DIAGNOSTICO IMAGING
MDCT PROTOCOL
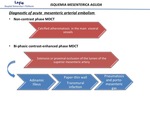
Different diagnostic techniques can be performed, but the technique of choice is abdominal CT angiography.
Abdominal radiography has historically been considered the first imaging modality (1B), to assess abdominal pain.

Fig. 5: American College of Radiology . ACR Appropiateness criteria Imaging of AMI
References: ACR Appropiateness Criteria
ANGIO-CT ABDOMINAL (1A)
It is the technique of choice and should be the first to be performed if MAI is suspected.
CTA is recommended by at American College of Radiology ( ACR) appropiates criteria for rapid, non-invasive and it has high sensitivity and specificity.

Fig. 6: CT protocol
MDCT IMAGING FINDING OF AMI.
The MDCT gives us double information, first of all the radiological findings that cause vascular ischemia and the intestinal findings secondary to vascular damage. And secondly it gives us a prognostic approach, which suggests extensive necrosis and complications.
1. Vascular imaging findings.
Intraluminal defects or occlusion of mesenteric vessels. It has a high specificity and a relatively low sensitivity.
· Occlusive forms.
The MDCT makes it possible to locate the proximal vascular fillings defects, more easily than the distal ones, for which the realization of multiplanar reconstructions is very helpful.

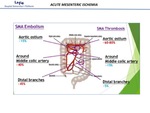
Fig. 7: Most frequent locations of stenosis according to etiology.
- Arterial embolism:
Cut-off sign: abrupt termination of the vessel
Ring sign: non-occlusive emboli.
Presence of small distal emboli.
Association with emboli attacks in other organs.
- Arterial thrombosis: Atheroma calcified or non-calcified plaques at the origin of the AMS.
It is more proximal than the embolism, seen in the firts centimetres of the artery.
- Arterial dissection: Linear intraluminal defect, which represents the intimal flap.
More frequent in association with aortic dissection, rare isolated.
- Venous thrombosis: Low density filling defect in enhancement-contrast CT
If it is acute: Increase the diameter of the vessel.
If it is chronic: narrowing of the vessel.
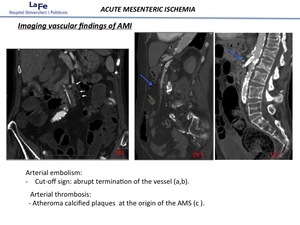
Fig. 8: Vascular imaging findings
· Non-occlusive forms:
They are based on low flow and vasocontriction
NOMI: narrowing of the vessels
Inferior cava flattening
irregularities in the AMS and poor visualization of bowel arches.
2. Bowel imaging findings.
They can be difficult to interpret, and there is some inter-observer variability.
- Thickening of the wall: It is the most frequent finding, but it is nonspecific, it has high sensitivity . It is due to mural edema .
It is most striking in venous thrombosis due to venous stasis and hemorrhage. It is associated with target appearance.
- Thinning of the bowel wall
In cases of arterial ischemia, the intestinal wall has a paper-thin appearance. It is due to the loss of volume of tissue and vessels in advanced ischemia.
- Bowell wall hyperattenuationon unenhanced MDCT:
This sign has an excellent specificy and lower sensitivity. Its result to submucosal hemorrhage, either due to arterial repercussion after AMI or increased pressure due to venous occlusion.
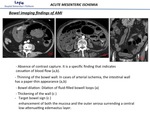
- Absence of contrast capture. It is a specific finding that indicates cessation of blood flow.
- Target bowel sign.
- Bowel dilation: is caused by a reflex interruption of intestinal peristalsis or exudation in the intestinal lumen. It is more frequent in arterial occlusion

Fig. 9: Bowel imaging findings
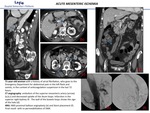
- Intestinal pneumatosis and portal venous gas: presence of air bubbles in the bowell wall (bubble-like) or air rings that dissect the wall in two layers (band-like), up to the portal. Its sign of necrosis, very specific.
- Mesenteric fat stranding and ascites
Transudation of fluid is produced to the mesentery and the peritoneal cavity due to increased venous pressure and infection of ischemic bowel.
It is one of the most sensitive sign of AMI.
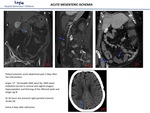
- Involvement of the others organs. infarts due to emboli, most often spleen or kidneys.

Fig. 10: Bowel imaging findings
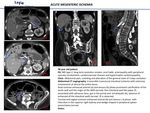
MESENTERIC ARTERIAL EMBOLISM (MAE).
The embolism is the most frequent cause of AMI (40-50%).

Fig. 24
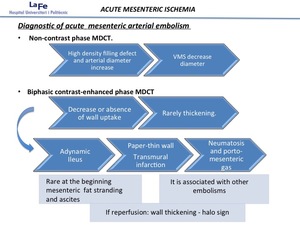
Fig. 11
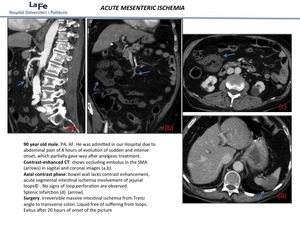
Fig. 12: Mesenteric arterial embolism

Fig. 13: Mesenteric arterial embolism
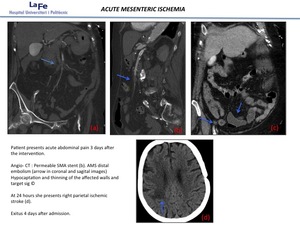
Fig. 14
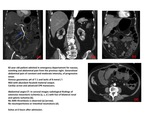
MESENTERIC ARTERAL THROMBOSIS.
Thrombosis usually occurs at the origin of visceral arteries, moreover, an underlying plaque in the SMA usually progresses to a critical stenosis over years resulting in collateral beds.

Fig. 25

Fig. 16: Mesenteric arterial thrombosis

Fig. 17
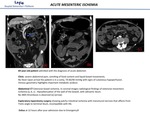
MESENTERIC VENOUS THROMBOSIS.
Mesenteric venous thrombosis (MVT) accounts for less than 10% of cases of mesenteric infarction .

Fig. 26
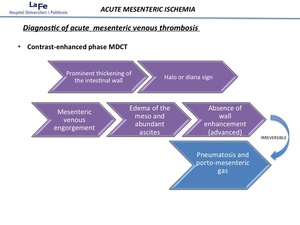
Fig. 18

Fig. 19: Mesenteric venous thrombosis
NONOCLUSIVE MESENTERIC ISCHEMIA.

Fig. 27

Fig. 20
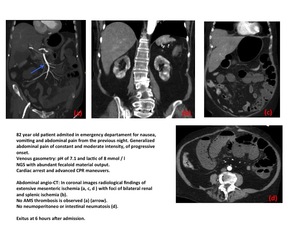
Fig. 21: Nonoclusive mesenteric ichemia

Fig. 22: Nonocclusive mesneteric ischemia
PRONOSTIC VALUE OF CT
Any delay of the initial diagnosis and intestinal revascularization
plays a critical role according to the prognostic parameters.
The lethality of AMI rises exponentially from 10 to 100%
within 24 h.

Fig. 23
TREATMENT OF AMI
Management of AMI has historically included surgical restoration of mesenteric blood flow and resection of the necrotic bowel. However, in cases without irreversible bowel damage from ischemia, EVT may reduce the need for open surgery.

Fig. 28

Fig. 29