INTRODUCTION
Intracranial ring enhancing lesions of different etiologies have a similar appearance on conventional MRI.
These lesions may present as solitary or multiple and are characterized by a contrast enhancing halo with a non-enhancing center.
"MAGICAL DR" (Fig.
2),
is a mnemonic used to help remember the differential diagnosis.

Fig. 38
In this pictorial review,
CT and particularly MRI findings of intracranial ring enhancing lesions are addressed and the most important imaging features for their differential diagnosis are presented.
As we approach a ring-enhancing lesion,
there are some fundamental points that are important to analyze in order to achieve the correct diagnosis such as clinical features,
medical history and radiologic findings (Fig.3).
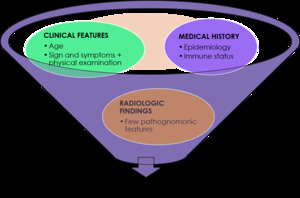
Fig. 36

Fig. 3
METASTASIS
- Metastatic tumors are the most common intracranial neoplasms in adults and frequent primary sites are lung,
breast,
gastrointestinal and genitourinary as well as melanoma.
- Metastatic lesions are typically subcortical,
occurring in or near the gray matter-white matter junction,
and are usually associated with severe perilesional edema.
These deposits are often solid nodular lesions that may become ring-enhancing possibly because of necrosis.
- They usually appear as small (< 2cm) circumscribed lesions near the gray matter–white matter junction.
These ring-enhancing lesions usually present with thick irregular wall (thicker than 10mm at least in some area) with a shaggy inner margin,
they can also be multilocular and have complex ring patterns.
- Metastases from malignant melanoma may demonstrate T1 hyperintensity because of hemorrhagic or melanin components of the lesion.
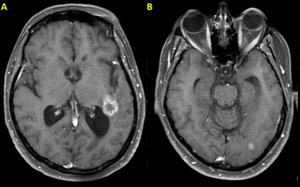
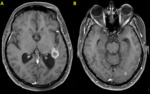
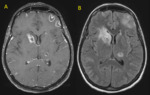
Fig. 12: Brain metastases in a 41-year-old woman with ovarian tumor. Axial post-contrast T1 MR images (A) and (B) demonstrate metastatic deposits, the largest lesion with ring-enhancement adjacent to the left posterior horn of the lateral ventricle.
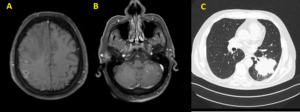
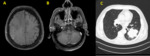
Fig. 13: Brain metastases in a 60-year-old man with lung cancer. Axial MR images show ring-enhancing lesions (A) as well as nodular lesions (B). Chest CT images (C) demonstrate a large spiculated mass in the left lung.

Fig. 4
ABSCESS
- Hematogenous abscesses typically manifest as cortical or subcortical lesions with cavitation.
- Deep white matter ring-enhancing lesions,
especially those with mass effect and surrounding vasogenic edema,
are most often either primary neoplasms or abscesses
- Pyogenic infections of the CNS usually arise from septic emboli transmitted hematogenously and after an initial unorganized inflammation or cerebritis,
the successful immune response will progresses to form an organized abscess.
- Multiple pyogenic brain abscesses are common in patients with human immunodeficiency virus infection,
organ transplant recipients,
intravenous drug abuse,
chemotherapy for lymphoma,
congenital cardiac defects or prosthetic cardiac valves and diabetes.
- The ring-enhancing lesion of a cerebral abscess is classically described as having a smooth inner margin and a smooth outer margin.
Abscess rim is typically hypointense on T2-weighted images (90%).
- The dual or double rim sign consists of two concentric rims surrounding the abscess cavity,
the outer one is hypointense,
and the inner one is relatively more hyperintense and it is seen on MRI (both SWI and T2) in approximately 75% of cerebral abscesses,
helping in differentiating an abscess from a glioblastoma (GBM).
- Abscess presents high signal intensity on diffusion-weighted image and low signal intensity on the apparent diffusion coefficient map.
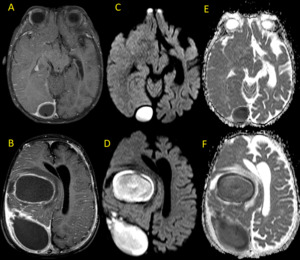
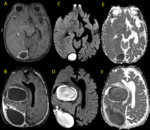
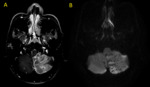
Fig. 14: Multiple abscesses in a 2 year-old child. Axial MR images show oval ring-enhacing lesions (A) and (B) with central restricted diffusion (C-F)

Fig. 5
GLIOBLASTOMA
- Glioblastomas may form unilocular lesions,
but more often they are complex,
multilocular,
thick walled,
ring-enhancing masses.
They are usually large in size and are often located deep in the white matter.
They also tend to cross the midline by infiltrating the white matter tracts of the corpus callosum.
These tumors often involve the corpus callosum and create bilateral hemispheric patterns (butterfly appearance).
Primary CNS lymphoma can also show this pattern.
- GBM characteristically has prominent neovascularity with abnormal blood-brain barrier.
The enhancing rim,
which contains the greatest concentration of neovascularity,
is often thick,
wavy or undulating,
and has a shaggy inner margin.
- These tumors often show increased perfusion and a shortened mean transit time.
-
GBM often shows the pseudopalisade sign.
Microscopically,
it consists on many of similar sized,
whole and soft elliptical bubbles that resembled mastoid cells.
On MRI,
there is irregular enhancement of the margins of the lesion but not at the centre.
Pseudopalisades were shown to be associated with necrosis.
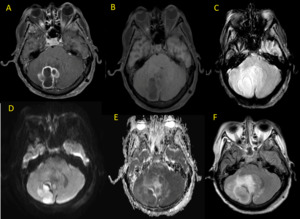
Fig. 18: Multiple abscesses in a 60 year-old man. Axial MR images show ring-enhancing lesions with central restricted diffusion.
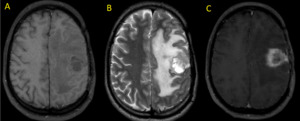
Fig. 19: GBM. Axial MR Images (A) T1 and (B) T2 show a parietal heterogeneous mass with extensive perilesional edema. T1 post-contrast image (C) demonstrates ring enhancement with thick irregular wall and a shaggy inner margin.
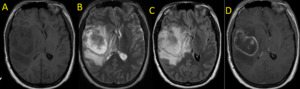
Fig. 20: GBM. Axial MR Images. (A) T1, (B) T2 and (C) FLAIR show a large mass with heterogeneous content and perilesional edema. T1 post-contrast weighted image (D) reveals ring-enhancement with irregular wall.
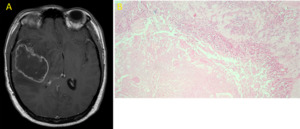
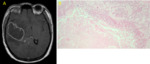
Fig. 21: Glioblastoma. T1 post-contrast MR Image (A) and microscopy (B) show a pseudopalisade sign.

Fig. 6
INFARCT/ISCHEMIA/INFECTION
Infarct
Occasionally there can be ring-enhancement following infarct,
usually in the subacute stage. The enhancement can have a confusing and bizarre appearance,
even mimicking tumors.
Infection- Neurocysticercosis
Neurocysticercosis (NCC) is the most common parasitic disease of the central nervous system,
and also one of the most common causes of seizures in endemic areas (Latin America,
parts of Oceania,
Asia,
Eastern Europe,
and Africa).
NCC is caused by the ingestion of larvae from the adult tapeworm Taenia solium.
Neuroimaging of parenchymal NCC depends on the stage of the development of the parasites.
In the vesicular stage the cysticerci appear as cystic lesions within the brain parenchyma.
CT and MRI reveal that the cyst wall is thin and well demarcated from the parenchyma,
without perilesional edema and do not enhance.
There may be a bright nodule in their interior giving the lesion a “hole with dot” appearance that represents the scolex.
As the cysts begin to degenerate they appear as ill-defined lesions surrounded by edema which enhance after contrast medium administration.
This is the colloidal stage of the cyst and represents the so-called “acute encephalitic phase” of NCC.
MRI reveals a thick and hypointense wall with marked perilesional edema.
Granular cysticerci appear as nodular hyperdense lesions surrounded by edema or a rim of gliosis after contrast medium administration.
Calcified cysticerci appear on CT as small hyperdense nodules without perilesional edema or abnormal enhancement after contrast administration.
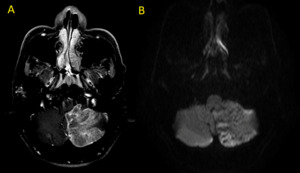
Fig. 25: Patient with posterior fossa infarct. (A) T1 post-contrast and (B) diffusion axial MR images. Note Irregular ring-enhancement in A.
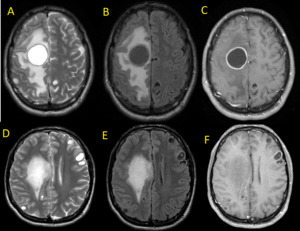
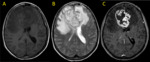
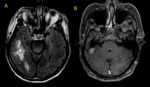
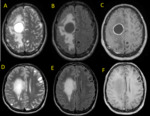
Fig. 35: Neurocysticercosis. Axial MR images (A, D) T2, (B, E) FLAIR and (C, F) T1 post-contrast reveal cystic lesions with ring-enhancement, the largest one with surrounding edema.

Fig. 7
CONTUSION
Both traumatic and nontraumatic intraparenchymal hemorrhage can show ring enhancement in the subacute to chronic stage.
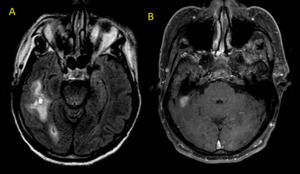
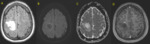
Fig. 26: Patient with a history of head trauma. Axial MR Images (A) FLAIR and (B) post-contrast T1. Oval lesion with ring enhacement is seen on the right. Also note perilesional edema.

Fig. 8
AIDS
Tuberculoma
- CNS tuberculosis is an AIDS defining illness,
and it may be the initial clinical manifestation of this syndrome.
- The most common intracranial manifestation of tuberculosis is meningitis,
however,
tuberculoma and tuberculous abscess are not uncommon findings.
- The majority of tuberculomas are supratentorial and may be solitary or multiple.
- On postcontrast images,
noncaseating tuberculomas demonstrate nodular homogeneous enhancement.
Caseating tuberculomas have ring enhancement.
They are typically less than 1 cm.
- Tuberculous abscesses tend to be larger (usually greater than 3 cm) and are more common in HIV-infected patients.
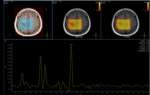
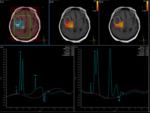
At MR spectroscopy,
they demonstrate prominent lipid and lactate peaks,
but no amino acid peak,
unlike bacterial abscesses
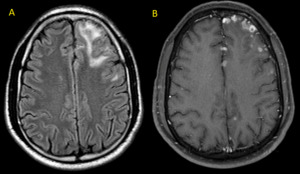
Fig. 27: Tuberculomas. (A) FLAIR and (B) T1 post-contrast axial MR images demonstrate multiple small lesions with ring enhancement. Surrounding edema is seen in A.
Toxoplasmosis
- Cerebral toxoplasmosis is the most common opportunistic CNS infection in AIDS patients,
occurring in 15%–50% of cases.
- These lesions are often multiple,
demonstrate ring or nodular enhancement and appear most frequently in the basal ganglia,
thalamus,
and corticomedullar junction.
- Sometimes a small eccentric nodule is seen alongside an enhancing ring,
the so-called “target sign” which is highly suggestive of toxoplasmosis,
although relatively insensitive and seen in less than 30% of cases.
- At MRI,
toxoplasmosis lesions are typically hypo- to isointense on T2-weighted sequences and are surrounded by high-signal-intensity vasogenic edema
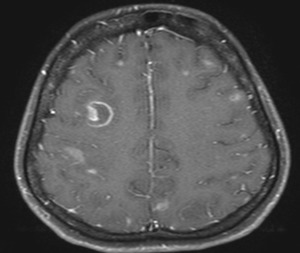
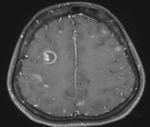
Fig. 28: Neutoxoplasmosis. Axial T1 post-contrast MR image shows ring enhancing lesion with thin well-defined wall. Note the presence of target sign in the larger right frontal lobe lesion. There are small foci of enhancement bilaterally.
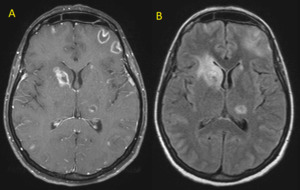
Fig. 29: Neurotoxoplasmosis. Axial T1 post-contrast MR Image (A) and axial FLAIR (B) show the eccentric target sign which is highly suggestive of this infection.

Fig. 9
LYMPHOMA
- Primary CNS lymphoma is the second most common cause of intracranial mass lesions in HIV infected patients and occurs in up to 2.0% of these individuals.
- The lesions of primary CNS lymphoma round or oval masses with homogeneous contrast enhancement and variable surrounding edema.
They are often multifocal and periventricular in location,
rarely invade the basal ganglia and have a tendency to occur in the white matter adjacent to an ependymal surface.
Approximately 50% of the patients with CNS lymphoma may also have multifocal ring-enhancing lesions
- Lymphoma lesions will result in positive findings at SPECT and FDG PET,
and toxoplasmosis will not which helps in the differential diagnosis,
although lymphoma lesions smaller than 2 cm may result in negative findings.
- At MR spectroscopy,
lymphoma demonstrates elevated peaks of choline and MR perfusion typically shows an elevated relative cerebral blood volume which is not seen in toxoplasmosis.
- If a periventricular pattern is present,
this finding suggests lymphoma,
since toxoplasmosis uncommonly involves the ependyma.
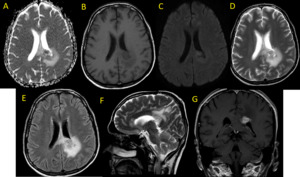
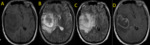
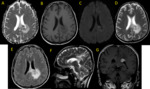
Fig. 30: Primary Lymphoma. Multiplanar MR images (A-G) show ring-enhancing mass with vasogenic edema on the left involving the corpus callosum and crossing the midline.

Fig. 10
DEMYELINATION/MULTIPLE SCLEROSIS
- The most common cause of demyelination is multiple sclerosis.
- The diagnosis of multiple sclerosis includes some demonstration,
by clinical or radiologic means,
that lesions are separated in both space and time.
- Classic multiple sclerosis lesions or plaques present as elongated oval regions of increased water that are oriented perpendicular to the margins of the lateral ventricles (“Dawson’s fingers”).
Multiple sclerosis plaques enhance during the “active phase,” and this enhancement usually lasts for 2–6 weeks.
- The enhancement of multiple sclerosis plaques may be faint,
with a thin and often incomplete rim (“open ring sign”) which is strongly suggestive of demyelination.
The lesions usually do not produce any perilesional vasogenic edema.
- An “incomplete ring” may be seen in active demyelination,
both in multiple sclerosis and in tumefactive demyelination.
If multiple sclerosis is suspected,
MR imaging of the spinal cord may demonstrate additional lesions to help support the diagnosis.
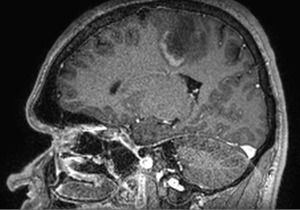
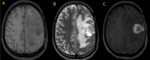
Fig. 31: MR Image shows open ring enhancing lesion compatible with active demyelination.
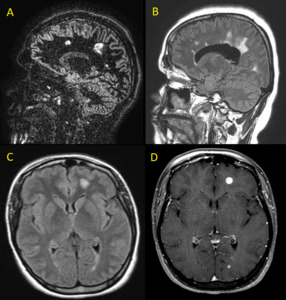
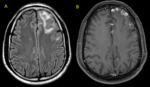
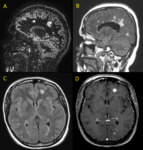
Fig. 32: Multiple hyperintense lesions in a patient with multiple sclerosis. (A) sagittal DIR, (B) sagittal FLAIR, (C) axial FLAIR and (D) axial post-contrast T1. Dawson’s fingers is best seen in sagittal images. Also note enhancement of some of these lesions.

Fig. 11
RESOLVING HEMATOMA
Ring enhancement is frequently observed in resolving intracerebral hematoma.
The proposed mechanisms of the enhancement in this condition include blood-brain barrier breakdown,
vascular granulation tissue,
and luxury perfusion.
SUMMARY AND TAKE HOME MESSAGES
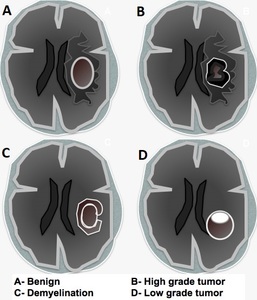
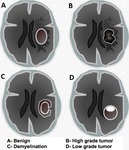
Fig. 37: Schematic drawings. Ring-enhancing lesions.
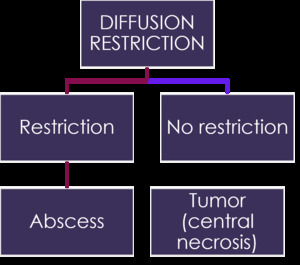
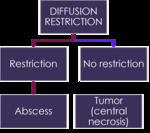
Fig. 15: Summary and take home message. Diffusion.
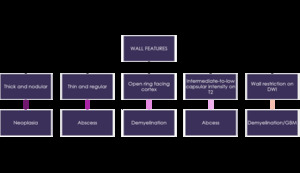
Fig. 16: Summary and take home message.
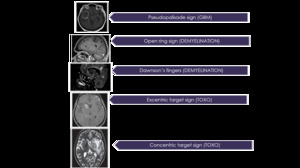
Fig. 17: Summary and take home message. Typical signs.