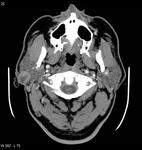
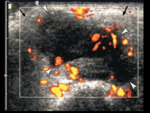
PATHOLOGY OF THE PAROTID GLAND
1.
SIALOLITHIASIS
Salivary stones are most often located in the submandibular gland (60%–90% of cases) and may be multiple.
Parotid glands are affected in about 10%–20% of cases.
- On classic radiographs,
intraglandular and small stones may be missed,
and only about 20% of sialoliths are radiopaque.
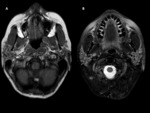
- CT allows visualization of large stones but without their precise localization and without the possibility of assessment of the ducts.
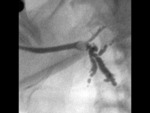
- The standard technique for imaging of the intraglandular ductal system remains digital sialography. Fig. 3
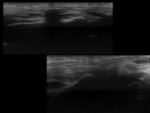
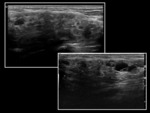
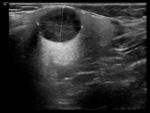
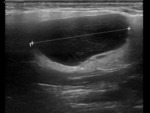
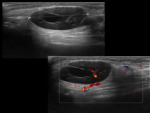
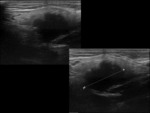
- US features of sialolithiasis include strongly hyperechoic lines or points with distal acoustic shadowing,
which represent stones. In symptomatic cases with duct occlusion,
dilated excretory ducts are visible. Fig. 4
Sialolithiasis causes partial or total mechanical obstruction of the salivary duct,
which results in recurrent swelling of a salivary gland during eating and may be complicated by bacterial infection.
In chronic cases of obstruction,
the gland undergoes fatty atrophy and becomes asymptomatic,
unless secondarily infected.
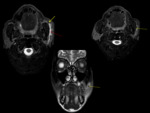
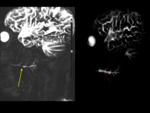
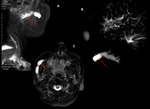
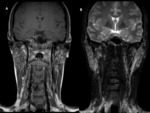
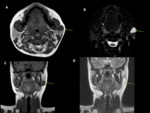
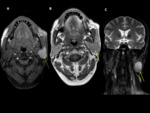
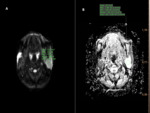
- MR sialography Fig. 5,
Fig. 6, Fig. 7

Fig. 8
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
2.
SIALOSIS
Sialosis is a noninflammatory,
nonneoplastic,
recurrent, painless salivary gland swelling,
usually bilateral,
which most often concerns the parotid glands.
Sialosis has been described in connection with endocrine diseases,
malnutrition,
hepatic cirrhosis,
chronic alcoholism,
or different deficiency diseases (eg,
avitaminoses).
US reveals enlarged,
hyperechoic salivary glands with a poorly visible deep lobe but without focal lesions or increased blood flow.
3.
SIALADENITIS
Sialadenitis refers to inflammation of the salivary glands.
It may be acute or chronic and has a broad range of causes.
Patients may present with painful swelling of the concerned salivary gland,
after eating (salivary colic).
In bacterial sialadenitis,
there may be a purulent discharge.
Etiology:
- Bacterial: Acute suppurative (usually localized)
- Viral: Acute viral parotid sialadenitis (epidemic parotitis)
- Obstruction-induced by sialolith: Secondary sialadenitis
- Unknown etiology: Juvenile recurrent parotitis
Associations:
- Sjogren syndrome: chronic sialadenitis
- Mikulicz syndrome: chronic sialadenitis
- post radiation:post-irradiative sialadenitis
- iodine-131 administration
Radiographic features:
- Fluoroscopy
Sialography is contraindicated in acute sialadenitis because it can worsen the infection.
- Ultrasound
- In acute sialadenitis,
the affected gland appears enlarged,
hypoechoic and hyperaemiac on ultrasound
- In chronic infective forms,
the affected gland appears atrophic and diffusely hypoechoic with irregular margins
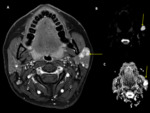
- CT

Fig. 9
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
- MRI

Fig. 10
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
4.
PAROTID SJÖGREN SYNDROME (SjS)
Sjögren syndrome is a chronic autoimmune disease predominantly affecting women over 40 years of age.
It is characterized by intense lymphocytic and plasma cell infiltration and destruction of salivary and lacrimal glands.
Imaging appearance depends on stage of disease and presence or absence of lymphocyte aggregates within parotid
- Earliest stage SjS: Parotids may appear normal.
- Intermediate stage SjS: Miliary pattern of small cysts diffusely throughout both parotids.
- Late stage SjS: Larger cystic (parenchymal destruction) & solid masses (lymphocyte aggregates) in both parotids.
Punctate diffuse calcifications in both parotids
Conventional sialography
- Alternating areas of ductal stenosis and dilatation (string of beads pattern)
- Acinar spill into enlarged acini (apple tree pattern)
US features of advanced Sjögren syndrome include inhomogeneous structure of the gland with scattered multiple small,
oval,
hypoechoic or anechoic areas,
usually well defined,
and increased parenchymal blood flow.
Hypoechoic or anechoic areas are believed to represent infiltration by lymphatic cells, destroyed salivary parenchyma,
and dilated ducts.
Sjögren syndrome is frequently associated with both reactive and neoplastic lymphoproliferative disease.
Fig. 11
CT Findings

Fig. 12
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
MR Findings Fig. 14,
Fig. 15

Fig. 13
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
5.
NEOPLASMS
5.1 BENIGN NEOPLASMS
The most common benign neoplasms are pleomorphic adenomas (mixed tumor) and Warthin tumors (adenolymphoma, cystadenolymphoma,
papillary cystadenoma lymphomatosum). Other benign tumors (eg,
oncocytoma,
basal cell adenoma) occur less frequently in the salivary glands.
Among nonepithelial lesions,
hemangiomas,
lipomas, and neurinomas or schwannomas may be found.
5.1.1.
PLEOMORPHIC ADENOMA
Occur most often in the parotid gland (60%–90%) in people in the fourth and fifth decades of life but may arise at any age.
There is a slight predominance in women.
Pleomorphic adenomas are usually solitary and unilateral.
They grow slowly and may be asymptomatic.
Nontreated pleomorphic adenomas may undergo malignant transformation after decades.
In exceptional cases,
pleomorphic adenomas may be clinically aggressive; they may metastasize and even be fatal.
After inadequate surgery, pleomorphic adenomas often recur,
usually multifocally.
US: they are hypoechoic, well-defined,
lobulated tumors with posterior acoustic enhancement and may contain calcifications.
The feature of lobulated shape is being emphasized in differential diagnosis.
Vascularization in pleomorphic adenomas is often poor or absent (even when the sensitive power Doppler mode is used) but may be abundant. Fig. 16
CT: When small,
they have homogeneous attenuation and prominent enhancement.
When larger,
they can be heterogeneous with less prominent enhancement,
foci of necrosis,
and possible delayed enhancement.
Small regions of calcification are common
MRI: Fig. 17,
Fig. 18

Fig. 19
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
5.1.2.
WARTHIN TUMOR
Warthin tumor is the 2nd most common benign salivary neoplasm (5%-10% of all benign salivary neoplasms). It arises most often in men in the fifth and sixth decades of life. The relationship between smoking and development of Warthin tumors has been proved. Warthin tumor is usually solitary, unilateral,
and slow growing.
In about 10%–60% of cases,
tumors may occur bilaterally or multifocally,
sometimes metachronously,
growing and manifesting clinically at different times.
Sporadically,
the epithelial component of Warthin tumor may undergo malignant transformation.
US: Most tumors tend to be ovoid,
with well-defined margins and multiple irregular,
small,
sponge-like anechoic areas.
Tumors that are large (e.g.
>5 cm) tend to have a higher proportion of cystic content than smaller lesions had and in some cases can be composed almost entirely of cystic material. They are often hypervascular. Fig. 20
CT:

Fig. 21
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
MRI: Fig. 23,
Fig. 24

Fig. 22
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
5.2 MALIGNANT NEOPLASMS
The most common malignant neoplasms occurring in salivary glands are mucoepidermoid carcinoma and adenoid cystic carcinoma.
Squamous cell carcinoma,
acinic cell carcinoma,
and adenocarcinoma are less common.
Unlike benign salivary neoplasms,
malignant tumors may grow rapidly,
may be tender or painful at palpation,
may be fixed to the background, and may cause facial nerve paresis or paralysis. Fig. 27, Fig. 28
5.2.1.
MUCOEPIDERMOID CARCINOMA
Mucoepidermoid carcinoma occurs mostly between 30 and 50 years of age. In the parotid gland, they are the most common malignant primary neoplasm. presents as a painless swelling,
with or without facial nerve involvement.
Mucoepidermoid carcinoma may show several levels of differentiation and thus different tendencies to infiltration, metastases,
and progress; the poorly differentiated form is extremely aggressive.
Radiographic features:
Radiographic appearances largely depend on grade,
making preoperative imaging important in planning and counseling.
US: Typically a well-circumscribed hypoechoic lesion,
with a partial or completely cystic appearance.
The lesion stands out against the relatively hyperechoic normal parotid gland.
CT: Low-grade tumors appear as well-circumscribed masses,
usually with cystic components.
The solid components enhance,
and calcification is sometimes seen.
They have appearances similar to benign mixed tumors.
High-grade tumors on the other hand,
have poorly defined margins,
infiltrate locally and appear solid. Fig. 29
MRI:

Fig. 25
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
5.2.2.
ADENOID CYSTIC CARCINOMA
It's the second most common malignancy involving the parotid gland. They are locally aggressive with a propensity for perineural spread.
CT: Generally,
a distinction is made radiologically between low-grade and high-grade adenoid cystic carcinomas.
Low-grade tumours tend to be well-defined,
in contradistinction to high-grade tumours,
which appear infiltrative.
However,
both subtypes are usually homogeneously enhancing after contrast administration.
Adenoid cystic carcinomas are frequently associated with perineural spread (via cranial nerve VII),
which is well appreciated on MRI.
MRI:

Fig. 26
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
5.2.3.
METASTASES
Salivary glands are very uncommonly sites of metastases. Primary tumors metastasizing to salivary glands may be located in the head and neck region, as well as in more distant parts of the body. Melanoma,
spinocellular cancer,
breast cancer,
and lung cancer may produce metastases to intraparotid lymph nodes.
Extremely rare are metastases from renal cancer. Fig. 30
At US,
metastases may be well defined and oval.
It may be difficult to differentiate multiple metastatic lesions from some patterns of inflammation,
Sjögren syndrome,
and granulomatous disease at US.