The prevalence of CAA is not high (1-2%), but early diagnosis and adequate clinical management are important, therefore it is necessary to rule out CAA in young athletes with symptoms (such as syncope, chest pain, arrhythmia). It is useful in this group of patients to find a "non-invasive" screening tool that replaces traditional coronary angiography.
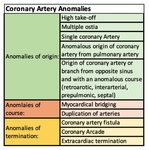
There are different systematic classifications of CAA based on their anatomical features as indicated by Kim. et al., modified from Greenberg classification: [Table 1] anomalies of origin, course and termination.
CAA can be also classified on their potential to induce myocardial ischemia (greater and lesser capacity or benign and malignant) [1-2].
CAA most likely to induce myocardial ischemia are:
- the anomalous origin of the right or left coronary artery (AORCA or AOLCA, fig. 2) from the contralateral aortic sinus with an inter-arterial course [Fig 4-6]
- the coronary artery fistula
- the anomalous origin of a coronary artery from the pulmonary artery (ALCAPA and ARCAPA)
- the single coronary
Minor CAA (benign) are those that usually do not cause myocardial ischemia:
The clinical significance and risk of a CAA generally depend on the type of coronary origin and the course, and also on the degree and location of the stenosis or responsible atherosclerotic lesion [Fig. 3].
In young people the consequences mainly occur during or immediately after exercise, potentially because of the dilation of the aortic root and pulmonary trunk causing coronary compression ab extrinseco, stretching and increasing the pre-existing tangential angle, with a reduction in the lumen of the vessel, sometimes even critical or lethal.
In middle-aged people the anomaly becomes slatent and becomes symptomatic when the arterial trunks become ectatic, rigid or tortuous [3].
Imaging methods for the visualization and evaluation of coronaries
Invasive coronary angiography (ICA)
ICA has been the gold standard for the study of coronary arteries for over 40 years, with excellent sensitivity in demonstrating the origin and course of coronary arteries. This imaging technique has limitations due to its two-dimensional view, invasiveness and cost. It has been reported that among patients with CAA evaluated with 16-layer Multilayer Computed Tomography and with ICA, the latter allowed the correct identification of the anomalies only in 53% of cases. [4]. In consideration of the limitations of ICA, there has been a growing interest in various techniques aimed at visualizing vascular walls and evaluating the mechanisms of myocardial ischemia. Some of these methods are invasive, based on the introduction of a catheter, such as intravascular ultrasound (IVUS) and fractional flow reserve (FFR) assessment.
Transesophageal echocardiography (TEE)
TTE may be useful for detecting CAA. With the TEE it is possible to visualize the proximal segments of the coronary arteries. It can be useful as a complement to ICA, to demonstrate the anomalous course of the main coronary artery; a predominant systolic flow pattern in the anomalous coronary artery can be observed with pulsed doppler [5].
Comparative studies are not available to determine the ability of TEE to identify CAA against other methods. Its limitations are due to its invasiveness and the high cost.
Transthoracic echocardiography (TTE)
TTE is a non-invasive and low-cost method. With this examination the origin of the coronary arteries can be evaluated.
It is especially useful for pediatric age studies; in the adult population it is more difficult due to the lack of an adequate thoracic acoustic window. The screening study for children and adolescents (up to age 18 years), was done by Davis and colleagues on 2.388 children; four anomalies of coronary origin were found, with an incidence of 0.17%, correlating with the autopsy studies of the general population [6]. However, Pelliccia et al. were unable to visualize the RCA ostium in 20% of young athletes, a population expected to have good image quality [7].
Magnetic resonance angiography (MRA)
MRA avoids the administration of ionizing radiation and presents excellent images. In determining the coronary origin, MRA is more effective than ICA, especially in patients with congenital heart disease.
In experienced centers, free breathing sequences can display the coronary ostium and course in almost all patients, with sedation in most young children (age < 7 years) [8].
Ripley et al., in the largest MR study avaible, were able to decribe the anatomy and detect 116 cases of CAA between 59.844 MR scans [9].
His biggest limitation, for now, is in determining the distal course of the coronary arteries. Therefore, this technique is less useful for assessing fistulas, the coronary origin outside the coronary sinuses (for example, from a ventricle or from the pulmonary artery) and collateral vessels. Furthermore, displaying the posterior descending branch can become problematic. MRI has contraindications such as the presence of metal objects, the state of pregnancy, claustrophobia. For patients under the age of 35, MRA is however the first instance examination after echocardiography, when it is necessary to exclude the presence of anomaly of origin.
Computed Tomography Angiography (CTA)
CTA has shown the best ability in the evaluation of CAA, because it gives the possibility to evaluate also the distal segment of the coronary vessel. The disadvantage of this diagnostic is that it uses ionizing radiation and the contrast medium that is potentially nephrotoxic or allergenic. Technical advances in computed tomography have improved image quality, diagnostic performance and accuracy of coronary artery CT. The main factors that determine the quality of CTA are spatial and temporal resolution and volumetric coverage. With the new generation CT scanners, the spatial resolution is about 0.2-0.3 mm, which is lower than the spatial resolution of traditional coronary angiography (0.1 mm). The temporal resolution varies between 135-175 ms, and it is now possible to reach a true temporal resolution of 70 ms. These values are satisfactory for the evaluation of the heart in diastole without movement artifacts related to the heartbeat, but it is still far from the excellent temporal resolution of ICA (4-7ms). The new CT scanners have 320 layers and allow an anatomical coverage of 16 cm in one rotation allowing to capture the entire heart volume in a single beat. The main challenge of CTA has been to reduce the radiation dose with strategies such as modulating the intensity of the radiant beam and sequential scanning with prospective cardiac gating. It is now possible to complete a CTA by administering a dose of 1-4 mSv and even less than 1 mSv, under particularly controlled conditions, with a significant reduction in the volume of contrast medium needed reduced to 50 cc. Multi-planar reconstruction techniques, three-dimensional volumetrics, volumetric renderings, MIP (maximum intensity projection) and curve techniques are used. The sensitivity of CTA for the display of CAA is 100%.
For this reason, CTA has currently become the method of choice for the diagnosis and preoperative assessment of CAA, always keeping in mind the age of the patient [10-12].
Patient Work-up
According to the most recent recommendations of the American College of Cardiology and the American Heart Association Task Force on Clinical Practice Guidelines, the most effective initial screening methods are the CTA or MRA in symptomatic patients [13]. Surgical repair is indicated when in cases of anomalous coronary arteries arising from the pulmonary artery and when a coronary artery originates from the opposite sinus with interarterial course if symptoms are present, or when there is evidence of inducible ischemia in these territories [14]. The myocardial SPECT-CT with exercise stress test proved to be a first-choice method in the evaluation of inducible ischemia in CAA patients [15].
When the patient has a right coronary artery anomaly and no evidence of ischemia, management is more controversial. A conservative approach in this situation can be reasonable.