We present a pictorial review of various imaging features of tuberculosis,
using several modalities,
performed in the Radiology Department between March 2012 and March 2018.
We selected exams that document a wide range of different forms of extrapulmonary presentation of tuberculosis.
Tuberculosis: General considerations
- Epidemiology: Worldwide problem because of high prevalence increase among immunocompromised patients. Causal agent: Mycobacterium tuberculosis (the majority),
but small amount is caused by other Mycobacteria.
- Risk factors: Poor socioeconomic status,
poor hygiene,
undernutrition,
use of steroids, immunosuppression,
history of transplant and others risk factors.
- Respiratory system is most frequently involved.
- Others systems involved: musculoskeletal,
gastrointestinal,
hepatic,
spleen,
genitourinary,
breast,
lymph nodes,
central nervous system.
- The diagnosis is established by: Clinical data,
tuberculin skin,
test baciloscopy, molecular diagnostic tests, radiologic features,
Biopsy and Culture specimens.
- Treatment: anti-tuberculostatic agents administered for at least 6 months.
Extrapulmonar tuberculosis
Extrapulmonary tuberculosis is used to describe the isolated involvement of tuberculosis in an anatomical region other than the lungs.
The most common sites are the lymphatic system,
the genitourinary tract,
the bones and joints,
and the central nervous system.
Less frequently,
the peritoneum and other intrabdominal organs are affected.
Extra-pulmonary involvement may exist alone,
or associated with a pulmonary focus.
The most common presentation of extrapulmonary tuberculosis is the ganglionic form,
(35%),
and in most cases,
there is no active pulmonary involvement.
Extrapulmonary presentation is particularly associated with human immunodeficiency virus (HIV) infection (more than 50% of patients with this infection also develop tuberculosis).
The most common anatomical location of lymphatic tuberculosis is the cervical region,
but cases are also reported in the inguinal,
axillary,
mesenteric,
mediastinal and intra-mammary regions.
In the cervical region it is called scrofula,
a term derived from Latin meaning "ganglionic swelling."
Extrapulmonary tuberculosis results more often from hematogenous dissemination,
although it can also spread directly from an adjacent organ.
The symptoms depend on the affected organ.
In the majority of cases initial presentation is fever,
weight loss and malaise.
1.
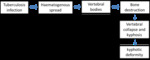
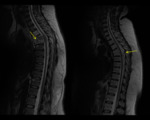
Pott’s disease
Tuberculosis of the spine is one of the oldest disease of humans.
Usually is secondary to extraspinal infection.
Fig. 18
The most frequently affected segments are: dorsal vertebrae,
lombar,
dorsolumbar and cervical.
Area affected: anterior of vertebral body.
Clinical manifestation: Gradual and increasing back pain,
kyphotic deformity of the dorsal/lumbar vertebraea, and weakness (lower limbs).
Fig. 1 Fig. 2 Fig. 3
Complications: - neurological - spine deformities - vascular (rare).
Fig. 4
Diagnosis: Epidemiology,
clinical manifestation,
biopsy,
culture and imaging (CT/MRI).
Differential diagnosis: pyogenic discitis; metastases.
Treatment: Tuberculostatic agents and surgery.
2.
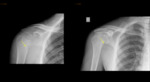
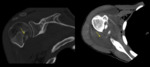
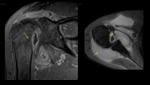
Extraspinal bone tuberculosis
- Rare.
- Clinical manifestations: chronic pain; fever usually absent; cold abscess; sequela- deformities.
- Challenging diagnosis.
- Long bones,
periarticular (hip and Knee +++)
- Haematological spread.
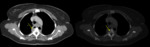
- Imaging: soft tissue oedema; bone destruction (periarticular); cold abscess; sequela- deformities. Fig. 5 Fig. 6 Fig. 7 Fig. 8
3.
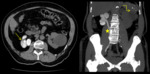
Intestinal tuberculosis
- The diagnosis of intestinal tuberculosis is a challenge,
because it can mimic other abdominal pathology.
- Early diagnosis and starting antituberculosis drugs or surgery are essential to prevent complication.
Fig. 9
4.
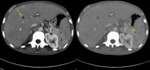
Hepatic and splenic tuberculosis
- TB Bacillus spreads through the hematogenically to the liver and spleen,
causing multiple micro abscesses. Fig. 10
5.
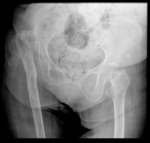
Renal tuberculosis
- From all the extra-pulmonary TB sites,
the urogenital system is the most frequently involved.
- Bacilli form intra-renal granulomas,
that,
when not treated,
progress to calcified caseum filling all the excretory system,
or a totally calcified non-fnctional kidney.
Fig. 11
6.
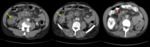
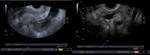
Pelvic tuberculosis
- The incidence of tubaric tuberculosis is increasing in the Western world.
- The clinical and laboratory findings may be non-specific and mimic other diseases,
including gynecological neoplasms.
- This entity commonly is associated with peritoneal tuberculosis,
involving the entire abdominal cavity,
a fact by which the two entities are studied together in most of the studies.
- The symptoms are usually nonspecific and,
even when the degree of suspicion is high,
establishing the diagnosis can be difficult.
- Pelvic tuberculosis can mimic clinical and laboratory ovarian carcinoma or other gynecological tumor.
Fig. 12
7.
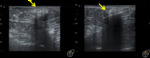
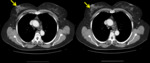
Breast tuberculosis
- Breast tuberculosis is a rare disease.
- Usually it is secondary to spread of disease from somewhere else,
mainly by axillary lymph node involvement.
- It can present as: nodular mastitis,
disseminated mastitis,
sclerosing mastitis and/or obliterans mastitis.
- In the nodular form of mammary tuberculosis,
this can simulate a carcinoma and in the disseminated form,
it is suggestive of an inflammatory carcinoma.
- The disease is rare,
particularly in males.
- The diagnosis is made histopathologically (granulomas with caseous necrosis and histiocytic inflammatory infiltrate),
and by microbiology direct and cultural procedures.
Fig. 13 Fig. 14
8.
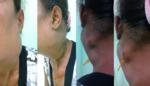
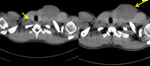
Tuberculous lymphadenitis
- The epidemiological characteristics of lymph node tuberculosis differ from pulmonary tuberculosis.
The clinical manifestations are variable.
- The diagnosis is a constant challenge,
largely based on clinical suspicion.
It is often difficult and late,
which increases morbidity and mortality.
- In the last decades,
thin-needle aspiration cytology has emerged as a simple method of diagnosing tuberculous lymphadenitis and has been replacing lymph node biopsy.
Fig. 15 Fig. 16 Fig. 17