Purpose
Describe the contribution of CT and MR imaging in the diagnosis of tuberculous sacroiliitis as well as post-treatment follow-up.
Methods and materials
We performed a retrospective, descriptive study of patients hospitalized in universtity hospital «Hedi Chaker», Sfax, tunisia, between 2007 and 2019. We included all patients presenting with tuberculous monoarthritis of the native sacro-iliac joint.
We collected the following Data:
·Age, gender, antecedents (familial tuberculosis story, be treated for pulmonary tuberculosis or other…)
·Initial clinical presentation.
·Fever.
·Diagnostic delay.
Biological parameters such as ESR, tuberculosis skin test and Quantiferon-TB-Gold test were collected.
We also collected the following microbiological Data : Tubercle Bacilli isolated from high quality samples...
Results
12 cases of tuberculous sacro-iliitis (34,3 %), from 35 infectious sacro-iliitis, were identified in adults, including 8 (67%) women and 4 (33%) men (Figure 1).
The average age of diagnosis was 53 ± 17 years.
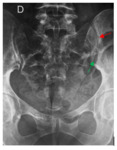
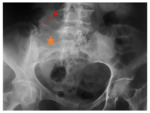
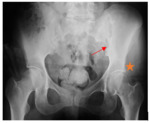
The sacro-iliitis was unilateral in 11 (91,7 %) cases, the right joint was effected in 5 cases and the left joint in 6 cases. It was bilateral in one case (8,3 %).
One patient was treated for lymph nodes tuberculosis, another was treated for pericardial tuberculosis.
Low back pain, fever...
Conclusion
Tuberculosis remains one of the most common infectious diseases in the world (1).
Musculoskeletal involvement with tuberculosis is uncommon, representing approximately 1 – 3% of cases (2). Sacroiliac joint involvement had been reported in 9.7% to 14 % of patients with skeletal tuberculosis (1–3). It represents 5 to 57% of infectious sacroiliitis (4).
Tuberculous sacroiliitis is responsible for inconspicuous symptoms (1), because of anatomy particularities of this articulation.
Sacroiliac involvement is usually unilateral, but bilateral involvement is possible, found in 6% of cases (4).
The...
Personal information and conflict of interest
A. Kammoun; Sfax/TN - nothing to disclose W. Feki; Sfax/TN - nothing to disclose H. Fourati; Sfax/TN - nothing to disclose E. Daoud; Sfax/TN - nothing to disclose Z. Mnif; Sfax/TN - nothing to disclose
References
1. Benchakroun M, El Bardouni A, Zaddoug O, Kharmaz M, Lamrani MO, El Yaacoubi M, et al. Tuberculous sacroiliitis. Four cases. Joint Bone Spine. avr 2004;71(2):150‑3.
2. Gao F, Kong X-H, Tong X-Y, Xie D-H, Li Y-G, Guo J-J, et al. Tuberculous Sacroiliitis: A Study of the Diagnosis, Therapy and Medium-Term Results of 15 Cases. J Int Med Res. févr 2011;39(1):321‑35.
3. Pertuiset É. Tuberculose ostéoarticulaire extravertébrale. Revue du Rhumatisme. avr 2006;73(4):387‑93.
4. Bouajina E, Harzallah L, Hachfi W, Slama KBH, Rammeh N, Ghannouchi M,...