The blood flow of the liver implies around 25-30% of the cardiac output,
which is about 1500ml/min.
Liver receives this blood supply from two different sources: the portal vein and the hepatic artery.
However,
a part of the splanchnic venous flow does not join the portal vein in the extrahepatic portion: these veins enter the liver independently and flow directly into the hepatic sinusoids.
Such aberrant veins are called "third inflow" vessels to the liver.
There are two kinds of third inflow veins that supply venous blood to the liver: veins originating from a digestive organ,
such as the cholecystic vein and parabiliary venous system,
and systemic veins,
such as the epigastric-paraumbilical venous system [1].
Portal venous thrombosis (PVT) has an incidence of 1% in a review of autopsies and is a major cause for non-cirrhotic portal hypertension.
The clinical presentation of the disease is usually nonspecific and variable depending on the moment of its evolution.
In acute thrombosis,
the patient can complain of abdominal pain,
fever,
malaise or this initial episode may even go unnoticed.
Some patients are diagnosed in a chronic stage,
presenting symptoms derived from complications of portal hypertension,
such as thrombocytopenia,
splenomegaly,
gastrointestinal hemorrhage (due to varicose veins) and jaundice.
The main causes of PVT are hepatocellular carcinoma,
liver metastasis,
pancreatitis,
cirrhosis,
liver transplantation and splenectomy.
Other causes are pancreatic cancer,
abdominal inflammation (appendicitis,
diverticulitis,
pancreatitis) and portal hypertension; less frequent causes include myeloproliferative disorders,
connective tissue disorders or inflammatory bowel disease.
The entity now known as cavernous transformation of the portal vein (CTPV) was first described by Balfour and Stewart in 1869 as thrombosis and varicose dilatation of the portal vein leading to splenomegaly and ascites.
The term “cavernoma” was used to describe a pathologic condition in which the portal vein and lesser omentum present a peculiar spongy appearance because of numerous fine blood vessels penetrating these sites.
Balfour and Stewart also coined the phrase “cavenomatous transformation of the portal vein” to imply that this condition follows thrombosis of the portal vein [2].
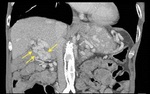
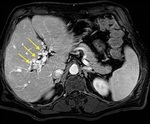
CTPV is defined as the development of venous channels in the porta hepatis within or around a previously thrombosed portal vein and their enhancement during the portal venous phase after contrast-agent injection.
The portal cavernoma is composed of two venous systems,
including the paracholedochal veins,
which run parallel to the ductal wall,
and the epicholedochal venous plexus,
located on the surface of the bile duct.
(Fig 1).
(Fig 2).
CTPV usually occurs in healthy liver,
in which it forms a bypass route around the obstructed portal vein into patent intrahepatic portal veins with normal resistance.
Cavernoma usually extends from the porta hepatis into the liver,
around lobar and/or segmental branches of the portal vein.
Blood may be shunted from a healthy liver segment into an affected one.
The time needed for CTPV to form after acute PVT is just a few days after the acute event.
Despite extensive intrahepatic and extrahepatic shunts,
portal hypertension persists [2].
The extension of CTPV is classified as extrahepatic (if it is extended from the confluence of the splenic vein and superior mesenteric vein to the bifurcation of the left branch of portal vein),
intrahepatic (if it is extended above the bifurcation of the left branch of the portal vein),
or both extra- and intrahepatic.
In this educational exhibit,
we describe the most common imaging findings of these syndromes and provide clinical and pathophysiological correlation of the radiological features.