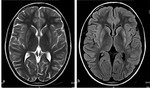
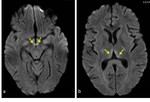
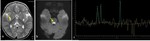
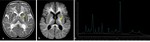
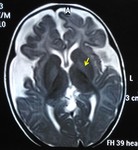
The basal ganglia have high energy requirements with rich blood supply; hence,
they are vulnerable to conditions that alter cerebral metabolism especially during childhood [3-5].
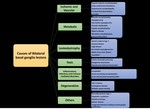
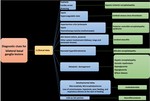
Differential Diagnosis of Bilateral Basal Ganglia Abnormalities (figure 2)
Ischemic and vascular causes:
Hypoxic Ischemic Encephalopathy (HIE)
HIE of the brain may be the result of circulatory or respiratory failure.
HIE occur in neonates as a result of perinatal asphyxia and hypotension [6].
- In neonates the pattern of injury differ according to the gestational age at birth and the severity and duration of injury.
- In preterm neonates: mild hypotension causes periventricular leukomalacia; severe hypotension affects the deep gray matter,
brainstem,
and cerebellum.
- In term neonates: mild hypotension causes parasagittal cortical and subcortical injury; severe hypotension leads to injury of the lateral thalami,
posterior putamina,
hippocampi,
corticospinal tracts,
and sensorimotor cortex.
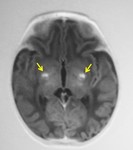
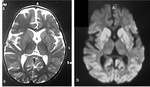
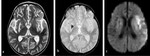
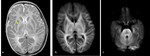
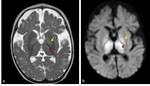
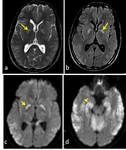
The affected areas exhibit diffusion restriction with hyperintense signal on T2WI and possible abnormal high T1 signal (figure 3).
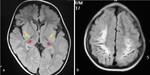
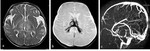
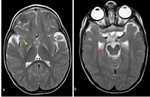
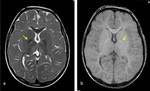
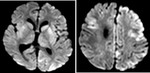
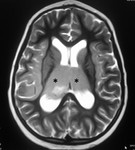
In the chronic stage,
gliosis and cystic changes ensue (figure 4) [6].
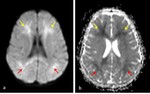
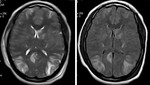
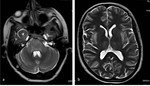
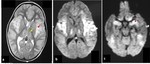
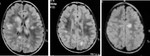
- In older children and adults,
mild HIE affect the watershed zones (figure 5).
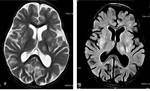
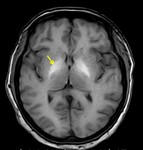
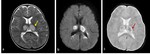
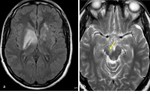
Severe HIE affects the gray matter structures,
including the cerebral cortex,
basal ganglia,
and hippocampi.
The thalamus and cerebellum may also be affected (figure 6) [6].
Deep Cerebral venous thrombosis
Thrombosis of the deep venous system can result in bilateral involvement of the thalamus and basal ganglia.
On MRI,
T2W and FLAIR hyperintense lesions involve the basal ganglia,
thalami.
Thrombus in veins appears hyperintense on T1W and T2W images.
The diagnosis can be confirmed by MRV (figure 7) [7].
Posterior reversible encephalopathy syndrome
Encephalopathy occurs secondary to hypertensive emergencies and may be related to sepsis or chemotherapy toxicity.
MRI reveals T2W and FLAIR hyperintensity involves the basal ganglia,
and hyperintense lesions of the hemispheric cerebral white matter predominantly in the parieto-occipital location,
cerebellum and brainstem (figure 8).
Areas of haemorrhage and diffusion restriction can also occur [8].
Cerebral thromboembolism
Bilateral thalamic infarct can result from arterial occlusion of the basilar top.
Artery of Percheron occlusion is another rare cause of bilateral thalamic infarct.
The resulting infraction is characterized by paramedian thalamic and rostral midbrain infarct with diffusion restriction on DWI [5,6].
Vasculitis
Ischemic lesions in the deep gray matter or white matter can result from vasculitis of the small perforating arteries (figure 9).
It can be associated with microbleeds or frank hemtoma and subarachnoid haemorrhage (figure 10) [9].
Metabolic:
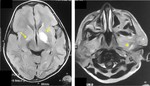
Bilirubin encephalopathy
Brain MRI of infants with chronic bilirubin encephalopathy shows abnormal signal in the globus pallidus,
hippocampus and cerebellum (figure 11).
In during the neonatal period,
the globus pallidus exhibit hyperintense signal on T1WI with diffusion restriction [10].
Osmotic myelinolysis
Central pontine myelinolysis and extrpontine myelinolysis are demyelination syndrome occur in alcoholics and malnourished individuals with electrolyte imbalance usually in cases underwent rapid correction of hyponatremia.
In central pontine myelinolysis,
there is a symmetric bat wing–shaped area of high T2 signal intensity in the central pons.
The ventrolateral pons and the pontine portion of the corticospinal tracts are charecteristically spared.
Extrpontine myelinolysis lesions are seen at basal ganglia and thalami,
showing T2 hyperintensity and T1W hypointensity (figure 12) [4,5].
Hepatic encephalopathy
In chronic hepatocellular disease,
there is accumulation of toxic substances (ammonia,
manganese) causing long-term toxic brain damage.
Bilateral hyperintense areas in the globus pallidus and substantia nigra on T1-weighted images is seen (figure 13).
Acute brain damage can occur due to acute hyperammonemia.
Brain MRI reveals bilateral symmetric swelling,
hyperintense T2 signal,
and restricted diffusion in the basal ganglia,
insular cortex,
and cingulate gyrus [4,5].
Wilson Disease
It is due to abnormal accumulation of copper.
On MR; areas of increased T1,
T2 signal in the putamen (a common finding),
globus pallidus,
caudate nuclei (figure 14).
T2 high signal at ventrolateral thalamus,
midbrain with a characteristic “face of the giant panda” appearance [3].
Wernicke encephalopathy
Results from a vitamin B1 (thiamine) deficiency.
MRI brain reveals symmetric T2 high signal in the medial thalamus,
periaqueductal area,
mammillary bodies,
and tectal plate (figure 15) [4].
Hypoglycemia
Severe hypoglycemia can be manifested by bilateral hyperintense T2 signal associated with diffusion restriction in the cerebral cortex,
hippocampi,
and basal ganglia [4].
Nonketotic Hyperglycemia
Typically,
in individuals with poorly controlled diabetes.
Lesions are seen at Globus pallidus or caudate bilaterally (rarely,
unilateral),
being hyperintense on T1-weighted images [4].
Leukodystrophy:
Basal ganglia can be affected in cases with leukodystrophy.
Neuroimaging has a key role in guiding the diagnostic workup.
Leigh’s disease,
Canavan disease,
non-ketotic hyperglycinemia,
glutaric aciduria type I are among leukodystrophies with fairly characteristic imaging findings.
Leigh Disease (subacute necrotizing encephalomyelopathy)
It is one of the mitochondrial diseases.
MRI reveals T2W hyperintense lesions involve the lateral portion of the bilateral putamen. White matter lesions and cortical atrophy are also noted (figure 16) [11].
Canavan disease
Affected children have macrocephaly.
MRI reveals diffuse white matter abnormality extending to subcortical regions associated with diffusion restriction.
Globus pallidus abnormality with sparing of the caudate and putamen is documented (figure 17) [12].
Glutaric aciduria type 1
Affected children have macrocephaly.
MRI reveals the characteristic pat wing appearance with basal ganglia abnormal T2 signal that could be associated with diffusion restriction.
Subdural haemorrhage can be seen (figure 18) [13].
Maple syrup urine disease
Affected neonates have predominant involvement of the cerebellar white matter,
cerebral peduncles,
posterior limb of the internal capsule,
thalami,
globe pallidi,
perirolandic cerebral white matter and dorsal brainstem.
Abnormal areas exhibit characteristic diffusion restriction (figure 19) [12].
Non ketotic hyperglycinemia
Globus pallidus,
the thalamus,
substantia nigra,
red nucleus and dentate can be affected in addition to white matter abnormality.
Diffusion restriction of the white matter of the ventral and dorsal brain stem that could extend to involve the subcortical white matter was described (figure 20) [14].
Fucociosis
Fucocidosis is a rare lysosomal strorage disease.
MRI reveals abnormalsignal of the globus pallidus being hperintense on T1WI,
hypointense on T2WI associated with hypomyelination (figure 21) [15].
Toxic Poisoning
Carbon monoxide mainly affect the globus pallidus.
Symetrical hyperintense T2 SI in both globus pallidi,
often with restricted diffusion.
Also delayed leukoencephalopathy and T1 shortening in the globus pallidus may be encountered (figure 22).
Manganese toxicity,
also seen with total parenteral nutrition
In Cyanide and methanol poisoning,
bilateral hemorrhagic necrosis of the putamen may be observed on gradient echo T2*W images.
Optic neuritis and white matter edema can be encountered in methanol poisoning [4,5].
Inflammatory,
infectious and immune mediated disorders:
Encephalitis
Encephalitis is a severe neurological disease.
Involvement of the thalamus or basal ganglia can occur in patients with encephalitis and commonly associated with respiratory viruses (figure 23),
especially in children.
Other causes include included herpes simplex virus (figure 24),
Mycobacterium tuberculosis and Creutzfeldt-Jakob disease (CJD).
CJD is cherecterized by bilateral involvement of the pulvinar sometimes extending to the dorsomedial thalamic nucleus (“hockey-stick” sign) [16].
Acute necrotizing encephalopathy (ANEC)
ANEC is a specific type of encephalitis seen in previously healthy young children usually of East Asian descent.
ANEC has characteristic imaging findings including multifocal,
symmetric lesions involving the thalami,
brainstem tegmentum,
supratentorial white matter,
and cerebellum.
Gradient MRI shows decreased signal in the thalami (arrows) indicating petechial haemorrhage (figure 25) [17].
Acute disseminated encephalomyelitis (ADEM)
Acute disseminated encephalomyelitis is a demyelinating disease that is characterized by encephalopathy that is associated with multifocal neurologic symptoms.
MRI reveals patchy areas of high T2 signal intensity predominantly affecting the subcortical and deep white matter.
Thalami,
basal ganglia and brain stem are frequently involved (figure 26)[18].
Degenerative
Fahr disease
It is a neurodegenerative disorder characterized by the abnormal deposition of calcium in the lentiform and dentate nuclei sometimes associated with thalamic and subcortical deposition of calcium.
These lesions are most conspicuous on CT; on MRI,
the lesions are hypointense on gradient echo T2*W images [4,5].
Neurodegeneration with Brain Iron Accumulation (Pantothenate kinase-associated neurodegeneration,
Hallervorden-Spatz disease)
Characterized by brain degeneration and excessive iron deposition in the basal ganglia.
Brain MRI reveals bilateral hypointense signal in the globus pallidus at T2WI with high signal intensity center “eye-of-the-tiger sign” [4,5]
Multiple system atrophy (MSA)
On MRI,
hypointensity of the putamen on T2WI with slit hyperintensity is seen in addition to brainstem and cerebellar atrophy,
“hot-cross bun” sign on T2WI due to degeneration of pontine fibers [4,5].
others
Neurofibromatosis Type 1
Neurofibromatosis is the most common phakomatosis (neurocutaneous syndrome).
On MR,
lesions of increased signal intensity on T1,
T2-weighted images,
the globus pallidus is the most common site of involvement,
but other lesions can also be found in the brainstem and cerebellum (figure 27).
They show no mass effect,
no surrounding edema,
and do not enhance after contrast injection [3-5].
Neurofibromatosis type I hamartomas can be differentiated from gliomas by their higher N-acetyl aspartate/choline,
N-acetyl aspartate/ creatine,
and creatine/choline ratios.
Neoplastic conditions
The thalami on both sides can be involved by astrocytoma leading to their enlargement with homogenous T2 signal abnormality with no enhancement (figure 28).
Optic pathway glioma can also involve the thalami.
This can occur in isolation or associating neurofibromatosis type 1[19]
Neuro-Behçet Disease
Behcet disease is inflammatory vasculitis.
lesions most commonly include the brainstem,
basal ganglia and thalamus.
Lesions show high SI on T2WI,
low SI on T1WI,
enhance after contrast injection,
associated with vasogenic edema (figure 29) [4].
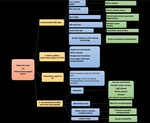
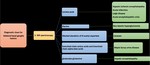
Diagnostic clues for bilateral basal ganglia lesions:
The presence of abnormal signal intensity in the basal ganglia at MR imaging necessitates a careful review of symptoms and personal and family history searching for possible risk factors along with proper describtion of the basal ganglia signal alterations and analysis of other brain areas (figure 30-33). The diagnosis is confirmed by proper laboratory investigations [4].