Aims and objectives
Pancreatico-duodenectomy is the main surgical option in patients with resectable pancreatic adenocarcinoma but several post-surgical complications may onset,
postoperative pancreatic fistula (POPF) being the most common and responsible of 11-37% of cases [1-5].
The severity of POPF is judged according to the ISGPF classification scheme which divides them in types A,
B and C,
the latter two representing clinically relevant postoperative pancreatic fistulas (CR-POPF) [6-8].
A major risk factor in developing a CR-POPF in adenocarcinoma patients is the presence of a soft pancreatic texture as...
Methods and materials
In this retrospective study we analysed the preoperative MDCTs of 48 patients who underwent pancreatico-duodenectomy for adenocarcinoma between January 2011 and June 2018.
24 patients (15 males,
9 women; ages 41-75,
mean age 62) developed a clinically relevant postoperative pancreatic fistula,
and 24 (15 males,
9 women; ages 34-76,
mean age 60) did not.
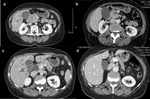
We included in this study only patients with histologically proven adenocarcinoma (Figure 1).
Exclusion criteria was the presence of significant motion artifacts.
All patients underwent a CT scan (Brilliance 64,
Philips),...
Results
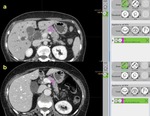
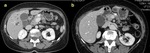
Mean attenuation values of the pancreatic parenchyma at the resection margin did not significantly differ between the two groups of patients (p>0.05) (Figure 3),
while several texture features did.
Considering the first order features,
kurtosis and entropy log2 (mean ± SEM of fistula group: 3.526 ± 0.067,
mean ± SEM of no fistula group: 3.323 ± 0.063; p = 0.0313) resulted to significantly differ between the two groups of patients (Table 1).
All the gray-level co-occurrence matrix (GLCM) and the grey-level run length matrix (GLRLM)...
Conclusion
Textureanalysis ofthe pancreatic parenchyma at the resection margin on the preoperativeMDCT shows significant differences between patients who develop pancreatic fistula or not.These preliminary findings could potentially change the management of these kind of patients providing an additional means of preoperative risk stratification and leading to a customization of the treatment for each patient.
However these results should be validated in a larger group of patients and in prospective studies.
References
1 Iacono C,
Verlato G,
Ruzzenente A,
et al.
Systematic review of central pancreatectomy and meta-analysis of central versus distal pancreatectomy.
Br J Surg.
2013;100(7):873–885.
2 Berger AC,
Howard TJ,
Kennedy EP,
et al.
Does type of pancreaticojejunostomy after pancreaticoduodenectomy decrease rate of pancreatic fistula? A randomized,
prospective,
dual-institution trial.
J Am Coll Surg.
2009;208(5):738–747; discussion 747–749
3 Bauman MD,
Becerra DG,
Kilbane EM,
et al.
Laparoscopic distal pancreatectomy for pancreatic cancer is safe and effective.
Surg Endosc.2018;32(1):53–61.
4 Wellner UF,
Kayser G,
Lapshyn H,...