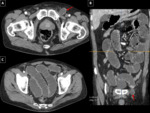
NORMAL ANATOMY
The left iliac fossa (LIF) is defined as the space between two imaginary lines,
a vertical one at the level of the left midclavicular line and a horizontal line between the two anterosuperior iliac spines.
The left iliac fossa is a crossroad in which coincide the gastrointestinal tract (sigmoid colon) the genitourinary tract (left ureter and left ovary in the female),
the iliac vessels and the muscles (iliopsoas).
CLASSIFICATION OF THE PATHOLOGY OF THE LEFT ILIAC FOSSA.

Fig. 1
References: Department of Radiology, Hospital Universitario Marqués de Valdecilla - Santander/ES
1.
GASTROINTESTINAL SYSTEM
1.1.
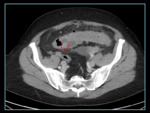
ACUTE DIVERTICULITIS
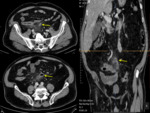
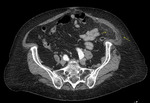
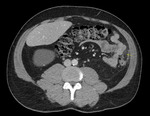
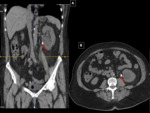
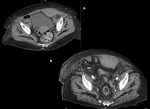
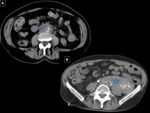
Sigmoid diverticulitis is the most common gastrointestinal cause of pain in the left iliac fossa seen in adult patients.
CT is the technique that will give us more information,
especially in situations of urgency regarding location,
degree of involvement and the existence of associated complications:
- Visualization of diverticula from 2 mm to 2 cm.
- Thickening and trabeculation of fat,
often disproportionate in comparison with wall thickening of the colon,
- Segmental thickening of the colonic wall.
- Mural enhancement after administration of intravenous contrast.
Greater in the zone that corresponds to the mucus and separated with a band of low attenuation.
- Free liquid.
- Detection of complications (signs of intestinal obstruction,
free air bubbles,
extravasation of contrast,
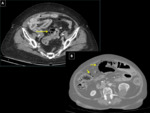
abscess of the sigmoid colon or at distant sites. Fig. 2, Fig. 3
1.2.
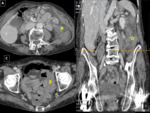
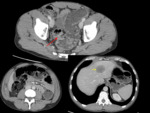
INFECTIOUS COLITIS
Common viral gastroenteritis can cause mild symptoms,
but it can also present with features similar to diverticulitis,
particularly if caused by pathogens such as Yersinia,
Campylobacter,
or Salmonella. Fig. 4
Imaging findings on US/CT involve a long segment circumferential wall thickening with hyperemia in color Doppler US and homogenous enhancement in CT,
usually without stranding of the adjacent fat.
Mesenteric adenopathy and surrounding free fluid may be present
1.3.
INFLAMMATORY BOWEL DISEASE
Inflammatory bowel disease usually affects longer intestinal segments and not only limited to sigma.
There are not necessarily diverticula in the affected area.
The clinical parameters show greater systemic involvement.
Imaging features:
- Transmural bowel wall thickening (> 4 mm).
- Mural stratification ("target" or stratified appearance of the bowel wall due to mucosal hyperenhancement (inner layer),
submucosal edema (low-density middle layer),
and soft tissue density outer layer (muscularis propria and serosa).
- Active inflammation leads to engorgement of vasa recta (the “comb sign”) and inflammatory changes in adjacent mesenteric fat.
- Chronic inflammation results in fibrofatty proliferation along the mesenteric side of the bowel wall,
creating the “creeping fat” sign.
- Complications: intramural or interloop abscesses,
fistulous anastomosis
1.4.
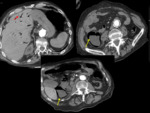
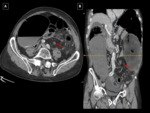
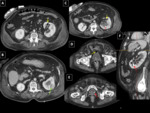
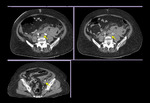
INTESTINAL ISCHEMIA AND ISCHEMIC COLITIS
Intestinal ischemia occurs in patients who are generally older,
with suspicious risk factors and systemic data of severity.
The MDCT usually presents a bowel segment that is thinner or thicker than diverticulitis,
associated with edema,
mural and peritoneal,
there may be free fluid,
a decrease in contrast uptake and loss of definition of the intestinal wall.
In advanced cases,
a bowel infarct may be present,
which manifests at CT as pneumatosis and air in the portal venous system. Fig. 5, Fig. 6
1.5.
APPENDICITIS
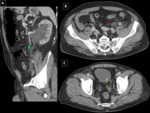
Acute appendicitis can cause suprapubic or lateralized pain to the left in exceptional cases if the anatomical situation of the appendix describes the path to the medial abdomen and even extends beyond the midline.
The inflamed appendicular end may manifest as left pain. Fig. 7
1.6.
VOLVULUS
Volvulus manifests acutely with a subobstructive or obstructive picture with the classic image of sigma dilated in coffee bean.
It can produce intestinal perforation with severe systemic involvement of the patient's condition. Fig. 8
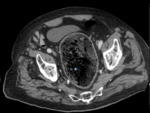
1.7.
MALIGNANT NEOPLASM
Sigmoid cancer is the first entity to consider due to its prevalence and its difficulty to diferenciate from diverticulitis (bowel wall thickening and pericolonic fat stranding occur in both).
Mesenteric edema and vascular engorgement are more characteristic of diverticulitis,
whereas the presence of pericolonic lymph nodes is more suggestive of a neoplasm. Fig. 9
1.8.
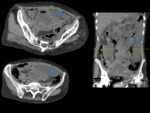
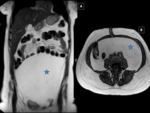
CONSTIPATION/FECALOMA
Fecalomas are suspected with adequate clinical history.
They are confirmed with simple abdominal X-ray or MDCT.
If they are associated with obstructive symptoms,
they produce left pain and dilatation of the proximal colon,
depending on the level of obstruction. Fig. 10
1.9.
INTESTINAL OBSTRUCTION
Intestinal obstruction is the stopping of passage of the intestinal contents at some point along the digestive tract,
secondary to a mechanical cause that prevents the progression of the intestinal contents. When it is not complete or persistent,
it is called intestinal subocclusion.
It may manifest as pain in the left iliac fossa due to distention of jejunal loops,
descending colon or sigmoid.
It is important to establish the cause of the obstruction,
either intrinsic (inflammation,
intussusception,
neoplasm,
ischemia...) or extrinsic (hernias,
fibrous adhesions...). Fig. 11, Fig. 12
1.10.
OMENTAL INFARCTION
Omental infarction is a rare cause of pain in left iliac fossa because it usually happens in the right side. Fig. 13
- Omental infarction is caused by torsion or vascular thrombosis secondary to postoperative omental adhesions,
trauma,
or increased intra-abdominal pressure (coughing,
obesity,
strenuous exercise).
- CT imaging features vary from an ill-defined,
heterogeneous fat-attenuation lesion to a well-defined heterogeneous fatty mass.
- Omental infarction may be differentiated from epiploic appendagitis by location (between the colon and anterior abdominal wall),
larger size (often greater than 5 cm in diameter),
and absence of a hypoechoic/hyperattenuating ring.
1.11 INFARCTION / EPIPLOIC TORSION (APPENDAGITIS)
Epiploic appendages are small fat protrusions arising from the serosal surface of the colon; these are not usually identifiable on cross-sectional imaging. Fig. 14
- Torsion of an epiploic appendix causes vascular occlusion,
ischemia,
and acute onset abdominal pain.
- Since the number and size of epiploic appendages increase from the cecum to the sigmoid colon,
epiploic appendagitis usually results in left-sided abdominal pain.
- Imaging findings: oval lesion < 5 cm with attenuation equivalent to that of fat (hyperechoic on US,
and hypodense on CT),
that abuts the anterior colonic wall,
surrounded by inflammatory changes,
and with a hypoechoic/hyperattenuating wall. A hyperdense/hypoechogenic central dot may be seen,
which represents a thrombosed vein.
1.12.
FOREIGN BODY
Although foreign-body ingestion is common,
complications such as intestinal perforation occur in less than 1% of cases.
The foreign body is usually a non-digestible component of food,
such as chicken bone,
fish bone or a toothpick.
- The rectosigmoid region is a common site of intestinal perforation by a foreign body.
- Pneumoperitoneum may not be seen due to progressive impaction of the foreign body in the intestinal wall,
with the site being covered by fibrin,
omentum,
or bowel loops,
which prevent leakage of gas or fluid.
2.
GENITOURINARY SYSTEM
2.1.
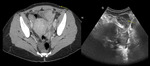
URETERAL STONES
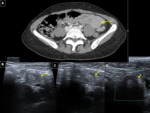
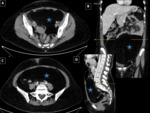
- Unenhanced CT is more accurate in detecting ureteral stones than US, both often showing hydronephrosis and a hydroureter as signs of obstruction. Fig. 15, Fig. 16
- US evaluation of the abdomen may demonstrate hydroureter.
If the bladder is distended,
the obstructing calculus may be visualized as an echogenic focus in the region of the ureterovesical junction.
Identification is improved by the creation of the twinkling artifact on Doppler images, which is rapidly changing red and blue colors behind the calcification due to "phase jitter" within the machine.
-CT images demonstrate a high attenuation calculus within the ureter,
with or without proximal ureteral dilatation.
Ureteral wall thickening and adjacent fat stranding may be present.
2.2.
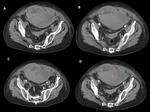
PYELONEPHRITIS
Is most commonly associated with an ascending genitourinary tract infection and is a clinical diagnosis; often times,
the US and CT findings are normal. Fig. 17, Fig. 18
- Imaging is useful in excluding complications,
such as abscess formation,
emphysematous pyelonephritis (typically in diabetics and immunocompromised patients),
or xanthogranulomatous pyelonephritis.
- CT findings include nephromegaly due to edema,
a striated or delayed nephrogram,
perinephric fat stranding,
and wall-thickening and enhancement of the renal collecting system.
Delayed appearance of the calyces may also be seen; however,
since pyelonephritis is often bilateral,
the comparison between the two kidneys may not be helpful.
- US may be normal.
But sometimes it shows nephromegaly and loss of renal sinus fat due to inflammation,
as well as loss of the corticomedullary junction.
The kidneys may be abnormally hyperechoic or hypoechoic.
3.
GYNECOLOGICAL SYSTEM
Transvaginal sonography is superior to a transabdominal approach.
3.1.
HEMORRHAGIC CORPUS LUTEUM
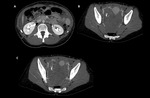
Imaging findings: Fig. 19, Fig. 20
- Thick and irregular walls (due to recent rupture or adherent blood clot).
- Internal contents of corpus luteum: anechoic or isoechoic at US.
- Color Doppler US depicts increased peripheral vascularity of the corpus luteum.
- Luteal cysts are often unilocular,
with thick,
crenulated and enhancing walls.
3.2.
FUNCTIONAL OVARIAN CYSTS
- Cysts ≥3 cm are considered pathologic.
- Uncomplicated non-hemorrhagic cysts are anechoic,
thin-walled,
unilocular masses exhibiting posterior acoustic enhancement.
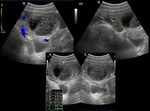
- Hemorrhagic ovarian cysts have varied sonographic appearances.
The most common one is a finely septated fishnet pattern or reticular appearance. Fig. 21
- Cyst rupture: larger amounts of echogenic peritoneal fluid may be seen.
- Hemorrhagic and non-hemorrhagic cysts are both avascular on color Doppler sonography.
3.3.
ADNEXAL TORSION
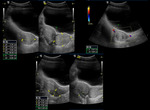
US findings: Fig. 22
- Increased size (> 4 cm) and volume of the involved ovary.
- Heterogeneous appearance (edema and hemorrhage).
- Associated cyst or mass.
- Multiple small follicles can be seen in the periphery of the enlarged ovary due to displacement from stromal edema à “string of pearls” sign.
- The torsed ovary often assumes a midline position,
either behind the bladder or cephalad to the uterus.
- Other features of adnexal torsion are twisted vascular pedicle,
ipsilateral deviation of the uterus to the side of the torsion,
and fluid.
The absence of ovarian blood flow in the color Doppler sonography can be helpful.
However,
arterial flow can be noted in the torsed ovary or the twisted vascular pedicle,
due to the dual blood supply from ovarian and uterine branch artery
3.4.
ECTOPIC PREGNANCY
Non-visualization of an intrauterine gestational sac on transvaginal ultrasound with a beta-hCG level greater than 2000 mIU/ml should raise the suspicion for ectopic pregnancy.
Presence of yolk sac or a live embryo with cardiac activity makes the diagnosis
3.5.
ACUTE PELVIC INFLAMMATORY DISEASE
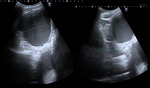
The imaging findings vary according to the severity of the disease,
but they may be normal in early conditions. Fig. 23
-US features:
- Enlarged and heterogeneous appearing ovaries.
- Thickened adnexal structures.
- Dilated fallopian tubes containing simple fluid or echogenic contents.
- Pelvic fluid collections.
- CT findings:
- Enlarged ovaries with abnormal enhancement.
- Dilated and fluid-filled fallopian tubes with enhancing wall from pyosalpinx.
- Stranding of the pelvic fat.
- Enhancement of the adjacent peritoneum.
- Pelvic abscesses in advanced cases.
- Similar findings can be seen involving the endometrium and cervix in endometritis and cervicitis.
4.
OTHERS
4.1.
ILIOPSOAS ABSCESS/ HEMATOMA
On CT scans,
an abscess/hematoma may manifest as enlargement of the iliopsoas muscle by an iso/low-attenuating lesion.
On MRI a hematoma will present with different imaging findings according to its evolution.
An abscess typically displays rim enhancement after the intravenous administration of contrast material at both CT and MR imaging.
Secondary findings include obliteration of the surrounding fascial planes,
bone destruction,
and gas bubbles
4.2.
RECTUS SHEATH HEMATOMA
A rectus sheath hematoma may be easy to diagnose in patients under anticoagulant therapy,
presenting with a painful palpable mass; however,
small non-palpable hematomas can clinically masquerade as diverticulitis and also occur in patients without anticoagulation.
Sonography and CT show a hemorrhagic mass within the sheath of the rectus abdominis muscle. Fig. 24, Fig. 25
4.3.
RETROPERITONEAL OR ABDOMINAL HEMORRHAGE
The spontaneous intra-abdominal hemorrhage is the extravasation of blood in the abdominal cavity without external trauma or iatrogenic causes. It can be located in the intraperitoneal or extraperitoneal space.
The CT is the diagnostic test of choice performing 3 phases (without contrast,
arterial phase,
and portal).
The origin of the bleeding can be visceral,
gynecological,
vascular or coagulopathy. Fig. 26
4.4 RETROPERITONEAL FIBROSIS
The retroperitoneal fibrosis is usually observed as a well-defined paraspinal mass with irregular edges,
isodense with respect to the muscle.
It starts around the aorta and the iliac arteries,
extending through the retroperitoneum and wrapping the ureters.
The intensity of enhancement of the mass after administration of contrast depends on the activity of the process.
Thus it is acute stages there is an intense enhancement with an increase of 20-60 HU after contrast,
while in chronic disease little or nothing is enhanced. Fig. 27
4.5.
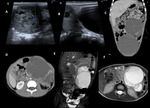
ABDOMINAL MASS.
A abdominopelvic mass may cause pain in the left iliac fossa due to the compressive effect on adjacent structures.
Fig. 28, Fig. 29, Fig. 30.