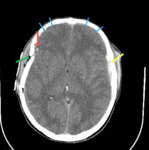
DAI is a severe form of traumatic brain injury which mostly occurs in high-speed motor vehicle accidents.
It is considered to be one of the most common types of primary neuronal injury in patients with severe head trauma representing approximately one half of all intra-axial traumatic lesions.
Overall incidence is 200 per 100 000 person.
It mostly occurs in younger population and it is the most common cause of persistent vegetative state.
Therefore,
it is a serious medical condition representing a great tragedy for the patients and their family.
DAI rarely occurs in isolation.
It is usually accompanied by other traumatic brain injuries such as hemorrhagic contusion or extra-axial hematoma.
ETIOLOGY
DAI results from high energy trauma.
Mostly from motor vehicle crashes and,
in some cases,
from falls and assaults.
Beside the direct impact force,
the inertial forces which are the result of rapid head rotational motions also play a significant role in pathogenesis.
Those forces deform the white matter and lead to DAI,
commonly referred to as “shearing” brain injury.
BIOMECHANICS OF DAI AND AXONAL PATHOLOGY
As the name implies,
DAI is characterized by widespread disruption of axons as a consequence of enduring intense acceleration or deceleration forces.
Those forces,
caused by unrestricted head movement instantly after injury,
are forcing the cerebrum to move back and forth,
pivoting around the upper brainstem.
The brainstem,
together with the cerebellum,
is held firmly fixed by the tentorium,
and the falx prevents side-to-side motion.
Axons are stretched but do not snap from this injury.
These stretching of the axons is known as “tensile elongation” of axons,
and it is thought to result in damage of the axonal cytoskeleton.
Subsequently,
the axons start to swell.
Calcium entry into damaged axons initiates further damage by the activation of proteases.
Swollen axons may become disconnected and contribute to additional neuropathologic changes in brain tissue.
Axonal injuries can occur anywhere but are particularly common in the parasagittal parts of the brain,
the corpus callosum,
fornix,
internal capsule,
and the brain stem.
Microscopic examination of the brain tissue,
which can be done post-mortem,
reveals the pathologic signature of DAI: a multitude of swollen and disconnected axons.
Axonal swellings can be detected with hematoxylin and eosin (H&E) and silver stains 15 hours after the injury.
In highly severe causes,
axons are not only swollen,
further mechanisms also lead to tissue tears and consequent intraparenchymal hemorrhage.
Axonal swellings can take a chronic form and persist for years.
Distal to the swellings,
axons and myelin degenerate and gliosis develops over time.
Severe DAI may cause the decrease of white matter volume,
atrophy of the corpus callosum,
and dilatation of the lateral ventricles.
CLINICAL PRESENTATION
Loss of consciousness at the moment of impact is typical and it occurs in almost all cases.
In severe DAI loss of consciousness is prolonged and it leads to coma.
There is a likelihood of a vegetative state or even death.
As in any trauma patient it is obligatory to determinate GCS (Glasgow Coma Scale) (Table.1).
Based on GCS,
traumatic brain injury can be classified as mild,
moderate or severe.
- Patients with GCS score from 13 to 15 are considered to have mild traumatic brain injury
- Patients with GCS score from 9 to 12 are considered to have moderate traumatic brain injury
- Patients with GCS score 8 or below are considered to have severe traumatic brain injury
Most head trauma patients have higher GCS score and consequently,
mild traumatic brain injury.
Sometimes DAI can occur with milder symptoms such as symptoms of cerebral concussion.
Possible symptoms,
which are nonspecific symptoms of any traumatic brain injury are:
- disorientation or confusion
- headache
- nausea or vomiting
- drowsiness or fatigue
- trouble sleeping
- sleeping longer than normal
- loss of balance or dizziness
The Adams classification is commonly used to classify the severity of of DAI (Table.2).
The loss of consciousness in concussion probably happens due to a functional disturbance of the reticular activating substance in the brainstem.
Since DAI is rarely an isolated finding in traumatic brain injury,
clinically it is hard to distinguish the symptoms from other accompanied injuries (Fig.1).
It is important to understand that is difficult to diagnose DAI in the acute phase.
Clinical signs and neuroimaging findings may suggest the diagnosis,
but confirmation is only possible post-mortem.
TREATMENT
Treatments of patients with diffuse axonal injury is primary supportive care.
There is no specific treatment. The main goals are prevention of secondary injuries and facilitating rehabilitation.
In the acute phase secondary injuries (cerebral edema,
impaired metabolism,
free radicals formation,
excitotoxicity) lead to increased mortality.
Therefore,
it is important to focus the treatment of DAI on preventing hypotension,
hypoxia,
cerebral edema,
and elevated intracranial pressure (ICP) since those factors can facilitate further brain damage by causing low oxygen delivery.
ICP (intracranial pressure) monitoring is indicated in patients with severe head injury (GCS score 8 or below).
Short-term anticonvulsant treatment can be used to prevent early post-traumatic seizures.
Steroids are sometimes used as part of therapy for reduction of cerebral edema.
PROGNOSIS
In mild cases of DAI clinical abnormalities such as headache,
memory and mild cognitive impairment,
personality change (post-concussion syndrome) may persist for months or longer.
In severe DAI a great number of patients remain unconscious and most likely,
turn to persistent vegetative state.
In patients who regain consciousness severe neurologic impairments are possible.
For some patients,
with most severe cases of DAI the outcome may be lethal.