Keywords:
Thorax, Computer applications, Oncology, CT, CAD, Percutaneous, Computer Applications-3D, Screening, Cancer, Epidemiology, Neoplasia
Authors:
M. Jelitto-Gorska, A. Durawa, R. Dziedzic, P. Kalinowska, M. Piskunowicz, E. Szurowska, K. Dziadziuszko, W. Rzyman, M. Studniarek; Gdansk/PL
DOI:
10.1594/ecr2018/C-2834
Methods and materials
Between February 2009 and April 2011,
8649 asymptomatic healthy volunteers in the age of 50-75,
with at least 20 pack-years smoking history underwent chest Low-Dose Computed Tomography (LDCT) screening in the Pilot Pomeranian Lung Cancer Screening Program.
Both former and current smokers were included in the program.
For patients with family history of lung cancer,
minimum history of smoking was ten pack-years.
A questionnaire included age and gender and complete smoking history was obtained.
Participants who reported lung cancer symptoms such as weight loss,
hemoptysis or repetitive pneumonias were excluded.
The cigarette consumption was measured in pack-years calculated by multiplying the average number of cigarettes smoked daily by the number of years smoked and dividing the result by 20.
Former smokers also reported years passed since smoking cessation.
The LDCT screening was carried out in 19 radiological centers in the Pomeranian region of Poland with the use of at least 4-rows CT scanners.
Low dose parameters were applied: 120kV and 20-40mAs.
An experienced radiologist evaluated each examination.
In case of nodule detection,
the board of specialists – two radiologists and thoracic surgeon,
consulted each result.
The screening protocol was designed for a 1-year follow-up due to the program’s timeframes.
According to CT results participants were categorized into four groups according:
- negative LDCT results - no further observation
- Mean size of lung nodule ≤5mm - one follow-up LDCT after 12 months
- Mean size of the nodule - 5 - 10mm - follow-up LDCT after 3,
6,
and 12 months;
- Mean size of lung nodule ≥10 mm,
or smaller but highly suspicious for malignancy - diagnostic work-up in the Department of Thoracic Surgery
Depending on medical indications,
the work-up consisted of bronchoscopy,
fine needle aspiration biopsy,
and spirometry tests.
Highly suspicious nodules with negative biopsy results were accepted for surgery.
According to the final pathology report,
patients were classified into Lung Cancer Positive (LCP) or Lung Cancer Negative (LCN) group.
Each group was analyzed according to smoking history,
nodule size and its radiological features,
and COPD and emphysema severity.
The presence of COPD was noted when FEV1/VC% <70%.
FEV1/FVC was analyzed as a continuous variable and categorical variable using the categories: >70%; 60% to 69.9%; 50% to 59.9%,
and <50%.
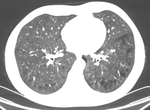
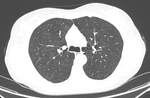
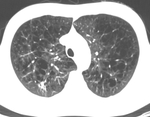
The occurrence of emphysema was checked visually by an experienced radiologist and noted when low attenuation regions were depicted in the lungs.
The severity of emphysema was categorized as mild,
moderate and severe.
The type of emphysema was also visually determined as cetrilobular,
paraseptal or panlobular – examples of each type are presented in Figures 1-3.
In statistical analysis,
Fischer’s exact tests or Student’s t-tests were used with p values ≤0.05 considered statistically significant.