♦ Introduction:
While lymphoma is a rather common malignancy,
spinal involvement is rare (accounting for 1-2% of extranodal lymphomas and 10% of all epidural tumors) [1].
Spinal lymphoma is mostly encountered in the setting of systemic disease,
usually non-Hodgkin lymphoma (NHL),
especially the diffuse large B-cell subtype [2].
Vertebral involvement in Hodgkin’s disease (HD),
can occur with extranodal stage IV lymphoma [3].
Spinal lesions are present in 1% of primary Central Nervous System (CNS) lymphoma and 3% of systemic CNS lymphoma [4].
Spinal lymphomas have been described in all age groups but mostly in the fifth to sixth decades of life,
with a male predilection of 1.6:1 [1].
High-grade B-cell NHL accounts for the majority of the cases of epidural lymphoma [5].
♦ Location:
While the axial and appendicular skeleton are similarly affected in primary osseous NHL,
secondary bone NHL involves mostly the axial skeleton.
Polyostotic disease is present in about 25% of the cases [6].
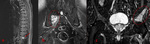
[Fig.1,
Fig.2]
Spinal lymphomas may be intraosseous,
extradural or intradural (extramedullary>intramedullary),
in descending order of frequency [7],
manifesting with intermittent pain,
mass-effect,
radiculopathy or progressive myelopathy,
depending on location.
Vertebral lesions occur most frequently in the thoracic spine.
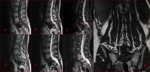
[Fig.3]
Epidural lymphoma is usually located in the thoracic spine,
more often dorsally [3].
In rare cases,
lymphomatous involvement of the spine may be predominantly epidural without significant vertebral involvement,
due to disease spread through the intervertebral foramina,
and can be seen with both NHL and HD [3].
♦ Imaging:
Conventional radiographs,
CT and MRI are the commonly used imaging modalities for depicting lymphomatous bone lesions.
MRI shows high sensitivity for assessing marrow replacement,
playing an essential role in osseous lymphoma imaging [2].
(18F)-fluorodeoxyglucose positron emission tomography (FDG -PET/CT),
is useful to exclude occult systemic lymphoma.
a. INTRAOSSEOUS SPINAL LYMPHOMA
- Imaging appearance varies from subtle or normal on radiographs to florid on other imaging modalities such as MRI,
due to marrow infiltration.
Further imaging for persistently symptomatic patients with normal radiographs is necessary to uncover underlying marrow disease.
- Radiographic appearance (diverse):
⇒ Vertebral NHL appears most frequently osteolytic,
showing a permeative or moth-eaten destruction pattern.
⇒ Vertebral HD involves osteoblastic /sclerotic changes more often (“ivory vertebra” sign).
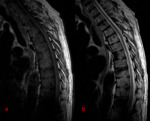
[Fig.4]
⇒ Aggressive behavior,
more commonly associated with HD: Cortical disruption,
accompanying soft-tissue mass and/or interrupted/lamellated periosteal reaction.
⇒ Pathologic fracture may be seen in both NHL and HD.
[Fig.5]
⇒ Bone sequestra are seen in approximately 10% of primary lesions.
⇒ Similar to radiographic features.
⇒ Superior visualization of cortical and trabecular destruction,
periosteal reaction,
sequestra and extra-osseous masses.
⇒ Contrast-enhancement: Depicting marrow disease and planning bone biopsy.
- MRI findings (similar in both NHL and HD):
⇒ Low T1-signal compared with normal bone marrow.
⇒ Variable T2-signal (hypointense,
isointense or hyperintense relative to fat.),
most commonly high signal intensity on fat-saturated T2-WI or STIR sequences. Areas of low intensity on T2-WI may be due to osteosclerosis or fibrosis within the tumor.
⇒ Different degrees of enhancement after intravenous contrast administration,
ranging from moderate to marked.
⇒ DWI-MRI: Restricted diffusion with low apparent diffusion coefficient values,
due to hypercellularity.
[8]
⇒ Superior evaluation of associated extra-osseous soft tissue mass.
Aggressive osseous lymphomas manifest with permeative growth and a soft tissue mass that is usually disproportionally large compared to cortical destruction; the cortex may even appear preserved.
- Pearls in differential diagnosis:
⇒ Differential diagnosis list:
-Other types of lymphoproliferative disease (myeloma,
leukemia)
-Other primary bone malignancies (osteosarcoma,
Ewing sarcoma)
-Inflammatory disorders (tuberculous spondylitis,
Langerhans cell histiocytosis)
-Other causes of “ivory vertebra” (osteoblastic metastases,
hemangioma,
chordoma,
Paget disease and SAPHO syndrome)
⇒ Relative absence of cortical destruction favors lymphoma over other bony neoplasms.
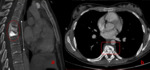
[Fig.6]
⇒ Lack of bone destruction or erosion on CT or X-ray suggests the diagnosis of spinal lymphoma [4].
However,
it lacks specificity and sensitivity [1].
⇒ NHL can rarely have an appearance overlapping with that of multiple myeloma,
with multiple focal lytic lesions.
⇒ Presence of bone sequestrum and/or crossing of discs and joints are more typical for lymphoma and infection,
but may also be seen in bony tuberculosis,
radiation necrosis and eosinophilic granuloma.
b. EXTRADURAL SPINAL LYMPHOMA
- Plain radiograph and CT have limited efficacy,
especially in the rare case of epidural lymphoma.
⇒ Epidural lymphoma demonstrates non-specific features,
similar to intraosseous spinal lymphoma.
[3]
⇒ “Wrap-around” sign: The characteristic appearance of diffuse spinal lymphoma with paravertebral involvement and circumferential epidural cord compression along with involvement of the posterior elements,
while preserving the intervening vertebral cortex.
[1]
- Pearls in differential diagnosis:
⇒ Differential diagnosis list:
-Other neoplastic disorders (leukemia,
metastases)
-Non-neoplastic disorders (abscess,
hematoma).
⇒ DCE-MRI demonstrates increased perfusion parameters in cases of diffuse tumor,
with a potential to differentiate malignant from benign disorders.[3]
⇒ Hematoma,
one of the major differential diagnoses for an epidural mass,
can be distinguished from lymphoma on the basis of the MR signal characteristics of blood [7].
⇒ Lymphoma is more likely to focally replace rather than infiltrate the bone marrow,
as opposed to leukemia [3].
⇒ Presence of the “wrap-around” sign is useful for differentiating lymphoma from metastases and multiple myeloma [3]
c. INTRAMEDULLARY SPINAL LYMPHOMA
⇒ Typical appearance: Expansile lesion,
appearing isointense to spinal cord on T1-WI and hyperintense on T2-WI.
⇒ Dural infiltration can occur either diffusely or focally (masslike) [3].
- Pearls in differential diagnosis:
⇒ Differential diagnosis list:
-Spinal cord inflammatory disorders (demyelination,
infectious myelitis)
-Granulomatous processes (such as neurosarcoidosis)
-Tumors with intramedullary deposits (dermoid tumor,
astrocytoma,
ependymoma,
hemangioblastoma,
ganglioneuroblastoma,
metastases) [3]
⇒ Lymphomatous leptomeningeal seeding often manifests with abnormal enhancement on the surface of spinal cord and nerve roots.
[5]
⇒ Spinal cord lymphomatous lesions may appear cystic and should be considered in the differential diagnosis of inflammatory processes.
[7]
♦ Treatment:
Therapeutic options encompass radiation therapy,
chemotherapy,
steroids,
stem cell transplantation and surgery [1].
It should be noted that steroid administration may “conceal” the abnormalities on CT and MR imaging.
[9]
♦ Post-therapeutic evaluation:
Imaging assessment of post-treatment response is widely achieved using MRI and FDG-PET/CT.
PET is superior to CT and MRI in distinguishing between viable tumour and post-therapy necrosis/fibrosis,
provided there was an FDG-avid mass on pre-treatment scan.
MRI characteristics indicating tumor response to treatment include decrease in both T2-signal intensity and contrast enhancement.
[2]
♦ Prognosis:
Primary bone lymphoma tends to exhibit better prognosis than secondary infiltration of the bone,
which is more common in the axial skeleton,
indicating extensive disease.
Vertebral and extradural lymphoma tend to have a better prognosis than intradural disease,
with the latter carrying a two-year survival rate of less than 50%.
[5]