Intracranial TB is becoming more sophisticated and atypical due to multi-drug resistance.
MRI Protocol
Any MRI of patients suspected of intracranial tuberculosis should include axial precontrast T1W,T2W,FLAIR,diffusion-weighted images sequence(DWI) GRE/SWI and postcontrast T1W scans in all three plans.Magnetic resonance angiography(MRA) and magnetic resonance venography(MRV) may be added in patients with suspected vascular complications.
The Spectrum of Intracranial TB
A-MENINGEAL
1-Leptomeningeal
2-Pachymeningitis
B-PARENCHYMAL TUBERCULOSIS
1-Tuberculoma
2-Cerebritis
3-Abscess
4-Rhombencephalitis
5-Encephalopathy
A-MENINGEAL TUBERCULOSIS
1-Tubercular Leptomeningitis
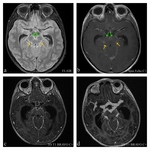
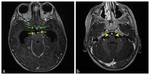
Tuberculous meningitis(TBM) is the most common manifestation of CNS TB and occurs frequently in children and adolescents.TBM strikingly gives findings in basal cisterns which are generally in interpeduncular fossa, suprasellar, ambient and perimesencephalic cisterns.Fig. 2 Less frequently may spread over the cerebral convexity,the tentorium,Sylvian fissure, along cerebellar meninges and choroid plexus.
Computed Tomography(CT) scans may be normal in the earliest stages of TBM.MRI is more sensitive than CT to show findings.Exudates can be recognized by increased FLAIR signal intensity or enhancement.Pre-contrast and post-contrast magnetization transfer(MT) imaging is superior to conventional spin-echo sequences in demonstrating meningeal inflammation.MT ratio (MTR) quantification helps to differentiate TB from nontuberculous meningeal inflammation.A low MTR indicates TBM[5].
The probable complications of meningitis are hydrocephalus,vasculitis, infarction, and cranial neuropathies.
- Hydrocephalus,which is the most common complication of CNS TB can be communicating or non-communicating type.Fig. 3
·Communicating hydrocephalus is more frequent and occurs as a result of obstruction to cerebrospinal fluid(CSF) flow in the basal cisterns by the exudates.
·Nonspecific hydrocephalus is the most common finding of TBM on non-enhanced computed tomography(NECT).
·Periventricular hyperintensity on T2W or FLAIR images indicates CSF leakage to white matter.
·Rupture of Rich focus or spread of infection into the ventricles results in ventriculitis.Venriculitis is seen on MRI with diffusion restriction and increased signal intensity of CSF on T1W and FLAIR images.Fig. 4
- Vascular complications are seen in 15-67% of cases.
·Stroke is associated with poor prognosis in patients with TBM.
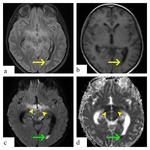
·Exudate spreads along the cisterns from the base of the brain and it covers the large arteries and their small perforators.For that reason, the middle cerebral artery and its perforators around the third ventricle are most frequently involved so thalamus and basal ganglia are the most common site of infarcts.Fig. 5
·Hemorrhagic transformation can be seen as in every stroke.Fig. 6
·Especially in children,the coexistence of infection and infarction should not only suggest tuberculosis, but herpes zoster should also be kept in mind.Fig. 7
·Infarcts can be detected early by using DWI.Three-dimensional time of flight(TOF) MR angiography reveals signal loss or narrowing within vascular structures.
·TBM can also lead to dural venous sinus thrombosis which can result in hemorrhagic infarction.
- Cranial nerve (CN) involvement occurs in 17-40% of cases.
·The most commonly affected cranial nerves are CNII,CNIII,CNIV, and CNVI.
·The affected nerve seems thickened and shows prominent contrast enhancement.Fig. 8
2-Tubercular Pachymeningitis
Tubercular pachymeningitis,which is the TB infection of the dura mater,is less common than tubercular leptomeningitis.Pachymeningitis may be focal or diffuse.On MRI,thickened dura mater and contrast enhancement of dura are seen.These findings aren’t specific for TB.
B-PARENCHYMAL TUBERCULOSIS
1-TUBERCULOMA
·Tuberculomas are the most frequent form of intracranial parenchymal TB.
·They are more common in children and mostly infratentorial.In adults, tuberculomas are predominantly supratentorial.
·Tuberculoma may be seen anywhere within the brain and commonly located at the corticomedullary junction.
·Tuberculoma may present without meningitis or meningeal involvement and may be seen in the form of solitary or multiple.
·Depending on the stage tuberculomas may have a variable appearance on MRI.Table 1 Fig. 9 Fig. 10
·Paradoxical reaction,that is, delayed development or worsening of brain lesions,can occur a few months after the start of TB treatments,in patients who show improvement after the first treatment.They may resolve completely but in most cases,they resolve with calcified granulomas.
2-Tubercular Abscess
·Tubercular abscess is not a common pattern of presentation and occurring less than 10% of cases.
·It is more common in elderly and immunocompromised patients.
·Contents of the abscess are hypointense on T1W and heterogenous-hyperintense on T2W.DWI generally shows diffusion restriction.
·Tubercular abscess shows peripheral enhancement.The abscess wall is usually hypointense on T2W.
·Tubercular abscess may be indistinguishable from caseating tuberculomas with liquefaction. >3 cm size,a thin smooth wall,the presence of restricted diffusion and multiloculation support abscess,but it isn’t certain.
·MR spectroscopy may help to differentiate tuberculous abscess from a pyogenic abscess.Pyogenic abscess demonstrates an amino acid peak at 0,9 ppm,which is absent in TB abscess.
3-Tuberculous Rhombencephalitis
·Tuberculous rhombencephalitis is an uncommon form of intracranial TB
·Patients usually present with focal neurological deficits of cranial nerve palsies or cerebellar symptoms
·It is generally associated with leptomeningitis involving the basal cisterns.
·It is usually visualized as tuberculoma and inflammatory edema( T2W/FLAIR hyperintensity) that involve the brainstem.Fig. 11
4-Tuberculous Encephalopathy
·Tuberculous encephalopathy occurs especially in infants and children with onset of seizures, stupor, and coma without signs of meningitis.
·This entity is thought to be the result of a type 4 hypersensitivity reaction to the tubercular protein
·On MRI,diffuse brain edema which is bilateral or unilateral and contrast enhancement of the involved white matter may be seen
5-Tubercular Cerebritis
·Cerebritis is defined as the involvement of a focal area of brain parenchyma in the infective process.
·T1 hypointensity,T2 hyperintensity and patchy contrast enhancement indicate cerebritis.Fig. 12