PSEUDOPROGRESSION is a subacute treatment (RT-TMZ or RT alone) related reaction with or without clinical deterioration.
Most patients are clinically asymptomatic despite the increase of tumor enhancement.
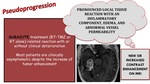
There is a pronounced local tissue reaction with an inflammatory componente,
edema and abnormal vessel permeability.
NEW OR INCREASED CONTRAST ENHANCEMENT ON MRI
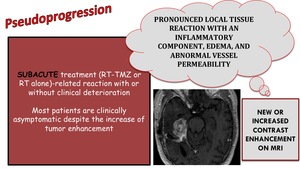
Fig. 3: Subacute treatment-related changes that appears as new or increased contrast enhancement on MRI
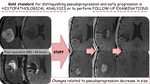
Gold standard for distinguishing pseudoprogression and early progression is histopathological analysis or to perform follow-up examinations.
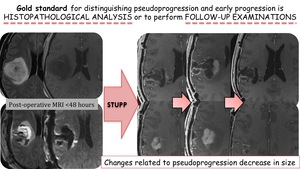
Fig. 4: Gold standard for distinguishing pseudoprogression and early progression
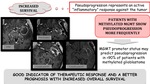
Pseudoprogression represents an active "inflammatory" response against the tumor and is related to increased survival.
Patients with methylated MGMT show pseudoprogression more frequently.
In fact,
MGMT promoter status may predict pseudoprogression in >90% of patients with methylated glioblastoma.
Pseudoprogression is a good indicator of therapeutic response and a better prognosis with increased overall survival.
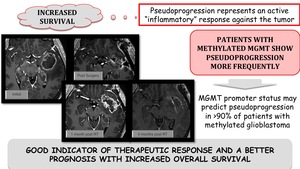
Fig. 5: Increased overall survival related to pseudoprogression
When we have to suspect pseudoprogression?
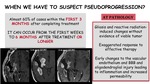
- Almost 60% of cases within the first 3 months after completing treatment
- But it can occur from the first weeks to 6 months after treatment or longer
A wide variation reported in the incidence of pseudoprogression (9%-64%) and depends on the amount of enhancement increase required for diagnosis:
- "Any lesion enhancement growth". This pattern overstimated incidence of pseudoprogression.
An initial slight enhancement after RT is frequent and usually disappears.
- 25% increase. This pattern of enhancement is related to a lower incidence of pseudoprogression,
but represents a better decision.
Any increase below woul not require any change in therapy,
since it would be recognized as stable disease.
At pathology,
pseudoprogression is characterized by gliosis an reactive radiation-induced without evidence of viable tumor.
There are early changes to the vascular endothelium and BBB and oligodendroglial injury leading to inflammation and increased permeability.
It represents an exaggerated response to effective therapy.
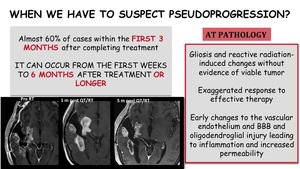
Fig. 6: When we have to suspect pseudoprogression?
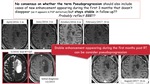
There is no consensus on whether the term pseudoprogression should also include cases of new enhancement appearing during the first 3 months that does nor dissapear (as it appears in PsP definition),
but stays stable in follow-up.
These cases probable reflect BBB.
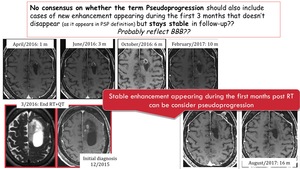
Fig. 7: No consensus whether the term PsP should also include a new enhancement appearing during the first 3 months that does not dissapear
TIME is important:
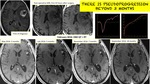
- Pseudoprogression can occur beyond 3 months.
It appears more frequently,
but not exclusively,
in the first 3 months following radiation therapy.
- It is unclear the exact number of "late pseudoprogression".
- With immunotherapy RANO recommends 6 months follow-up.
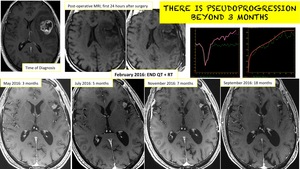
Fig. 9: Pseudoprogression beyond 3 months
There is also CLINICAL RELEVANCE.
Pseudoprogression has important implications in clinical decisions:
- If we name it pseudoprogression and it is a true progression ⇒ delayed new treatment or enrollment into clinical trials
- If we called it a true progression and it is a pseudoprogression ⇒ premature stop of an effective therapy
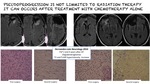
Pseudoprogression is not limited to radiation therapy and it can occurs after treatment with chemotherapy alone.
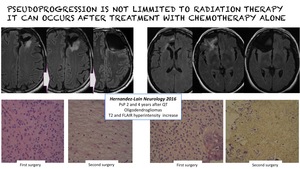
Fig. 8: Pseudoprogression can occur after treatment with chemotherapy alone