Imaging modalities and protocols
Ultrasound is the primary imaging modality for the diagnosis of scrotal pathologies. MRI is also useful for differentiating benign and malignant lesions. The main focus of this article is ultrasound, and we have elaborated with other imaging modalities, wherever needed.
Scrotal Ultrasound technique
Scrotal ultrasound is usually performed with a straight high-frequency probe. Color Doppler imaging can provide a good overview of vascularity, but it has some limitations.
Intra-testicular scrotal pathologies
Epididymo-orchitis
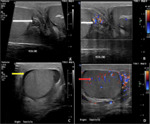
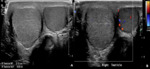
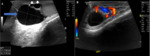
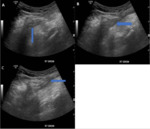
It is the swelling of epididymis and testes. On ultrasound, the epididymis appears enlarged and hypoechoic. It may appear hyperechoic in case of hemorrhage. In 20- 40% cases, it involves the testes due to local spread, and it might give the heterogeneous hypoechoic appearance of the testicle. It is usually associated with minimal hydrocele that generally resolves after the treatment. Color Doppler study depicts hyperemia of epididymis and testes if involved. (Fig. 1)
Testicular abscess
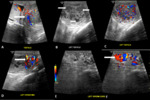
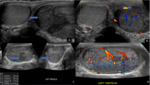
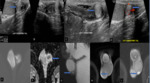
A testicular abscess is a complication of severe or untreated epididymo-orchitis. On ultrasound, the affected side usually shows increased scrotal wall thickness, large testes with intratesticular lesion having shaggy irregular walls. The lesions are variable from hypoechoic to isoechoic with a focal region of avascularity surrounded by increased blood flow on Doppler ultrasound. (Fig. 2)
Tuberculous epididymo-orchitis
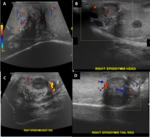
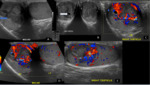
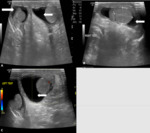
Tuberculous epididymo-orchitis can mimic tumors or bacterial infection. Ultrasound shows diffusely enlarged homogenously hypoechoic, diffusely enlarged heterogeneous hypoechoic, and nodular enlarged heterogeneously hypoechoic epididymis and testis. Scrotal skin thickness and sinus tract formation are the other features suggestive of tuberculosis. (Fig. 3)
Testicular trauma/rupture
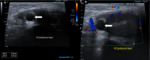
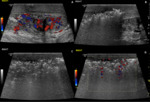
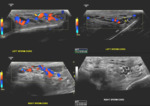
In testicular rupture, ultrasound shows a defect in the tunica albuginea, abnormal contour, a heterogenous echotexture of the testes with irregular, poorly defined borders. It may also represent scrotal wall thickening and a large hematocele. A hematocele is a blood collection within tunica vaginalis, and its echotexture varies with time. The presence of associated hyperechoic or hypoechoic changes in the testicular parenchyma usually suggests testicular rupture. Also, an extra-testicular hematoma can present with the trauma, and its echotexture also varies with time. It often gives avascularity on color Doppler study. (Fig. 4).
Testicular torsion
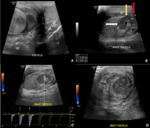
Testicular torsion is the rotation of a testicle along the longitudinal axis of the spermatic cord. The presence or absence of identifiable intratesticular color flow is the only criteria for the diagnosis. The greyscale Ultrasound is non-specific and mostly appears normal during the early hours. During the later hours, it may depict the heterogeneous echotexture and bulky size of the affected testicle. However, the presence of normal echotexture is strongly suggestive of the viability of the testis (Fig. 5).
Testicular tumors
The presence of intratesticular mass lesions is considered malignant, and ultrasound is the modality of choice. Ultrasound usually shows hypoechoic lesion, sometimes with cystic and calcified foci. Mostly, the testicular tumors show increased intralesional vascularity on the Doppler study. MRI is used for local staging (when local penetration of the tumors is inconclusive on ultrasound), characterizing, and differentiating various types of tumors. (Fig. 6 & 7).
Extra-testicular scrotal pathologies
Epididymal cyst and spermatocele
Epididymal cysts can occur anywhere within epididymis, while spermatocele occurs in the head. Greyscale ultrasound shows an anechoic lesion in both conditions with posterior acoustic enhancement. However, spermatocele shows internal echoes due to the presence of spermatozoa. (Fig. 8 & 9).
Epididymal Adenomatoid
Adenomatoid tumors are the most common benign extratesticular tumors and most frequently occur in the epididymis. It occurs more often in the lower pole. There is no evidence of malignant transformation. Ultrasound is the modality of choice, and it shows variable echogenicity and vascularity. MRI is helpful when ultrasound is non-conclusive and cannot differentiate the testicular and extratesticular origin (Fig. 10).
Hydrocele
A hydrocele is a collection of clear fluid around the testicle between the layers of tunica vaginalis. Ultrasound shows anechoic fluid around the testicles. It may have scattered echoes because of cholesterol or calculi. They usually increase in size on straining or Valsalva maneuver. Intraperitoneal contents can also herniate through the process vaginalis (Fig. 11).
Fournier gangrene
Fournier gangrene is polymicrobial necrotizing fasciitis that usually involves perineum and anterior lower abdominal wall. It is a urological emergency due to the high mortality rate. The hallmark of the diagnosis is the presence of subcutaneous gas in the scrotal wall and scrotal wall thickening. The gas appears as discrete hyperechoic foci with reverberation artifacts. (Fig. 12).
Indirect inguinoscrotal hernia
It is an abnormal protrusion of abdominal contents through the patent process vaginalis, crossing the deep inguinal ring into the inguinal canal. Mesentery, peritoneal fluid, small bowel, and mobile large bowel segments are the usual contents of the hernia. (Fig. 13).
Varicocele
It is tortuous dilatation of the pampiniform plexus that drains the testes. Ultrasound shows multiple serpiginous dilated tubular dilated structures of variable sizes, larger than 2mm, and best visualized on the superior and lateral aspect of the testes. It shows increased size on straining or Valsalva. Doppler ultrasound can classify the varicocele into various grades. (Fig. 14).