Breast Imaging-Reporting and Data System (BI-RADS) 3,
or “ probably benign” lesions are challenging with high inter-observer variation.
The accepted probability of malignancy of these lesions is within 2%.
However,
real-practice incidence of malignancy of BI-RAD 3 lesions is still under investigation.
It is known that the main role for mammography is the early detection of breast cancer in asymptomatic patients.
The efficacy of this screening test has been established by trials in which its ability to depict carcinoma,
both in situ and infiltrating,
has significantly reduced breast cancer mortality.
Breast ultrasound and MRI may be useful in the screening setting of high-risk patients,
including clinically palpable masses without imaging correlation where the probability of malignancy ranges between 0.1% to 4%.
The use of category 3 is reserved for specific findings that have a 2% probability of malignancy.
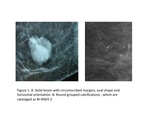
Findings include non-calcified circumscribed solid mass,
focal asymmetry,
and solitary group of punctuate calcifications for mammography (Figure 1).
BI-RADS 3 patients require a short-interval follow-up with periodic surveillance.
There are two major prompts for this short-term surveillance,
the first one is to confirm the benignity of the lesion as a non-changing finding; and the second one is the identification of rapidly growing cancers.
If these probably benign findings persist with no changes after 2-3 years or if they are seen to decrease or disappear the category should be changed to benign with a routine mammography screening recommendation.
Interval change is an unspecific feature shown by malignant and benign lesions.
Imaging change may be correlated with physical examination findings.
Short-interval follow-up identifies patients with benign lesions who should not undergo biopsy without decreasing the rate of malignancy detection.
The diagnostic challenge of these lesions should encourage the radiologist to perform a careful scrutiny and objectively determine whether the lesion truly merits a probably benign categorization.
As referred in the literature,
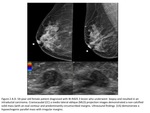
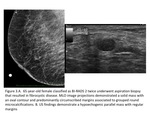
common BI-RADS 3 assessment errors include failure to use proper BI- RADS descriptors,
failure to perform a complete diagnostic work- up,
and overreliance on negative imaging findings (Figure 2 and 3).
Raza et al performed an imaging follow-up of 252 masses that documented stability for 6–24 months.
Aspiration of 24 masses revealed cysts.
Biopsy in 80 masses revealed three malignancies,
all of which were diagnosed within 6 months of the index examination,
all of them were smaller than 1 cm with negative nodes (negative predictive value 99.2%).
The decision to classify some mammographic lesions as Breast Imaging Reporting and Data System (BI-RADS) category 3–probably benign and recommend a short-interval follow-up,
usually at 6 months,
continues to be problematic for radiologists,
patients,
and referring physicians.
According to Baum et al short-term follow-up recommendations do not work as intended if patients do not return for follow-up imaging.
Patient compliance with recommendations for additional imaging and/or follow-up has been shown to be low after initial screening in a mobile setting.
Short-term follow-up is critical because it typically includes not only the first 6-month follow-up but also annual follow-up for up to 2 years.
There are many barriers to follow-up imaging.
Factors that reduce compliance are low educational level,
low patient concern for cancer,
poor general health,
and race.
Baum et al tried to determine (a) the frequency of BI-RADS 3 used in the American College of Radiology Imaging Network (ACRIN) Digital Mammographic Imaging Screening Trial (DMIST),
either at the time of screening mammography or after work-up,
(b) patients compliance with recommended follow-up examination,
and (c) the rate of a malignancy subsequently found in subjects for whom short-interval follow-up was recommended.
The additional economic impact of repeated diagnostic examinations is cost-effective (vs immediate biopsy) for US alone and/or for mammography alone.
Repeated examinations may lead to patient anxiety because a finding representing a potential cancer may be unresolved,
under current standards,
for up to 2 years.
The need to improve the diagnostic specificity of diagnostic mammography and ultrasonography (US) has led to interest in modalities that might extract distinguishing features between benign and malignant masses based on tumor biology.
Efforts to improve the specificity and cost-effectiveness of screening and diagnostic mammography led to the development and widespread acceptance of short-term follow-up of probably benign findings.
The purpose of the short-term follow-up algorithm is to reduce false-positive findings while retaining a high sensitivity for early stage breast cancer.
The aim of this study is to evaluate outcomes of patients with BI-RADS 3 lesions at third-level medical center.