Men with testicular cancer may experience a variety of symptoms or signs,
or do not have any of these changes.
Testicular and scrotal ultrasound is the primary modality for imaging most of the male reproductive system.
It is relatively inexpensive,
quick,
can be correlated quickly with patients signs and symptoms,
and most improtantly,
does not employ ionising radiation.
The paired testicular arteries arise directly from the abdominal aorta,
just below the origin of renal arteries and are drained by pampiniform plexus,
wich continue as the testicular veins.
The right testicular vein directly drains into the inferior vena cava,
while the left testicular vein drains into the left renal vein. Lymphatic drainage of the testes follow the testicukar arteries back to the paraaortic lymph nodes. Because of venous and lymphatic drainage pathway,
retroperitoneal lymph nodes are initial landing station for testicular cancers. Lymphoma and leukemia,
occasionally spread to the testicules.
Staging of cancer is the main objective of cancer screening,
and considered the most important predictor of survival,
where cancer treatment is primarily determined by staging.
Testicular malignancy has one of the most complete and thorough staging systems among genitourinary cancers.
It combines clinical,
pathologic,
radiologic and serum tumor marker components.
The staging system commonly used the International Germ Cell Tumor Consensus Conference Classification and the American Joint Committee on Cancer,
is a TNMS- based T-tumor,
N-node,
M-metastases,
S-serum markers classification because progression can also be monitored by the level of specific serum markers : AFP,
HCG and LDH. Whereas surgical pathology determines the T category of the neoplasm,
imaging plays a critical role in determining the N and M components of testicular tumor staging.
N category is determined by the extent of retroperitoneal lymphadenopathy,
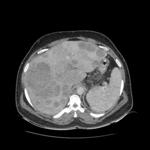
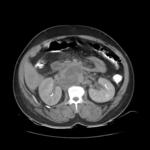
and M category describes distant metastases.Roman numeral stage grouping divides testicular cancer into three major groups on the basis of TNMS characteristics: tumor limited to the testis are stageI,those with retroperitoneal nodal involvment are stage II (fig 8),
and those with distant disease are stage III (fig7).
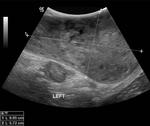
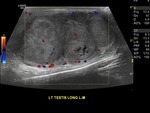
Ultrasound imaging of the testes represents the reference standard imaging evaluation,
with near 100% sensitivity when combined with physical examination. Testicular tumors are typically well defined and hypoechoic compared with normal testicular tissue but can be heterogeneous with calcification or cystic changes.
Increased vascularity of lesion is not specific to testicular tumors.
In cases in which the diagnosis is in question,
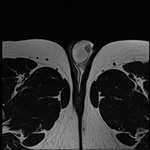
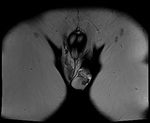
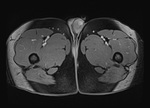
additional information can be gained with MRI.
Solid testicular tumors have lower signal intensity on T2-weighted MRI in contrast with the high signal intensity of normal testicular parenchyma. The sensitivity and specificity of MRI in differentiating beginn from malign intratesticular lesions were 100% and 87,5%.
The role of MRI of the testis in place of ultrasound remains to be clearly determined.
However,
it offrs reliable and detailed information in the case of equivocal ultrasound findings.
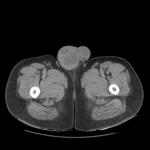
The accuracy of MRI for assigning pathologically confirmed T category is abou 92%.
(Fig1,2,3,4)
Differentiation of stage I and stage II or III disease can only be accomplished with cross-sectional abdominal imaging .
CT of the chest is the imaging procedure of choice for staging testis cancer.
. Although abdominal CT offers excellent anatomic resolution of the retroperitoneum,
the high dose of radiation generated and the relatively young age of testicular cancer patients have served as an impetus to evaluate MRI as a potential modality for retroperitoneal lymph node evaluation.
MRI with intravenous contrast administration is the references standard for evalution of retroperitoneal lymphadenopathy and abdominal viscera.
Staging of retroperitoneal disease depends on nodal size.
Although MRI excels at identifying and detremining the diameter of retroperitoneal lymph nodes,
this modality cannot differentiate a lymph node that is infiltrataed with malignant tissue from a lymph node that is beging.
As a result,
malignant lymph nodes are identified base on size criteria,
nodes 8 mm or larger should be considered suspicious,
especially in higher risk patients who have lymphovascular invasion or T category ≥ II.
Nuclear medicine studies have also faleen out of favour because of their ionising radioation.
The primary goal of cancer imaging is accurate disease characterization at diagnosis and through all stages of management. Knowledge of the disease and diagnostic performance characteristics of each technique is critical to identify the appropriate modality for staging disease and monitor for treatment response and and recurrence that may need further intervention.