Fungus ball,
Allergic fungal sinusitis,
acute invasive,
chronic invasive and chronic granulomatous invasive sinusitis are 5 subtypes of fungal spectrum disease in sinuses that will be discuss shortly on this review.
Non Invasive Sinusitis
a.
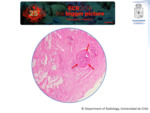
Fungus Ball:
Uncommon variant of fungal sinus disease also known as Mycetoma,
which is mainly seen in immunocompetent elderly patients.
Is more prevalent in females.
It’s thought to be caused by inefficient mucociliary clearance.
The fungi proliferate and incite an inflammatory response. Usually there is only one sinus compromised.
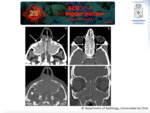
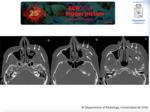
Imaging Findings: A non-expansive lesion centred in the maxillary sinus is usually seen,
followed by the sphenoid sinus. On CT calcification could be noted,
and secondary bone sclerosis of the sinus is described (Fig. 2).
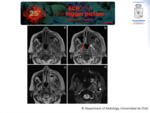
On MRI the signal intensity on different sequences is variable and reflects the content of the fungus ball. Usually a low intensity ball on T1WI and T2WI associated to mucosal enhancement with Gadolinium is reported.
The accumulation of paramagnetic elements shortens the relaxation times,
and explain the low intensity,
mainly on T2WI. (Fig. 3)
b.
Allergic Fungal Sinusitis:
Is the most prevalent form of fungal sinusitis,
mainly seen in atopic and immunocompetent young adults. Corresponds to an allergic response to fungi in all the sinus cavities,
with obstruction of the sinus outflow tracts,
developing an expansive inflammatory reaction that could lead to bone erosion.
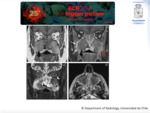
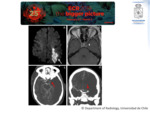
Imaging Findings: All the sinuses are compromised with expansive soft tissue mass.
CT demonstrates hyperdense mucin.
Erosions could be seen secondary to progressive expansion of the inflammatory reaction (Fig. 4).
MRI shows T2 signal void,
possibly to high concentrations of metals.
Mucosal linear enhancement could be seen (Fig. 5).
Invasive Sinusitis
a.
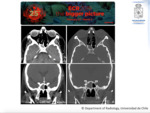
Acute Invasive Fungal Sinusitis
Fulminant fungal disease in immune compromised patients,
that could be fatal in days.
The mortality reported in literature is between 50 to 80%.
The clinical scenario could be seen in diabetic patients or severe neutropenia. The pathognomonic finding is histological invasion to the submucosae,
bone walls and vessels (Fig. 6).
The invasion could lead to thrombosis of the cavernous sinus,
orbital disease and brain abscess or cerebritis.
When vascular invasion occurs,
secondary infarcts develops.
Imaging Findings: Unilateral involvement with predilection of the ethmoid and sphenoid sinuses.
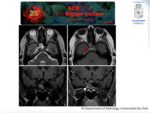
The CT findings demonstrate bone erosion and mucosal thickening (Fig. 7).On MRI lack of enhancement of the mucosae is noted secondary to necrosis.
Also is more sensitive to identify compromise in the nearby tissue (Fig. 8). The vascular invasion is noted in contrast enhancement study,
where thrombus can be identified (Fig. 9).
b.Chronic Invasive Fungal Sinusitis and Chronic Granulomatous Fungal Sinusitis
The literature on imaging findings in Chronic Invasive Fungal Sinusitis and Chronic Granulomatous Fungal Sinusitis is limited and the radiological differences between them are unclear,
and could be indistinguishable from malignancy.