Learning objectives
Review the role of preoperative embolization of intracranial meningioma.
Illustrate the possible known complications and adverse effects of embolization.
Correlate outcomes with type of embolizing agents and other factors,
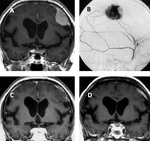
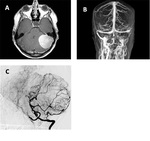
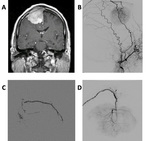
and present cases from our practice.
Background
Meningiomas are the most common benign intracranial neoplasm,
showing a prevalence of approximately 13% to 26% of adult intracranial tumors.[1]
Intracranial meningioma is a common pathology and,
therefore,
familiar to all neurosurgical units.
Surgical excision is the mainstream way of treatment.
Preoperative endovascular embolization is aimed primarily at reducing this vascularity via the dural arteries.
Though,
preoperative embolization of intracranial meningioma has been always controversial since it was first described.
With benefits as decreased blood loss and “softening of the tumor” during subsequent surgical resection....
Findings and procedure details
We’ve performed a structured literature review across Medline and Pubmed databases,
with concept map of terms:pre-operative,
meningioma,
embolization,
complications,
embolizing agent,
.with literature articles from 1993 to 2018 were retrospectively reviewed.
Inclusion criteria included prospective and retrospective in the aforementioned period in English,
Exclusion criteria included case reports with small number of cases “ less than 20 cases”,
or non English language articles.
Studies included are tabulated in [table1] including 25 studies,
with different techniques and variable embolizing materials.
Articles were screened for advantages of...
Conclusion
Preoperative embolization has been proven to be an optimal option for some specific cases of meningiomas,
meaning not all cases would benefit from it,
and therefore should be considered on a case-by-case basis.
The intraoperative complications,
duration and degree of resection are independable factors of embolization.
With complete devascularization managed to obtain a lower blood transfusion requirement,
considered an indirect measure of operative blood loss.
The use of small polyvinyl alcohol particles was more effective in devascularization than larger particles.
Needs of thorough devascularization of...
Personal information
Contact: Dr.
Sherif Mohsen Shalaby,
MSc
[email protected]
Diagnostic and Interventional Radiology Registrar,
National Institute of Diabetes and Endocrinology (NIDE),
Dar Al Fouad Hospitals (DAFH),
ERMED.
Egypt
Prof.
Dr.
Wael Shawaf,
M.D
Prof.
of Diagnostic and Interventional Radiology,
Maadi Military Hospital,
International Medical Center,
Cairo.
Egypt
References
Bondy M,
Ligon BL.
Epidemiology and etiology of intracranial meningiomas:a review.
J Neurooncol.
1996;29(3):197-205.
D.M.S.
Raper,
R.M.
Starke,
F.
Henderson,
D.
Ding,
S.
Simon,
A.J.
Evans,
J.A.
Jane,
K.C.
Liu.
Preoperative Embolization of Intracranial Meningiomas: Efficacy,
Technical Considerations,
and Complications.
American Journal of Neuroradiology 2014;35:1798-1804.
Dowd CF,
Halbach VV,
Higashida RT.
Meningiomas: the role of preoperative angiography and embolization.
Neurosurg Focus 2003;15:E10.
Alexiou GA,
Gogou P,
Markoula S,
Kyritsis AP.
Management of meningiomas.
Clin Neurol Neurosurg.
2010;112(3):177-182.
Gruber A,
Killer M,
Mazal P,
Bavinzski G,...

![Table 1: [table1] including 25 most outstanding studies, with different techniques and variable embolizing materials. References: Sherif M. Shalaby, MSc & Wael Shawaf, MD](https://epos.myesr.org/posterimage/esr/ecr2019/147126/media/784851?maxheight=150&maxwidth=150)
![Table 2: 4 cases of our practice [Table 2] References: Wael Shawaf, MD](https://epos.myesr.org/posterimage/esr/ecr2019/147126/media/784852?maxheight=150&maxwidth=150)