Portal hypertension (PH) is a common consequence of chronic liver diseases and leads to major complications of liver cirrhosis,
such as ascites,
hepatic encephalopathy,
and variceal bleeding.
Definition of Portal Hypertension
PH is an increase of the hydrostatic pressure within the portal vein or its tributaries,
which is manifested as an increase in the pressure gradient between the portal vein and hepatic vein or the inferior vena cava (IVC).
Hepatic venous pressure gradient (HVPG) is calculated by subtracting the free hepatic venous pressure from the wedged hepatic venous pressure,
and the normal portal venous pressure varies between 5 and 10mmHg.
Clinically significant portal hypertension (CSPH) is defined as hepatic venous pressure gradient (HVPG) greater than or equal to 10mmHg,
and severe portal hypertension is defined as HVPG greater than or equal to 12mmHg.
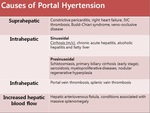
Causes and Mechanisms of Portal Hypertension
The most common cause of PH is liver cirrhosis,
but it can be caused by any disease interfering with blood flow at any level within the portal venous system.
According to anantomic location,
the diseases causing PH are classified in prehepatic,
intrahepatic,
or posthepatic[1] (Fig.
1).
In PH,
blood that normally flows through the liver is diverted into systemic veins because of increased resistance to portal venous flow.
This diversion of portal venous blood occurs via exiting portosystemic communications and the opening of embryonic channels.
The most common portosystemic anastomosis is via the left gastic-gastroesophageal route (80-90% of patients),
which causes lower esophageal and gastric varices.
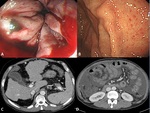
Complications of Portal Hypertension
The main complication of PH is variceal bleeding,
with a mortality rate of 30-50%. In addition, various comlications are caused by PH,
including hypersplenism,
ascites,
portal hypertensive gastropathy/enteropathy/colopathy,
hepatic encephalopathy and hepatorenal syndrome (Fig.
2).