Type:
Educational Exhibit
Keywords:
Infection, Acute, Education, MR, CT, Head and neck, Inflammation
Authors:
C. A. Robles1, A. Torres1, G. A. Miranda2, P. Orellana1, K. Bezares1, R. Núñez Flores1, M. López Ramírez1, J. de Grazia2, A. Salas1; 1Santiago/CL, 2Santiago, RM/CL
DOI:
10.26044/ecr2019/C-1023
Background
Fungal sinusitis corresponds to a wide spectrum of diseases which depends on 2 important factors.
The first is a normal immune state of the host,
that prevent the infection and dissemination of the disease.
The second is the virulence of the fungi that is implicated,
because only few fungi are truly pathogens to the humans.
The more common fungi that causes disease in humans are Aspergillus,
Bipolaris and Rhizopus.
The interaction between fungi and host ranges from a simple colonization to fatal infection.
Has to be noted that most of human are colonized by fungi but do not develop the infection,
thanks to a normal immunity.
Once infection is developed it can be classified as non-invasive and invasive,
which is an histological diagnosis.
Biopsy of the fungal infection,
necrosis,
normal mucosae and bone tissue has to be obtained for the pathological analysis.
The invasion is defined as the submucosal,
bone tissue and vessel compromise with hyphae.
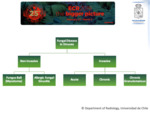
The wide spectrum of invasive and non-invasive fungal disease is summarized in Fig. 1 .