Keywords:
Radioprotection / Radiation dose, Radiation physics, Computer applications, Digital radiography, Radiation safety, Dosimetry, Radiation effects
Authors:
N. Loy Rodas, A. Kadkhodamohammadi, M. de Mathelin, A. Gangi, N. Padoy; Strasbourg/FR
DOI:
10.1594/ecr2018/C-1615
Aims and objectives
The use of X-rays for medical purposes carries with it an inherent risk of exposing patient,
surgeons and supporting medical staff members to harmful ionizing radiation.
As the popularity and difficulty of X-ray guided interventional procedures are increasing,
so are the risks of overexposure to ionizing radiation for patients and staff.
Countless studies have shown that any amount of exposure increases the risk of radiation-induced tissue reactions (epilation,
skin necrosis,
cataracts…) and of stochastic effects such as cancers [1].
While a patient’s exposure can be justified by medical indication and usually occurs in a single episode,
medical staff providing patient care can be exposed daily.
The repetitive nature of this exposure,
even to low dose,
increases the risk of developing negative biological effects,
and such a risk increases with the dose accumulated over time [2].
Studies have documented the dosage of ionizing radiation among interventional practitioners as the highest registered for any medical staff working with X-rays [1].
Indeed,
most interventions are performed under fluoroscopy guidance (continuous X-ray imaging) and staff is obliged to remain close to the patient during the procedure (see figure 1).
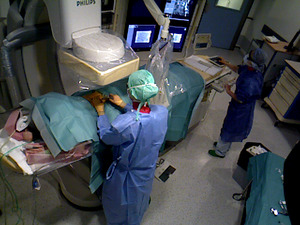
Fig. 1: Fluoroscopy-guided interventional procedure at Strasbourg's University Hospital.
Currently,
no means exist to intraoperatively monitor the 3D propagation and magnitude of scattered radiation fields.
The invisible nature of radiation and the complexity of its propagation difficult the intraoperative monitoring of exposure and the optimal use of protective measures.
They also lead to reduced awareness and concern of overexposure during a procedure.
Indeed,
studies have reported a considerable amount of unnecessary exposure resulting from a lack of awareness,
a reduced concern of long-term exposure risks and a poor knowledge of the behavior of ionizing radiation [3].
We therefore propose a system capable of providing real-time visual feedback of the current patient and staff exposure and of the 3D propagation of scattered radiation using augmented reality (AR).
Such a system can help improving the monitoring of radiation monitoring and to increase clinical staff's awareness of radiation risk and patient dose.
A prototype of the system has been demonstrated in an interventional room in our institution.
The system has been positively received by our collaborating interventional radiologists since it provides a clear in-situ visualization of radiation,
and is ideal for teaching about radiation’s diffusion effects.



