Aims and objectives
Introduction:
Misidentification of patients should be a ‘never event’ in radiology departments; however in a large teaching hospital in Dublin and almost all other hospitals nationally in Ireland there are several reports per annum of patients receiving wrongful exposures to ionising radiation.[1] Where there is a risk of a patient being misidentified in a radiology department there is also a risk to the patient’s safety as they may receive a wrongful exposure to ionising radiation and this must be addressed.
Checklists have been shown to...
Methods and materials
A baseline audit was carried out to assess radiographer compliance with the local three point identification policy in the radiology department.
This audit was carried out by the radiation safety team.
This team was set up in order to improve standards on patient’s safety related to ionisation radiation.
The radiographers in the department where unaware that the initial audit was being carried out,
this was done in order to ensure that the results were a true representation of how the radiographers carried out the triple...
Results
During this campaign three audits were carried out.
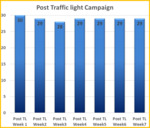
The initial baseline audit established radiographer compliance with the local three-point identification policy results prior to any intervention are demonstrated in Fig.
[3].
This graph shows only 60 percent of three-point ID checks were carried out in accordance with the local three-point identification policy.
These results showed that there was a need for improvements in the way in which identification checks were carried out on patients prior to them receiving an exposure of ionising radiation.
The audit...
Conclusion
The purpose of this study and audit was to assess the effectiveness of a safety checklist in reducing the misidentification of patients prior to a medical exposure of ionising radiation.
This was anticipated to reduce the number of radiation incidents occurring in a local radiology department in the Republic of Ireland.
Safety checklists and timeouts have proven to improve patient safety.
This has been demonstrated effectively with the World Health Organisation’s theatre time out and checklist and the Society and College of Radiographers,
(SCOR) PAUSED...
References
[1] Medical Exposure Radiation Unit (MERU) Incidents reported to medical exposure radiation unit in Diagnostic Radiology(including nuclear medicine) and Radiotherapy.
Dublin.
2015.
11p
[2] Medical Exposure Radiation Unit (MERU) National Radiation Safety Committee Patient Radiation Protection Manual.
2018 [Online 2018]
[3] World Health Organization (WHO) WHO Guidelines for safe surgery 2009 – safe surgery saves lives.
Geneva Switzerland.
2009.
133p
[4] Society and College of Radiographers (SCOR).
Have you paused and checked? IR(ME)R.
2016 (Online 2018)
[5] World Health Organisation.
2007.
Patient Safety Solutions.
(1)2....