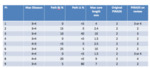
A total of 296 patients were identified.
Of the 296 patients who received MP-MRI 296 (100%) of those scanned had T2 and DWI sequences 290 (98%) received Gadolinium. 22 (7%) were technically limited scans either secondary to local metallic artefact i.e.
from a total hip replacement or secondary to patient claustrophobia.
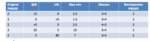
229 (77%) of reporters provided a three-dimensional prostatic size in their report and 292 (99%) calculated a prostatic volume.
124 (42%) did not provide a PSA density in their report (17 of these were not provided with PSA information in the first instance). 270 were allocated a PIRADS score in their radiology report.
123/270 patients (46%) were allocated PIRADS 1 or 2 (clinically significant cancer very unlikely or unlikely),
70/270 scored PIRADS 3 (intermediate) and 77/270 (29%) scored PIRADS 4 or 5 (clinically significant cancer likely or very likely).
PIRADS 1 & 2
Of the 123 men with a negative MP-MRI (PIRADS 1 or 2),
33 had a biopsy.
90 (33%) of the 270 did not have a biopsy.
The PROMIS trial suggests that a negative MP-MRI triage may allow 27% of men to avoid biopsy.
Our data compares favourably with 46% (123/270) of patients not requiring a biopsy based on radiological assessment.
Of the 33 PIRADS 1 or 2 who were biopsied,
6 men had Gleason 3+3 clinically insignificant cancer and 18 did not have cancer.
Clinically significant secondary definition ≥ 7 Gleason cancer was identified in 9 patients (7%) of 123.
Again this compares favourably with the PROMIS trial which demonstrated that 11% (17/158) of men with a negative MP-MRI had clinically significant cancer on biopsy.
We reviewed the 9 false negatives paying specific attention to cancer core length.
Of the 9 biopsies,
the maximum core length was less than 6mm in 5 cases.
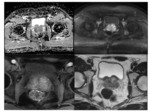
The MP-MRI scans of the 9 false negatives were also reviewed and retrospectively there were features to upgrade 4 (44%) cases to a higher PIRADS score (see Figure 2). 5 cases that were originally identified as MP-MRI negative PIRADS 2 remained PIRADS 2 on retrospective review.
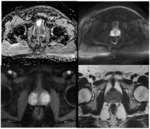
All of these cases had Gleason 3+4 disease or a maximum core length of <3mm (see Figure 3).
PROMIS demonstrated that all 17 MP-MRI negative cases with clinically significant cancer on biopsy had Gleason grade 3+4 or less with core lengths that ranged from 6–12 mm.
Of the 4 cases that were retrospectively radiologically upgraded to a higher PIRADS score,
3 were > 7 Gleason or > 6mm length and considered radiological misses on MP-MRI.
PIRADS 3
70 (26%) of the 270 men were allocated PIRADS 3 and 47 (67%) were biopsied.
18 (38%) of those biopsied had cancer and 13 (19%) of 70 were clinically significant by primary definition.
This compares well to the PROMIS data in which 21% of PIRADS 3 men demonstrated clinically significant cancer.
PIRADS 4 & 5
77 (29%) of 270 patients were allocated a PIRADS 4 or 5 score (clinically significant cancer likely or very likely),
73 (95%) of which had a biopsy.
56 (77%) of those biopsied demonstrated cancer - 37 (51%) of those biopsied were secondary definition clinically significant cancer (≥7 Gleason) and 31 (42%) were primary definition.
Comparatively the PROMIS trial demonstrated a positive predictive value of 51% for primary definition clinically significant cancer.
17 (23%) of those biopsied demonstrated insignificant cancer compared with PROMIS 24%.
17 (22%) of the 77 PIRADS 4 or 5 men went on to have a biopsy that did not demonstrate cancer.
Comparatively the PROMIS trial demonstrated 8% without cancer,
although 100% of PROMIS cases had a biopsy.
We reviewed the pathology of the 22% who were biopsied without demonstrable cancer and found that four histological patterns emerged.
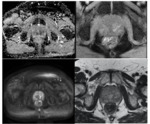
3 (18%) biopsies demonstrated high grade prostatic intraepithelial neoplasia (PIN,
see figure 4),
4 (24%) demonstrated inflammation (figure 5),
3 (18%) were suspicious but not diagnostic of cancer (figure 6) and 7 (41%) yielded normal prostatic tissue.
‘High grade PIN’ is a histological diagnosis characterised by prostate glands retaining a complete or partial basal cell layer lined by atypical cells with prominent nucleoli5.
Prostate adenocarcinoma by comparison is where the abnormal cells spread beyond the boundaries of the acinus and form clusters without basal cells.
In high grade PIN the basal cell layer is interrupted but present.
High grade PIN indicates a 21% risk of adenocarcinoma in subsequent biopsies and is considered the only histological cancerous precursor6.
High grade PIN is not associated with an elevated PSA.
‘Suspicious but not diagnostic of cancer’ indicates atypical small acinar proliferation (ASAP) and is not a pathological entity but instead represents diagnostic ambiguity.
Pathologic features suspicious but not definitive for malignancy are present.
The most common cause for ambiguity is small size of the foci of atypical glands6.
The National Institute for Clinical Excellence ‘Prostate cancer: diagnosis and management’ guidance states that of men who have a negative first prostate biopsy,
the risk of developing prostate cancer or that undersampled prostate cancer is already present is slightly higher if high grade PIN or atypical small acinar proliferation is present1.