Keywords:
Breast, Oncology, Mammography, Nuclear medicine conventional, Diagnostic procedure, Cancer, Prospective, Diagnostic or prognostic study, Performed at one institution
Authors:
A. Chernaia1, A. Mishchenko2, S. N. Novikov3, P. Krivorotko3, P. Krzhivitskiy3, R. Ulyanova4, V. Danilov4; 1Saint-Peterburg/RU, 2St. Petersburg/RU, 3St Petersburg/RU, 4Saint-Petersburg/RU
DOI:
10.26044/ecr2020/C-00370
Methods and materials
437 women were examined at N. N. Petrov National Medical Research Center of Oncology; the mean age of the women was 50 years.
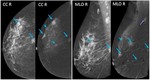
Mammographic digital images were obtained on Senographe DS «GE» unit with a flat panel detector (Se, 100 μm) and image size - 24х31 cm² = 7.4 megapixel. Mammographic examination was performed with breast compression and included routine craniocaudal (CC) and mediolateral oblique (MLO) views of the breasts. An IV injection of 1.5 mL/kg body weight of a non-ionic contrast medium (Iohexol 350) was carried out using an injector with an injection rate of 3 mL/s. After a 2-minute delay, the mammography technologist positioned the patient and compressed the breast as for a mammography examination in CC and MLO view. For each breast, the CC view of breast with suspicious lesion was collected first, then CC view of second breast, followed by the MLO view of breast with suspicious lesion, after that MLO view of second breast. 2 images (a low-energy acquisition and a high-energy acquisition) in each view orientation were automatically collected in the CESM mode (Fig. 1., Fig. 3.).
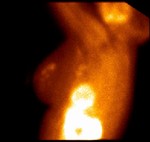
Breast imaging with 99mTc-MIBI was performed with dual detector SPECT unit «Forte» (Philips) with low energy, all purpose collimation. Images of both breasts were obtained 10-15 min after injection of 740 MBq of 99mTc-MIBI into a footstep vein. Planar scintigraphic images were acquired in anterior (supine) and lateral (prone) positions with a lead shield placed between two mammary glands. Images were acquired 10 min after the tracer injection into 256x256 matrix with 600 sec exposition of each projection and breast “in touch” with detector. Special attention was paid to standardization of basic acquisition parameters: injected activity, time after injection, exposition time and distance between a breast and a detector (Fig. 2., Fig. 4.).
In all cases, histopathology was taken as the gold standard.