1 VASCULAR CONGENITAL SYNDROMES
1.1 RENDU-OSLER-WEBER SYNDROME
Rendu-Osler-Weber syndrome,
also known as hereditary hemorrhagic telangiectasia,
consists of a variable combination of capilary and arteriovenous malformations and yet arteriovenous fistulas (therefore,
of high flow),
of visceral and mucocutaneous distribution,
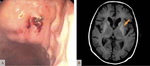
impairing preferably the brain,
skin,
lungs and gastrointestinal tract.
These patients usually present epistaxis around 10 years of age as a first manifestation of the disease and these episodes tend to worsen as time passes by.
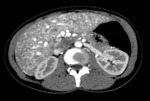
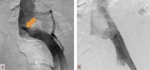
It is believed that up to 60% of patients have hepatic findings,
assymptomatic in the majority of cases.
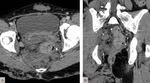
The multiphasic CT is the gold standard to evaluate these malformations that can be between the arterial and portal systems,
portal and systemic irrigation or even arteriovenous.
This hepatic visceral impairment,
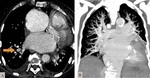
much like the pulmonary impairment,
can create various degrees of right to left shunts,
leading to cardiac insuficiency,
pulmonary hypertension and hepatic encephalopathy.
1.2 KLIPPEL-TRÉNAUNAY SYNDROME
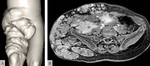
Klippel-Trénaunay syndrome is a combined vascular anomaly that can present venous and/or capilary malformations with or without lymphatic malformations which,
in most cases,
impairs a inferior limb,
leading to its abnormal development.
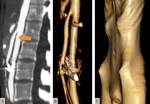
Being a low flow anomaly,
phleboliths can be seen as as imaging finding which,
in young patients,
are pathognomonic of a venous malformation that has previously bled or thrombosed.
In the abdomen,
though unusual,
the bladder,
rectum and distal colon are frequently impaired and bleeding is one of the most feared complications.
Another note worthy complication is Kasabath-Merrit syndrome.
Some malformations,
specially the cutaneous ones,
if too large can cause platelet sequestration,
leading to consumptive coagulopathies.
1.3 BLUE RUBBER BLEB NEVUS SYNDROME
The blue rubber bleb nevus syndrome (or Bean syndrome) consists of multiple simple venous malformations in many organs,
notably the skin and gastrointestinal tract,
that are low in flow and can therefore present with phleboliths.
The cutaneous lesions are usually present since birth,
are blue and small,
of rubbery texture,
and can be seen all throughout the body.
A Doppler evaluation can confirm the low flow nature of the lesions and MRI studies are the gold standard to assess their extension.
Enhancement is homogeneous and intense and,
due to the low flow,
flow voids aren´t seen but instead,
phleboliths and thrombus are expected.
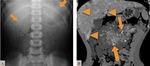
The gastrointestinal tract is impaired in all patients.
Though more common in the small intestine,
the lesions can be seen all throughout and tend to bleed,
this being of the main complications in such patients.
Polyps may also be present,
indistinguishable from neoplastic lesions from the imaging point of view and can be triggers for complications such as volvulus or intussusception.
2 COMPRESSION VASCULAR SYNDROMES
2.1 SUPERIOR MESENTERIC ARTERY SYNDROME
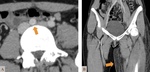
The superior mesenteric artery syndrome (SMAS) is an obstruction of the third duodenal portin due to its compression between the superior mesenteric artery (SMA) and the aorta.
The SMA is the second aortic ramus and its origin is at the L1-L2 vertebrae level,
with anterior and inferior orientation.
The third duodenal portion and the left renal vein pass between the SMA and the aorta.
The angle that is formed between the two vessels is maintained due to the retroperitoneal fat that involves the duodenum and it is that fat that prevents the compression of the organs in between.
Symptoms involve epigastric pain and postprandial fullness,
nausea and vomiting,
weight loss and anorexia.
Classically,
pain usually improves with left lateral decubitus or prone positioning.
Vomiting and weight loss can lead to a vicious circle,
with progressive loss of retroperitoneal fat.
2.2 COCKETT SYNDROME
Cockett syndrome,
also known as May-Thurner syndrome,
is the compression of the left common iliac vein between the right common iliac artery and the vertebral body of L5.
A compression higher than 50% of its diameter can be an incidental finding in up to 25% of patients but the chronic compression and pulsation can cause endothelial damage and intimal fibrosis,
leading to the development of venous hypertension,
stenosis,
obstruction and deep venous thrombosis.
This syndrome usually impairs middle-aged women.
The compression of this vein can be assymptomatic but the most typical symptom is left lower limb edema which can be acute,
due to deep venous thrombosis,
or chronic,
due to venous congestion.
Chronically,
varices and ulcers can appear as a result of venous insuficiency.
Phlegmasia cerulea dolens is a rare and severe complication and is the result of an extensive thrombosis with acute ischemia of the limb,
which can progress to gangrena.
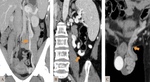
2.3 NUTCRACKER SYNDROME
The Nutcracker phenomenon is the compression of the left renal vein (LRV) which impairs the venous drainage of the left kidney to the inferior vena cava.
It can be assymptomatic and be just a variation of normality.
The term Nutcracker syndrome should be used when there are symptoms that go along with the imaging findings.
They are a result of the increase in pressure of the LRV and include haematuria,
proteinuria and left flank pain.
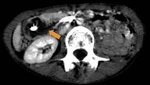
Tipically,
the LRV compression in this syndrome happens in the portion between the aorta and the superior mesenteric artery (anterior Nutcracker syndrome).
However,
the compression can also happen secondary to a variation of normality,
when the LRV passes posteriorly to the aorta and,
in this case,
compression is between the aorta and the adjacent vertebral body (posterior Nutcracker syndrome).
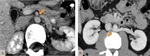
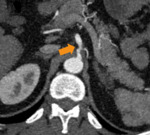
2.4 MEDIAN ARCUATE LIGAMENT SYNDROME
The median arcuate ligament syndrome happens when this diaphagmatic ligament,
with connective tissue fibers,
causes compression of the celiac trunk.
It can happen if this ligament shows a lower insertion than usual or if the celiac trunk is higher in origin.
Symptoms include postprandial abdominal pain,
weight loss,
nausea and vomiting.
Though compression alone of the celiac trunk during expiration is not clinically significant,
severe compression happens in a small percentage and can cause these symptoms.
When severe compression occurs,
colateral vessels between the SMA and the celiac trunk develop.
All symptoms can be secondary to the blood steal from the SMA to the celiac trunk.
Diagnosis can be stablished through arterial phases of post-contrast CT or MR.The proximal compression of the trunk is a finding that can be aggravated with expiration.
Additional findings such as distal dilatation of the trunk,
the typical hook shape that the vessel assumes after its compression and the presence of colateral vessels can help with stablishing diagnosis.