Introduction
Acute mesenteric ischemia AMI is a catastrophic abdominal emergency characterized by a sudden interruption of intestinal blood flow, which leads to ischemia, intestinal necrosis and eventually death.
Etiologies of AMI include a arterial occlusion from a variety of underlying causes, venous occlusion, and nonocclusive arterial processes. The causes of AMI are further classified as MAE, MAT, MVT and NOMI. Fig 1
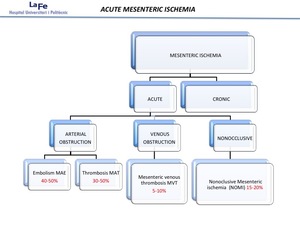
Fig. 1: Causes of vascular insuffiency.
Normal Anatomy
The superior mesenteric artery supplies the third and fourth portions of the duodenum, jejunum, ileum and colon to the level of the splenic flexure.
There are numerous mesenteric collateral pathways like the marginal artery of Drummond and the arc of Riolan .
( FIG 2)
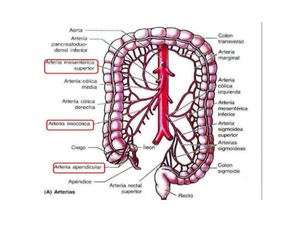
Fig. 2
References: https://image.slidesharecdn.com/anatomiadeestomagoeintestinos-110303131601-phpapp01/95/anatomia-de-estomago-e-intestinos-34-728.jpg?cb=1299158224
The venous system returns essentially parallel to the arterial supply. The superior and inferior mesenteric veins run parallel to the arteries and drain the respective part of the bowel. ( Fig 3)
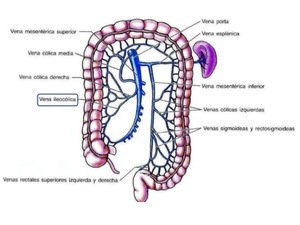
Fig. 3
References: https://image.slidesharecdn.com/anatomiadeestomagoeintestinos-110303131601-phpapp01/95/anatomia-de-estomago-e-intestinos-36-728.jpg?cb=1299158224
Pathophysiology of Intestinal Ischemia
Although a 75% reduction in blood flow can be tolerated for up to 12 hours, complete vascular occlusion will progress to irreversible intestinal infarction if untreated within 6 hours.
Intestinal ischemia progresses through three stages.
Only the mucosa is affected in the first stage, resulting in increased mucosal permeability to macromolecules.
Complete resolution is possible, however, if the ischemia is reversed at this stage. The first stage is called reversible ischemic enteritis.
The second stage involves progressive necrosis of the underlying submucosal and muscular layers. Deeper necrosis is likely to cause luminal dilation due to either reactive interruption of peristalsis or direct muscular involvement. If the ischemia is reversed at this stage, a fibrotic stricture is likely to develop.
Complete transmural bowel wall necrosis indicates the third and final stage. Perforation is also indicative of transmural involvement while pneumatosis and portal venous gas suggest an advanced stage of infarction of either partial or full wall thickness. After that, the mucosal barrier breaks down leading to bacteraemia and sepsis
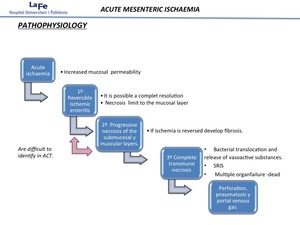
Fig. 4: Pathophysiology of intestinal ischemia









