cholangiography.
Tube is removed after some time.
In our center,
this time is three months.
In recent years a new technique has been introduced: hepaticojejunostomy on defunctionalized loop.
Complications that affect the bile duct have a very high prevalence: they occur approximately on 25% of liver transplant recipients,
are more frequent in the first three months after transplantation.
Furthermore,
it is the second most common complication of graft dysfunction behind the rejection.
For detection of this complications,
the best technique is magnetic resonance cholangiopancreatography.
However,
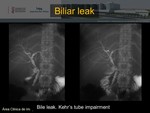
if the Kehr tube remains implanted,
cholangiography is preferred.
It is performed by introducing contrast through it,
because it allows a better analysis of possible biliary stricture.
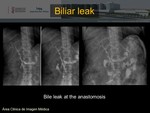
Leakage and anastomotic stricture
Its incidence is approximately 5% of all liver transplants.
Approximately 70% occur in the first month after the operation,
being more frequent in the early days.
They usually occur in connection with the Kehr tube and less frequently in the anastomosis.
Bile fluid can be contained forming a perihepatic collection (biloma). In that case,
treatment is based on the drainage of this collection.
Another more serious possibility,
it is that the bile fluid diffuses freely in the peritoneal cavity.
In this case,
it produces a chemical peritonitis,
which may require surgical cleaning and repair of the leak.
Development of fluid collections
Besides collections formed from leaking bile duct (bilomas),
there are other possible causes for the formation of collections.
The most common is the development of collections (seroma) in connection with surgical manipulation seen in the examinations carried out in the first days after transplantation.
They disappear in the first few weeks.
Water density pleural effusion caused by pleural irritation in connection with surgical procedure is also a common finding.
Hematomas and abscesses are characterized by a greater ultrasound heterogeneity compared to seroma or bilomas.
However,
it is difficult differentiate them only by using this techniques.
On these occasions,
they are especially useful CT and especially MRI.
Imaging techniques,
in these cases,
is not only diagnostic but also therapeutic.
Biliary sludge and choledocolitiasis
It is possible that the patient had biliary sludge or choledocholithiasis both on its own liver or gallbladder or in the graft.
Due to surgical handling,
they may migrate from this place to distal bile duct,
producing an obstruction that is clinically expressed as choledocholithiasis or pancreatitis.
The choledocholithiasis has a clearly defined boundary, which allows differentiate it from other elements causing an obstruction of the bile ducts,
such as bile molds.
Haemobilia
It consists of bleeding drains through the bile ducts.
This blood can coagulate and produce common bile duct stones,
which results in a clinical triad:
● Fluctuating jaundice. Jaundice is the result of direct bilirubin accumulation due to obstruction of the bile ducts.
Since clots produce intermittent interruption of bile flow,
jaundice is not constant but fluctuates.
● Upper gastrointestinal bleeding. The passage of blood from the bile duct to the duodenum can mimic upper gastrointestinal bleeding,
similar to that of duodenal ulcer.
● Pain in the right upper quadrant. Common bile duct stones produce intermittent obstruction of the bile duct,
causing similar symptoms to those of choledocholithiasis.
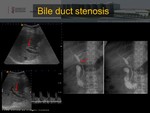
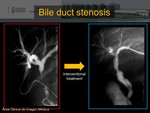
Obstruction and bile duct stenosis
It is the most common biliary complication both in adults and in the pediatric population.
They usually affect the anastomosis.
They can have several causes:
● Proliferation of fibrous structures involved in the anastomosis,
leading to a progressive narrowing of the bile lumen (stenosis) or causing obstruction.
● Obstruction associated with ischemia of the bile duct.
This is a less common cause.
It is usually the result of stenosis or thrombosis of the hepatic artery.
It will better explained in the ischemic complications section.
There are other changes that produce bile duct stenosis in other places,
apart from the anastomosis.
Sclerosing cholangitis deserves special mention and will be discussed in the corresponding section.
Another possibility is infectious cholangitis.
Sclerosing cholangitis
It is a possible cause of obstruction of the bile duct in a different place of the anastomosis. It is caused by preexisting disease in liver transplant.
In spite of having multiple causes,
it is important to consider primary sclerosing cholangitis of unknown etiology disease,
although it is associated with other autoimmune entities,
which suggests that it actually is an autoimmune disorder.
It is associated with ulcerative colitis,
retroperitoneal and mediastinal fibrosis,
orbital pseudotumor,
thyroiditis or Sjögren's syndrome,
among others.
The technique of choice for the diagnosis of this entity is the cholangio-resonance. It is relatively common no to diagnose it before transplantation because 95% of patients are asymptomatic.
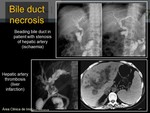
Ischemia associated with bile duct
It is a broad and diverse group of disorders of biliary duct,
all of them caused by impairment on arterial supply.
Its cause may be:
Thrombosis / hepatic artery stenosis
It is the most common cause of ischemia of the bile ducts.
It is produced because the bile ducts completely depend on the hepatic artery for blood supply.
Therefore,
a stenosis or occlusion of the hepatic artery causes necrosis of bile duct.
Following ischemia,
biliary bile leaks may occur,
leading to the formation of bile fluid collections (bilomas),
release of bile fluid to the peritoneal cavity or biliary enteric fistula formation.
Both cases,
thrombosis and stenosis,
are diagnosed by introducing contrast in the affected arteries,
both by CT angiography or by catheterization.
In both cases,
a significant decrease on vascular area or obstruction of blood flow will be observed.
The diagnostic technique of choice for thrombosis / hepatic artery stenosis is CT angiography.
Prolonged ischaemia
It comes as a consequence of no significant stenosis of the hepatic artery,
which cannot be observed in angiography or intra arterial injection of contrast by catheterization.
Nevertheless,
insufficient blood supply to the bile ducts leads to fibrotic proliferation and,
therefore,
its stenosis.
In cholangiography,
the hepatic duct adopt a beaded appearance.
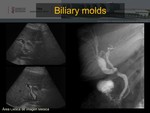
Obstruction of the biliary ducts by bile molds
This is obstruction of the bile duct by blood residues,
necrosis and biliary lithiasis,
all together.
It responds poorly to percutaneous treatments and often need surgical removal.
It is related to thrombosis / hepatic artery stenosis,
although it is not its only cause.