CEUS LR-M Criteria

Fig. 3: CEUS-LI-RADS M Criteria
References: CEUS LI-RADS v2017 CORE

Fig. 4: Washout degree and onset
References: CEUS LI-RADS v2017 CORE
Example: Fig. 5
CEUS Ancillary Imaging Features

Fig. 6: CEUS LI-RADS.Ancillary Imaging Features
References: CEUS LI-RADS v2017 CORE
CT-MR LR-M Criteria

Fig. 7: CT-MR LI-RADS M Criteria
References: CT/MRI LI-RADS v2018 CORE
Examples: Fig. 8, Fig. 9, Fig. 10, Fig. 11
CT-MRI Ancillary Imaging Features

Fig. 12: CT-MRI LI-RADS
Ancillary Imaging Features favoring malignancy not HCC in particular
References: CT/MRI LI-RADS v2018 CORE

Fig. 13: CT-MRI LI-RADS
Ancillary Imaging Features favoring malignancy HCC in particular
References: CT/MRI LI-RADS v2018 CORE
The next algorithm suggests a probable etiology based on radiological findings.

Fig. 14: CT/MRI LI-RADS M Algorithm
References: CT/MRI LI-RADS v2018 CORE
The differential diagnosis includes; atypical HCC, iCCA, cHCC-CCA, and less common, primary tumor, metastases, and benign entities.

Fig. 15: LI-RADS M
% Malignancies
References: CT/MRI LI-RADS v2018 CORE

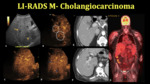
Fig. 16: LI-RADS M examples
References: Department of Radiology UC San Diego
Intrahepatic CCA
CCA is the most common biliary tract malignancy and the second most common primary hepatic tumor after HCC.
Among numerous risk factors described for iCCA, many are similar to those reported for HCC. The majority develops sporadically.
Has been categorized for the anatomic location: extrahepatic, peripheral intrahepatic (20%) and hilar intrahepatic (50–60%) and morphologic: intrahepatic mass-forming, periductal infiltrating and intraductal growth types.
CT-MRI show the arterial phase not only to distinguish from HCC but also helps more clearly to delineate the vascular anatomy prior to surgical resection. The delayed phase accentuates the presence of fibrous stroma, which is a distinguishing feature of CCAs.Fig. 17
May be FDG avid on PET. Mucinous variants may show little FDG uptake. Periductal may be difficult to diagnose when there is background inflammation and-or stents.
Liver transplantation is not done for these lesions except under investigational protocols, because of high post-transplant recurrence risk.
Combined HCC-CCA
They are the third most common primary liver cancer in cirrhosis.They are malignancies composed of cells with both cholangiocellular and hepatocelluar differentiation.
Emerging reports suggest they resemble iCCAs in appearance although they may exhibit hepatocellular features such as intralesional fat or blood products.Fig. 19
Conservatively, these tumors are assumed to have poor prognosis and biology, similar to iCCA.
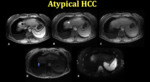
Atypical HCC
Approximately 40% of HCCs do not demonstrate the classic imaging findings, resulting in decreased accuracy of imaging tests for the diagnosis of HCC.
Types: Non-Hypervascular(Fig. 20), targetoid(Fig.21), fibrolamellar, infiltrative(Fig. 22), and intraductal growing.
Other examples: Fig. 23, Fig. 24
Sarcomatoid Carcinoma (SC)
Malignant tumor type of unclear pathogenesis.SC rarely occurs in the liver, and has been detected in only 1.8% of all surgically resected HCCs, and in 3.9-9.4% of autopsied cases, accounting for only 0.2 % in the primary malignant liver tumors.
On contrast-enhanced MRI, the tumors show irregular annular enhancement in the arterial phase and central "honeycomb" heterogeneous enhancement in the delayed phase, which could be considered as a specific imaging feature of hepatic sarcomatoid carcinoma. Ischemia and necrosis of intratumoral tissues are low-signal areas within honeycombs, and the solid components of tumors are "grids" of honeycombs in the delayed phase. There are fibrous stromal components in the tissue contrast media stay and flow out slowly, so it is delayed enhancement. SC has a worse prognosis than HCC or iCCA.Fig. 25
Others malignancies
Primary hepatic lymphoma (PHL)
PHL represents less than 10% of space occupying focal hepatic lesions. Among lymphoma, PHLs represent 0.4% of all extranodal lymphomas and 0.016% of all non-Hodgkin lymphomas.
PHL is commonly associated with viral hepatitis B and C and Epstein-Barr virus, but the pathophysiology of PHL is poorly understood.
Has been categorized according to the anatomic location and morphology: discrete focal liver mass or masses, diffuse infiltrating disease and ill-defined mass in the porta hepatis.Solitary discrete lesion is the most common presentation (60%), multiple lesions (35%–40%) or diffuse infiltration (uncommon)
CT and MRI show lymphomatous nodules commonly have soft-tissue attenuation but enhance to a lesser degree than the liver parenchyma on arterial, portal venous, and delayed phase images. DWI may allow earlier identification of disease. FDG PET-CT for lymphoma staging demonstrates avid hypermetabolism and is the imaging modality of choice for staging and for assessing treatment response.
Angiosarcoma
Hepatic angiosarcoma accounts for 0.1%-2% of all primary hepatic malignancies.
US: multiple nodules or solitary mass with varying echogenicity from necrosis and hemorrhage.
CT: hypodense with multiple patterns of enhancement and postcontrast; the lesions become partly or completely isodense in comparison with the hepatic tissue. MRI can also be used to identify hepatic angiosarcoma as it can reflect the hemorrhagic, heterogeneous, and hypervascular nature of the lesions.
Has an aggressive clinical course, and the prognosis is poor in inoperable cases.Complete hepatic resection or radical resection of the tumor is the most effective form of treatment for single lesions; however, it is not always feasible in metastatic disease.Fig. 26
Metastases
In general, metastases are the most common malignant liver lesions and are about 18-40 times more common than primary liver tumor in non-cirrhotic livers. Metastases are less common in cirrhosis, potentially due to altered hepatic-portal flow and background liver milieu.
Most common primaries that metastasize to the liver:

Fig. 27: Most common liver metastases
References: Department of Radiology UC San Diego
Among carcinomas, adenocarcinoma comprises 70%, and squamous cell carcinoma follows.Fig. 28
Metastases are categorized as LI-RADS M, and the biopsy will be a tool to find the etiology.
Several types of liver metastases are known to have avid FDG uptake and thus FDG-PET has a good detection rate for liver metastases. On a per patient basis, PET-CT shows good performance for detection of liver metastatic disease (is 90-94.6%).PET-CT is indicating for the search the primary tumor, and to stage tumors prior to curative-intent surgery. Fig. 29
Benign lesions

Fig. 30: Benign LI-RADS M
References: Department of Radiology UC San Diego
Sclerosing hemangioma(SH)
SH is an unusual tumor type, for the atypical radiologic findings can be difficult to distinguish from other lesions.
Hemangioma degeneration can occur by an increasing degree of fibrosis and thrombosis of its vascular channels. The process of sclerosis changes the radiologic characteristics of hemangiomas.
Mild to moderate hyperintensity on T2 (typically less than classic hemangioma), hypointensity on T1, patchy enhancement during the arterial phase, and gradual progressive enhancement during the portal and delayed phases except in the central area. Due to fibrosis, there is often capsular retraction. FDG-PET show iso to hypometabolism.Fig. 31
Abscess
Tumors with extensive necrosis may mimic hepatic abscesses, however, the pattern of wall enhancement and signal intensity in tumors does not show the typical “target” appearance; the internal surface of the wall may also be more nodular in necrotic neoplasms. Transient early circumferential or wedge-shaped segmental regions of hepatic hyperenhancement and/or perilesional edema are often associated with abscesses.Fig. 32
Abscesses generally show hyperintensity on DWI images with high b values and hypointensity on ADC maps, in contrast to the cystic or necrotic portion of tumors, but there may be overlap.
Differentiation may not be possible and aspiration/biopsy must be performed.