Type:
Educational Exhibit
Keywords:
Oncology, Abdomen, Thorax, CT, MR, PET-CT, Complications, Education, Treatment effects, Cancer, Monoclonal antibodies, Toxicity
Authors:
V. Vani1, C. Maglia2, G. Giannetto3, L. Pusceddu3, A. Timpani4, V. M. Doronzio3, G. L. Desi4, D. Campanella3, D. Regge5; 1Turin/IT, 2Torino/IT, 3Candiolo/IT, 4Candiolo (TO)/IT, 5Candiolo-Torino/IT
DOI:
10.26044/ecr2019/C-1319
Findings and procedure details
The following is an exhaustive overview of clinical and radiological signs of the most significant irAEs,
according to the existing literature on clinical and imaging findings of irAEs induced by the currently approved ICIs,
administered both as monotherapy or in combination.
Furthermore,
we present examples of irAEs and provide a description of their incidence rate,
clinical,
laboratory,
anatomical and functional imaging findings,
relevant differential diagnoses,
and recommended management.
Enterocolitis
- Besides dermatologic toxicity,
it is the most frequent irAEs.
- More frequent for anti–CTLA-4.
- Median time to onset: 5-10 weeks after start of therapy.
- Clinical aspects: diarrhoea,
abdominal pain,
vomiting,
fever,
haematochezia and/or endoscopic evidence of colon inflammation; even asymptomatic.
Grade 3 and 4 colitis has a prevalence of 7–9% for ipilimumab and 1–2% for nivolumab and pembrolizumab; such grades are more frequent for combined treatment.
- <1% of patients have life-threatening events like bloody diarrhea and perforation.
- Two different computed tomography (CT) patterns:
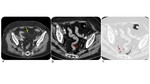
1. Diffuse colitis:
- diffuse colonic wall thickening
- mucosal hyperenhancement
- mesenteric vessel engorgement (early sign!) (Figure 3)
- with or without fluid filled distended colon
2.
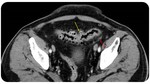
Segmental colitis:
- colonic wall thickening
- pericolic fat stranding
- mucosal hyperenhancement
- mesenteric vessel engorgement
- often superimposed to diverticulitis,
named also “segmenta colitis associated with diverticulosis”,
characterized by mild systemic symptoms and absence of fecal bacterial/leukocyte (Figure 4).
- It can be helpful to exclude ipilimumab–associated colitis if those findings are present on CT: pneumatosis or bowel wall edema,
halo or target signs.
- Differential diagnoses: Crohn’s disease (terminal ileum,
patchy transmural distribution),
ulcerative colitis (affects the colon increasing intensity distally,
diffuse crypt atrophy,
submucosal halo of fat),
infectious colitis (most commonly limited to the right colon,
wall thickening,
homogeneous enhancement),
and pseudomembranous colitis (marked circumferential or eccentric wall thickening).
- Histology: neutrophilic infiltrate,
lymphocytic infiltrate,
or a mix of both.
- Management: after stopping the drugs,
diffuse colitis is treated with high dose steroids while segmental colitis is treated with steroids and antibiotics.
Hepatitis
- Median time to onset: 6–14 weeks after start of therapy.
- Clinical aspects: asymptomatic elevation of ALT,
AST and total bilirubin has a prevalence of 5–10% for monotherapy and 25–30% for combined therapy (e.g.
ipilimumab +nivolumab); sometimes fever,
fatigue,
jaundice and changes of stool color.
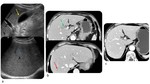
- CT,
Magnetic Resonance (MR): hepatomegaly,
periportal oedema,
periportal lymphadenopathy,
periportal T2-hyperintencity,
attenuated liver parenchyma (a decreased attenuation may obscure hepatic metastases and new geographic areas of low-attenuation may mimic metastases).
- Ultrasonography (US): prominent periportal echogenicity,
gallbladder wall oedema (Figure 5).
- Differential diagnoses: viral hepatitis (positive viral serology),
alcoholic liver disease (history of alcohol abuse,
steatohepatitis,
cirrhosis),
idiopathic autoimmune hepatitis (cirrhosis,
autoantibodies),
other medications.
- Histology: hepatocyte injury,
with acute hepatitis pattern or as bile duct injury (pattern of cholangitis).
- Management: depending on the grade of toxicity could be necessary to stop ICIs and to start steroid therapy; usually resolves in 4–6 weeks.
Pneumonitis
- Uncommon,
variable in onset and severity,
even fatal.
- Median time to onset: 8-12 weeks.
However,
it might occur at any point during treatment.
- Prevalence <1% for anti–CTLA-4,
1-6% for anti–PD-1/anti–PD-L1 (1-2% for melanoma,
3-6% for lung cancer) and 10% for combined ICIs treatment.
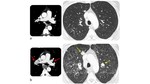
- Four different CT patterns:
1.
Cryptogenic organizing pneumonia (COP): patchy ground-glass opacities and consolidation in a subpleural,
peribronchial,
or band pattern,
sometimes accompanied by the reversed “halo sign”; it is the most frequent pattern.
2.
Non-specific interstitial pneumonia (NSIP): bilateral ground-glass opacities with reticular opacities,
traction bronchiectasis or bronchiolectasis,
and minimal or absent honeycombing in a basal distribution with subpleural sparing; it is the second most frequent pattern.
3.
Hypersensitivity pneumonitis (HP): centrilobular nodules and mosaic attenuation due to air trapping with an upper lobe–predominant distribution.
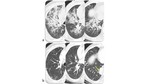
4.
Acute interstitial pneumonia/acute respiratory distress syndrome (AIP/ARDS): patchy bilateral ground-glass opacities with consolidation in the dependent lung; superimposed reticular densities (crazy paving)(Figure 6); ventrodorsal and craniocaudal gradient; end-stage lung disease with fibrosis characterized by honeycombing,
and bronchiectasis.
- Differential diagnoses: bacterial pneumonia (consolidations with air-bronchogram,
pleural effusion); drug-induced pneumonitis (review of medication history); radiation pneumonitis (threshold of 30-40Gy).
- Histology: can include cellular interstitial pneumonitis,
organising pneumonia,
and diffuse alveolar damage.
- Management: usually stop ICIs and start steroid therapy.
Sarcoid-like post-immunotherapy granulomatosis
- Median time to onset: 24 weeks;
- Prevalence 5-7%,
more frequent in melanoma.
- Sites most frequently involved by sarcoidosis: lung,
hilar and mediastinal lymph nodes,
and/or skin.
- CT: small nodules similar in size in a peribronchovascular distribution mostly in the upper lobes,
symmetric hilar and mediastinal lymphadenopathy (Figure 7).
- Clinical aspects: usually asymptomatic; may present with nonspecific skin lesions of erythema nodosum–like panniculitis; alternatively,
the patient may present with a triad of uveitis,
parotitis,
and fever; associated with favourable anti-tumor therapy response.
- Differential diagnoses: metastatic lymphadenopathy (may be asymmetric,
may show inhomogeneous enhancement with natural or treatment related necrosis); lung metastases (nodules have different size).
- Histology: histopathology from involved skin reveales florid non necrotising granulomatous inflammation.
- Management: usually stop ICIs and start steroid therapy.
Hypophysitis
- Median time to onset: 9 weeks.
- Prevalence 2-4%,
more frequent for ipilimumab.
- Clinical aspects: headache,
fatigue,
hypothyroidism,
hypogonadism and hypocortisolism.
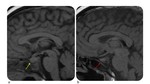
- MR: moderate enlargement of the pituitary gland,
convex aspect,
enlargement of the stalk or infundibulum and homogeneous contrast enhancement (Figure 8).
- Differential diagnoses: pituitary adenoma (asymmetric enlargement,
heterogeneous contrast enhancement,
loss of pituitary bright spot); pituitary metastasis (more frequent in melanoma,
breast cancer,
and lung cancer); lymphocytic hypophysitis (young women during pregnancy or postpartum period with headache,
visual impairment,
and ACTH deficiency).
- Management: depending on the grade of toxicity could be necessary to stop ICIs,
start hormone replacement therapy (HRT) and,
in some cases,
start steroid therapy.
Less common irAEs
Less common irAEs are: nephrotoxicity,
neurological toxicity,
cardiotoxicity,
pancreatic toxicity,
musculoskeletal and rheumatologic toxicity.