Purpose
To assess by ultrasound (US) cardiovascular disease (CVD) in patients with different types of hypoxia, studying the volume of atheromatous plaques and intima-media thickness (IMT) in femoral and carotid arteries.
Methods and materials
We conducted a prospective study including 223 patients who visited the sleep and chronic obstructive pulmonay disease (COPD) consultation between May and June 2017.
These patients were divided among COPD as a model of continuous hypoxia, obstructive sleep apnea (OSA) as intermittent hypoxia, combination of both as overlap syndrome (OS) and healthy controls.
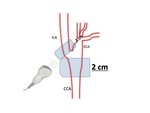
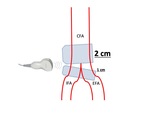
All of them underwent sleep study and spirometry with bronchodilator test. Then we performed US,looking for atheromatous plaques and measuring the IMT. For this purpose, we employed a 7 MHz probe.
The...
Results
223 patients who visited the sleep and COPD consultation between May and June 2017 were included.
COPD= 38 (17%)
OSA = 114 (51%)
controls = 32 (14%)
OS = 38 (17%)
Cardiovascular and metabolic comorbidities were studied:
COPD and OS had significantly higher pack-year index (p
Conclusion
Atheromatous plaques aremore prevalent and in more territories in COPD and OS.
GIM is not different among different types of hypoxia. A bigger sample might be needed.
COPD and OS present more atrial fibrillation, heart failure and TC90.
US is a useful tool characterizing CVD in patients with intermittent or continuous hypoxia. A further analysis with 3D reconstruction of the plaques mightprovide some new information.
Personal information and conflict of interest
J. M. Muñoz Olmedo; Madrid/ES - nothing to disclose J. Tejelo Labrador; Madrid/ES - nothing to disclose A. Friera; Madrid/ES - nothing to disclose P. Rodriguez Carnero; Madrid/ES - nothing to disclose
References
1. Touboul PJ, Hennerici MG, Meairs S, Adams H, Amarenco P, Desvarieux M, et al. Mannheim intima-media thickness consensus. In: Cerebrovascular Diseases. 2004.
1. Touboul PJ, Hennerici MG, Meairs S, Adams H, Amarenco P, Desvarieux M, et al. Mannheim intima-media thickness consensus. In: Cerebrovascular Diseases. 2004.