Keywords:
Workforce, Education and training, Safety, Medico-legal issues, Audit and standards, Fluoroscopy, CT, Conventional radiography, Radioprotection / Radiation dose, Radiographers, Quality assurance
Authors:
A. Doyle, J. J. Binghay, R. crawley; Dublin/IE
DOI:
10.26044/ecr2019/C-3548
Methods and materials
A baseline audit was carried out to assess radiographer compliance with the local three point identification policy in the radiology department.
This audit was carried out by the radiation safety team.
This team was set up in order to improve standards on patient’s safety related to ionisation radiation.
The radiographers in the department where unaware that the initial audit was being carried out,
this was done in order to ensure that the results were a true representation of how the radiographers carried out the triple identification check.
The audit focused on the three point ID check and whether or not the radiographers were filling it out in accordance with the local three point identification policy.
Radiographers only were audited as it is their responsibility to ensure the correct patient is identified prior to medical exposure of ionising radiation.
This audit looked at the way in which the radiographers checked the patient’s identification,
i.e.
by asking the patient what their name,
date of birth and address was or by checking the patient’s identity bracelet in incidents were the patient was unable to identify themselves.
The audit also looked at the process in which the radiographers documented and recorded completion of this task in accordance with the local identification policy i.e.
was the radiographer ticking each box and signing the form prior to the exposure of ionising radiation being carried out.
The audit was only carried out in areas of the department where ionising radiation is used,
for example,
CT,
General X-Ray,
Nuclear Medicine and Fluoroscopy.
This audit established intermediate compliance [Fig.
3] in carrying out the three point identification check which may explain why patients had received wrongful exposures to ionising radiation.
This intermediate compliance needed to be addressed as 100% compliance was needed.
After carrying out some research it was decided a checklist should be introduced on the topic as they have been shown to improve patient safety and healthcare professionals working standards,
this has been demonstrated effectively with WHO’s theatre checklist [2] and Society and College of Radiographer’s (SCOR) PAUSED and checked checklist.[3]
With the permission of the SCOR,
the radiation safety team adapted their Paused and Checked checklist in order to comply with the department's local rules and the national Medical Exposure Radiation Unit (MERU).
The PAUSED and Checked checklist which was created was then launched with the aim to improve conformity amongst radiographers with triple identification checks [Fig.
1].The checklist was launched by holding a department meeting with all of the radiographers in order to explain the checklist and make sure all staff understood and were aware of the PAUSED and checked checklist.
Posters of the PAUSED and checked checklist were also displayed across the department in every area where ionising radiation is used to ensure that all radiographers were constantly reminded of it.
A re-audit of 30 radiographers were then carried out each week for 7 weeks after the PAUSED and checked checklist was launched.
This re-audit showed improvements but revealed variations in practices in applying the triple identification checks [Fig.
3].
As an intervention,
a specific initiative was launched to address this element.
This initiative was called the traffic light campaign.
A poster and prompt cards were made as a memory aide for radiographers on how to effectively adhere to patient identification policy [Fig. 2].
The prompt cards included “Essential points to remember” which would prompt the radiographers to carry out the three point identification checks in accordance with the local three point identification policy.
This traffic light campaign was again launched by a staff meeting and the poster and prompt cards were placed in every area where ionising radiation is used.
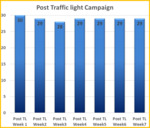
After this implementation a follow-up audit was initiated [Fig.
4] This audit was carried out each week for 7 weeks on 30 Radiographers a week.