Spectrum of lesions in CNS TB,
Meningeal:
- TB meningitis
- Miliary and leptomeningeal granuloma
Parenchymal:
- Tuberculous granuloma (tuberculoma)
- Tuberculous abscess
- Tuberculous encephalopathy
- Tuberculous cerebritis
- Non-osseous spinal cord tuberculosis
Complications:
- Vasculitis and infarction
- Cranial neuropathy
- Calvarial tuberculosis,
subdural and epidural abscess.
- Immune Reconstruction Inflammatory Syndrome(IRIS).
TB meningitis (TBM):
TB meningitis is the most common manifestation of CNS.
It may result from either haematogenous spread or rupture of Rich focus.
Generally,
pre-contrast MR imaging cannot detect pathological,
signal from meningeal inflammation or basal exudates in early stages.
However,
in later stages there may be widening of subarachnoid spaces with associated T1 and T2 shortening of CSF.
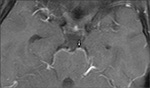
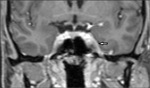
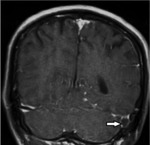
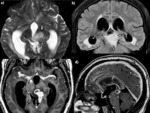
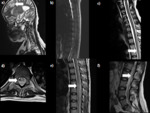
Post-contrast T1 images show diffuse meningeal enhancement around basal cisterns and sylvian fissures (Fig.3,4).
This appearance is nonspecific and has a wide differential diagnosis that includes meningitis from other infective agents,
inflammatory diseases such as rheumatoid arthritis,
and sarcoidosis and neoplastic causes.
Magnetisation transfer spin echo (MT-SE) imaging following contrast injection is superior to conventional post-contrast imaging in demonstrating meningeal inflammation.
Quantitative MT ratio is also of value in differentiation of TB meningitis from other chronic meningitis.
Significantly lower MT ratio is seen in TB meningitis than pyogenic and fungal meningitis and significantly higher MT ratio than viral meningitis.
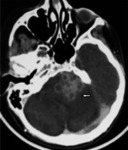
The most common complication is a communicating hydrocephalus and is caused by blockage of the basal cisterns by inflammatory exudates.
Ischaemic infarcts are also common,
being seen in 20 - 40% cases,
mostly within basal ganglia and internal capsule regions,
and result from vascular compression and occlusion of small perforating vessels.
Cranial nerve involvement is seen in 17 - 70% cases,
most commonly affecting second,
third,
fourth,
and seventh cranial nerves.
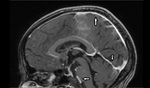
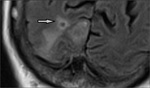
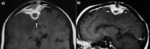
Parenchymal granuloma (Tuberculoma - Fig.5,6):
Tuberculoma is the most common parenchymal lesion in CNS TB.
This lesion may be solitary,
multiple,
or miliary,
and may be seen anywhere within the brain parenchyma,
although it most commonly occurs within the frontal and parietal lobes.
These granulomas usually involve the cortico-medullary junction and periventricular region as expected from haematogenous dissemination.
Non-caseating granuloma: It is usually iso-/hypo-intense on T1 and hyper-intense on T2-weighted images.
Homogeneous enhancement is seen with gadolinium.
Caseating solid granuloma: It is usually hypo-intense on T1 and strikingly hypo-intense on T2-weighted images.
This relative hypo-intensity is attributed to the granulation tissue and compressed glial tissue in the central core resulting in greater cellular density than the brain parenchyma.
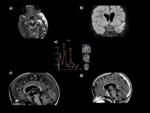
Granuloma with central liquefaction(Fig.12,13): It appears centrally hypointense on T1,
and hyper-intense on T2-weighted images with a peripheral hypo-intense rim on T2W images.
The low signal intensity of the capsule may be related to a layer of collagenous fibres with high protein concentration and low water content and a layer of outer inflammatory cells.
Gd-DTPA-enhanced T1W images show rim enhancement in caseating granulomas.
The oedema surrounding the granuloma is relatively less than pyogenic abscess.
However,
at times it is significant in the early stage.
MR spectroscopy shows prominent lipid peaks in tuberculomas as compared to other lesions such as metastasis and high-grade gliomas which shows lipid peaks in addition to other metabolite peaks like choline.
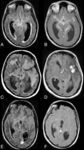
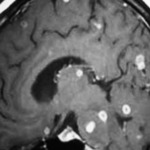
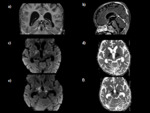
Disseminated/miliary tuberculoma(Fig.7.8): This condition is a subtle clinical event demonstrated in patients with military pulmonary tuberculosis who have no clinical brain involvement.
They may also occur in patients with TB meningitis.
It is characterised by diffuse infiltration of brain by multiple small granulomas (< 2 mm) which have high or low signal on T2-weighted images .
Post-contrast shows numerous round areas of intense enhancement.
Leptomeningeal granulomas show similar appearance; however,
they are seen located in the sulcal spaces and basal cisterns .
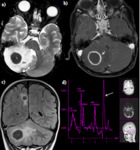
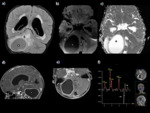
Tuberculous abscess(Fig.9,10,11):
Tuberculous abscesses are occasionally seen.
They occur in less than 10% of patients with CNS TB and are more common in the elderly and immunocompromised.
They may be solitary or multiple and are frequently multiloculated.
On imaging,
a TB abscess may be indistinguishable from a caseating tuberculoma or a pyogenic abscess.
However,
TB abscess has thinner and smoother enhancing walls,
is larger (> 3 cm in diameter),
and it has peripheral oedema and mass effect.
Differentiation of TB abscess from pyogenic abscess can be done with MR spectroscopy and magnetisation transfer (MT) imaging.
On MR spectroscopy,
TB abscess does not demonstrate aminoacids at 0.9 ppm as compared to pyogenic abscess which shows amino acids at 0.9 ppm.
MT ratio in a TB abscess is lower than that found in a pyogenic abscess.
Tuberculous encephalopathy:
Tuberculous encephalopathy,
a syndrome exclusively present in infants and children,
has been described by Udani and Dastur in Indian children with pulmonary tuberculosis.
The characteristic features of this entity are the development of a diffuse cerebral disorder in the form of convulsions,
stupor,
and coma,
without signs of meningeal irritation or focal neurological deficit.
Pathologically,
there is diffuse oedema of cerebral white matter with loss of neurons in the grey matter.
Neuroimaging shows severe unilateral or bilateral cerebral oedema.
On T2-weighted images,
hyper-intensity is seen in white matter suggesting myelin loss.
These patients also show diffuse alteration of MT ratio in white matter which reverts back to normal after clinical recovery.
Tuberculous cerebritis:
TB cerebritis is rare but has specific clinical,
radiological,
and pathological manifestations.
The involved areas show extensive inflammatory exudates,
Langerhans’ giant cells,
reactive parenchymal changes,
and diffuse caseating and noncaseating microgranulomas in the cortex.
On MR imaging,
focal cerebritis appears hypo-intense on T1,
hyper-intense on T2 and small areas of patchy enhancement on post-contrast scan.
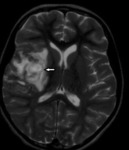
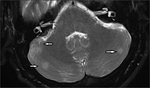
Vasculitis and infarction (Fig.14,15,16):
Intracranial vaculitis is a common finding in patients dying from TB meningitis and a major factor contributing towards residual neurological deficits.
Vasculitis is initiated by direct invasion of vessel wall by mycobacteria or may result from secondary extension of adjacent arachnoiditis.
Infarction resulting from vascultits is more common in infants and children and is most frequently seen at basal ganglia,
cerebral cortex,
pons,
and cerebellum.
The middle cerebral artery territories are commonly affected and the infarcts are frequently bilateral. MR imaging shows areas of hyper-intensities on T2-weighted images.
Diffusion weighted images are the gold standard in acute infarctions seen as increasing hyperintensity with increasing b values.
Cranial neuropathies:
Cranial neuropathies are seen commonly in association with TB meningitis.
These are partly due to vascular compromise resulting in ischemia of nerve or may be due to entrapment of nerves by the exudates.
Large tuberculoma may also compress the nerves,
resulting in compression neuropathy.
Commonly affected are II,
III,
IV,
and VII cranial nerves. On MR imaging,
the affected nerves appear thickened and may show hyper-intensity on T2-weighted images.
On contrast,
the proximal portion of the nerve root is commonly affected and may show enhancement .
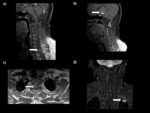
Non-osseous spinal cord tuberculosis (Fig.18,19):
Non-osseous spinal cord tuberculosis can occur in the form of tuberculomas.
Extramedullary lesions are more common; of them,
the majority being extradural.
Intramedullary tuberculomas are very rare.
Cervico-thoracic cord is commonly involved.
The pathophysiology of spinal meningitis is similar to that of TBM: a submeningeal tubercle forms during primary infection and ruptures into the subarachnoid space eliciting mediators of delayed hypersensitivity.
As with intracranial lesions,
there is granulomatous inflammation with areas of caseation and tubercles with eventual development of fibrous tissue in chronic or treated cases.
The clinical features are indistinguishable from those of any extramedullary or intramedullary tumour,
although acute worsening may occur.
MRI features include CSF loculation,
and obliteration of the spinal subarachnoid space with a loss of outline of the spinal cord in the cervico-thoracic spine,
and matting of the nerve roots in the lumbar region.
Sometimes,
patients who appear normal on unenhanced MRI images may show nodular,
thick,
linear,
intradural enhancement,
often completely filling the subarachnoid space on post contrast images.
Spinal cord involvement in the form of infarction and syringomyelia may occur as a complication of arachnoiditis.
Parenchymal TB myelitis and tuberculoma formation may also occur .
Calvarial tuberculosis,
subdural,
and epidural abscesses (Fig.17):
Calvarial involvement in tuberculosis is rare.
Before the advent of effective chemotherapy,
calvarial tuberculosis was estimated to represent 0.2 - 1.3% of all cases of skeletal tuberculosis.
About 50% of the cases reported in the literature were in patients younger than 10 years,
and 70 - 90% were younger than 20 years.
The disease is rarely seen in infants.
It is believed that calvarial tuberculosis occurs by haematogenous seeding of bacilli into the diploic space.
Lymphatic dissemination of tuberculosis,
common in other bones,
is not thought to occur in the skull.
Tuberculosis may present as a subgaleal swelling (Pott’s puffy tumour) with a discharging sinus when the outer table is involved .
Involvement of the inner table is associated with formation of underlying extradural granulation tissue.
MR imaging,
in most cases,
leads to a conclusive diagnosis.
Proton density and T2-weighted images show a high signal- intensity soft-tissue mass within the defect in bone.
This may project into the subgaleal and/or epidural spaces and show peripheral capsular enhancement on the contrast-enhanced image .
MR imaging is sensitive in demonstrating changes in the meninges and the ventricular walls and in detecting parenchymal foci of involvement.
Dural and subdural pathology: Tuberculous pus formation occurs between the dura and the leptomeninges and may appear loculated.
It appears hyper-intense on T2W and iso- to hypo-intense on T1W images.
The dural granulomas appear hypo- to isointense on T2W,
and iso-intense on T1W images.
Rim enhancement can be seen on post-contrast images.
Epidural TB: Lesions generally appear to be iso-intense on T1W images,
and have mixed intensity on T2W images.
In post-contrast images,
uniform enhancement can be seen if the TB inflammatory process is phlegmonous in nature whereas peripheral enhancement is seen if true epidural abscess formation or caseation has developed.
Epidural tuberculous abscess may occur as primary lesions or may be seen in association with an underlying tuberculous focus.
Tuberculosis - Immune Reconstitution Inflammatory Syndrome (Fig.20):
It is an excessive immune response against Mycobacterium tuberculosis that may occur in either HIV-infected or uninfected patients,
during or after completion of anti-TB therapy.
In HIV-infected patients it occurs after initiation of antiretroviral therapy independently from an effective suppression of HIV viremia.
There are two forms of IRIS: paradoxical or unmasking.
Paradoxical IRIS is characterized by recurrent,
new,
or worsening symptoms of a treated case.
Unmasking IRIS is an antiretroviral-associated inflammatory manifestation of a subclinical infection with a hastened presentation.
The pathogenesis is incompletely understood and the epidemiology partially described.
No specific tests can establish or rule out the diagnosis.
Treatment is based on the use of anti-tuberculosis drugs sometime with adjunctive corticosteroids.
Mortality is generally low.
Paradoxical neurologic TB-IRIS is a possibly life threatening con- dition and symptoms tend to manifest later than in forms not in- volving the central nervous system,
generally 5-10 months after ART initiation.
Neurologic TB-IRIS generally presents with new or worsening meningitis and/or features of raised intracranial pres- sure,
due to enlarging cerebral tuberculomas or intracranial ab- scesses; mortality is high and ranges from 12% to 25% .
It may also present with spondylitis,
epidural abscesses,
and radicu- lomyelopathy.