RENAL CELL CARCINOMA - CLEAR CELL SUBTYPE (CC-RCC)
Clear cell is the most common subtype of RCC. Most of the cases are sporadic (95%)[3], but can be familial or associated with von Hippel-Lindau syndrome. Compared to chromophobe and papillary subtypes, CC-RCC has a poor prognosis, with a five-year survival of 50-60%[3]. Multicentricity and bilaterality are rare, although it can be present in up to 5% of patients[3].
On computed tomography (CT), CC-RCC usually presents as a mass with an expansile growth pattern. Due to its hypervascularization, it shows strong enhancement in the corticomedullary phase, followed by wash-out. Larger CC-RCC may show a more heterogeneous appearance due to necrosis, cystic degeneration or hemorrhage [2].
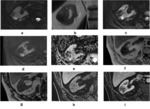
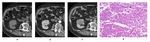
On T1-weighted images, CC-RCC often shows signal intensity similar to the renal parenchyma; on T2-weighted images, it is usually hyperintense. Deviations from this typical pattern occur due to necrosis, hemorrhage and cystic component. Necrotic areas show low signal intensity on T1-weighted images and moderate to high signal on T2-weighted images. The manifestations of intra-tumoral hemorrhage will depend on the stage of degradation of blood components: subacute hemorrhage will show hyperintensity in both T1 and T2-weighted sequences, while chronic hemorrhage, because of the accumulation of a large amount of hemosiderin, will show low signal intensity both in T1 and T2-weighted images. The presence of intra-tumoral lipids results in a loss of signal intensity on T1-weighted opposed-phase images compared with the in-phase images. Dynamic sequences often show a hypervascular lesion, excluding necrotic areas that typically lack enhancement. The role of ADC values in characterizing the histological subtypes of renal carcinoma is still limited, nonetheless, some studies suggest that the mean ADC values of CC-RCC were found to be higher than those of non-CC-RCC [2] (Fig.1).

Fig. 1: Clear Cell RCC of the right kidney in a 70 year-old patient. Axial fat-suppressed T2 (a), coronal T2 (b), axial DWI b0 (c), DWI b1000 (d), ADC map, (e) axial T1 in-phase (f), T1 opposed-phase (g), T1- VIBE before gadolinium administration (h) and postcontrast (i). MR images illustrate a solid heterogeneous tumor with minimal restriction on higher b values (a,b,c), no signal loss on opposed-phase sequences (d,e) and enhancement in corticomedullary phase (f, g).
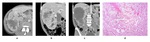
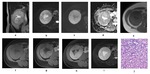
Histologically, CC-RCC contains cells with clear cytoplasm due to dissolved lipids and cholesterol (Fig.2), arranged in sheets or with an acinar or solid-nested growth pattern and prominent thin-walled vasculature, which contributes to the hypervascularity of the tumor. Necrosis, hemorrhage, calcification and cystic degeneration may occur in 4-15%[3].

Fig. 2: Clear cell RCC of the right kidney in a 61 year-old patient. Abdominal CT scan in axial (a) coronal (b) and sagittal(c) reconstructions in corticomedullary phase, showing an heterogeneous tumor with strong enhancement, similar to that of normal cortex,and central necrotic areas. Photomicrograph (hematoxylin-eosin, x100) of the surgically removed tumor (d) showing cells with clear cytoplasm.
RENAL CELL CARCINOMA – PAPILLARY SUBTYPE (P-RCC)
Papillary carcinoma is the second most common subtype of renal cell carcinoma and generally has a better prognosis than CC-RCC, with a five-year survival rate of approximately 90%[3]. They are bilateral in 4% of patients and show multifocality in up to 23% of patients[4].
On CT, a well-circumscribed homogenous mass is typically seen, usually located in the surface of the kidney, although larger tumors may show heterogeneity due to calcification, necrosis, and hemorrhage. It usually shows minimal enhancement after contrast administration in the corticomedullary phase.
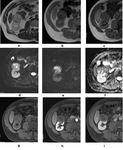
On T1-weighted images, P-RCC often shows signal intensity similar to the renal parenchyma, and low signal intensity on T2-weighted images. Dynamic sequences often show minimal enhancement in the cortical phase due to its low vascularity (Fig.3).

Fig. 3: Papillary RCC of the right kidney in a 58 year-old patient . Axial T2-weighted (a), axial T1 in-phase (b), T1 opposed-phase (c), DWI b0 (d), DWI b800 (e), ADC map (f), T1- VIBE before gadolinium administration (g), postcontrast administration in corticomedullary phase (h) and in early excretory phase (i). The dynamic sequences show a well-circumscribed lesion with minimal enhancement in the corticomedullary phase and late progressive enhancement. The tumor shows a capsule on morphological sequences and restriction on DWI.
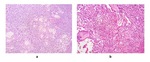
Histologically, P-RCC usually presents with a well-developed pseudocapsule. It has distinct features that correlate with the MR findings. The predominant papillary architecture is associated with the low signal on T2-weighted sequences. Type 1 P-RCC consists of lined up cells with papillary architecture, with scanty clear to basophilic cytoplasm and low nuclear grade. On the other hand, type 2 P-RCC consists of papillae formed by cells with eosinophilic cytoplasm and higher nuclear grade (Fig.4). The former has a better prognosis [5].

Fig. 4: Photomicrograph (hematoxylin-eosin, x 100) of two surgically removed papillary renal cell carcinomas. Type 1 P-RCC (a) with its scanty clear to basophilic cytoplasm contrasting with type 2 P-RCC (b) which exhibits cells with eosinophilic cytoplasm. Both of these tumors have a typical papillary architecture.
RENAL CELL CARCINOMA - CHROMOPHOBE SUBTYPE (C-RCC)
C-RCC is the third most common and has the best prognosis among all three RCC subtypes, with a five-year survival rate up to 92%[3].
On CT, the presentation is very variable, with an intermediate pattern of enhancement on the cortical phase, which depends on the tumor constitution. On MRI, C-RCC often shows intermediate to low signal on T2-weighted images, just like CC-RCC. It shares some similar imaging features with oncocytomas and sometimes their differentiation can be a real challenge. The enhancement pattern lays between CC-RCC and P-RCC (Fig.5).

Fig. 5: Chromophobe RCC of the left kidney in a 70 year-old patient. Abdominal CT scan with coronal reconstruction in corticomedullary phase (a). Axial T2 (b) and axial T1 -VIBE after gadolinium administration (c). A large tumor is seen with less enhancement when compared to the normal cortex and the extensive necrotic area.
Histologically, C-RCC cells have round to polygonal shape with well-defined cytoplasm borders, pale eosinophilic cytoplasm with fine reticular pattern and show characteristic perinuclear haloes (Fig.6). The histological aspect may mimic an oncocytoma, so it is important to use immunohistochemistry to make a final diagnose (Fig.7). C-RCC has a strong positivity to CK7.

Fig. 6: Chromophobe RCC of the right kidney in a 77 year-old patient. Axial precontrast (a) corticomedullary (b) and excretory phases (c), showing a well circumscribed lesion with minimal enhancement after contrast administration (b,c). Photomicrograph (hematoxylin-eosin, x100) of the surgically removed tumor (d) showing cells with pale eosinophilic cytoplasm and the characteristic perinuclear halos (arrow).

Fig. 7: Photomicrograph (hematoxylin-eosin, x 100) of chromophobe RCC (a). Photomicrograph (hematoxylin-eosin, x 200) of an oncocytoma (b). As in radiology, the pathologic features of both tumors are remarkably similar. The differential diagnosis can only be achieved by immunohistochemistry . Notably, C-RCC will show a strong positivity to CK7.
Two benign entities must be distinguished from renal cell carcinomas: angiomyolipoma and oncocytoma. The recognition of their imaging features may avoid unnecessary surgeries.
ANGIOMYOLIPOMA (AMP)
Angiomyolipoma is one of the most common renal lesions and as the name suggests it is composed of variable amounts of dysmorphic vessels, smooth muscle, and adipose tissue. Most of AMP are sporadic, although 20% are associated with tuberous sclerosis [4].
Classically, an angiomyolipoma has a high signal intensity on T1-weighted images and low signal on fat-suppressed sequences. It typically enhances quickly after contrast administration and shows a fast wash-out. Given this distinctive imaging features, it is frequently easy to identify (Fig.8 and 9).

Fig. 8: Angiomyolipoma of the left kidney in a 44 year-old patient. Axial T2-weighted (a) and fat-suppressed T2 (b). DWI b100 (c), ADC (d) showing minimal restriction. Coronal DIXON WATER (e) and coronal DIXON FAT (f) demonstrating an intra-tumoral fat component. Coronal T1-weighted in-phase (g) and opposed-phase, demonstrating decrease of signal intensity, consistent with AML. Axial T1-VIBE after gadolinium administration in corticomedullary phase (i) showing minimal enhancement which results from the few vessels within the tumor.
Fat-poor AMP accounts for 5% of AML [4] and represents a challenge for the radiologist as it appears very similar to RCC. Because of the low-fat content, it shows low signal both in T1 and T2-weighted sequences due to the presence of abundant smooth muscle, with no signal loss on fat-suppressed sequences. The best way to differentiate a fat-poor AMP from RCC is achieved by using DWI sequences, as it usually has a low ADC mean value, still, this is not specific.
Histologically, an angiomyolipoma represents a triphasic tumor composed of dysmorphic vessels, smooth muscle and adipose tissue (Fig.9).

Fig. 9: Angiomyolipoma of the left kidney in a 69 year-old patient. Axial T2-weighted (a) and fat-suppressed T2-weighted (b) demonstrating that the tumor contains fatty tissue. T1 in-phase (c) and opposed-phase (d), showing signal decreased, consistent with the diagnosis of AML. Axial T1-VIBE before (e) and after (f) gadolinium administration showing intra-tumoral enhancement. CT (g) of the same patient, showing a ROI (region of interest) of -26 HU, compatible with fatty tissue. Photomicrograph (hematoxylin-eosin, x 200) of the AML (h), showing the typical features of the tumor and where there are visible smooth muscle cells (arrow), vessels (arrow-head) and fatty tissue (star)
ONCOCYTOMA
Oncocytoma is a benign tumor that often mimics RCC, especially C-RCC, and unlike AMP it lacks any unique distinctive imaging feature. It usually appears as a well-circumscribed lesion showing a low signal on T1-weighted images and with high signal on T2-weighted images. Although is not specific for oncocytoma, a central scar is visible in 50-60% of cases[2]. On dynamic sequences, it usually shows minimal enhancement in all phases (Fig.10).
Histologically, just like C-RCC, oncocytoma cells have round to polygonal shape with well-defined cytoplasm borders, pale eosinophilic cytoplasm with fine reticular pattern and show perinuclear halos (Fig.10). Immunohistochemistry is essential to establish the final diagnose, opposing C-RCC, oncocytoma is CK7 negative.

Fig. 10: Oncocytoma of the left kidney in a 65 year-old patient. Abdominal CT scan in axial before contrast administration (a) and postcontrast in corticomedullary phase (b) and in early excretory phase (c) reconstructions. Coronal T2-weighted (d) and axial fat-suppressed T2 (e) sequences of the MR of the same patient. Photomicrograph (hematoxylin-eosin, x200) of the surgically removed tumor (f) showing poligonal/round cells with pale eosinophilic cytoplasm and with a small and central nucleus.
Although rare, other renal tumors can sometimes be a part of our daily practice and so its recognition is necessary (Fig.11 and 12).

Fig. 11: Abdominal CT scan in axial (a) and coronal (b, c) reconstructions of a 26 year-old patient with primary liver lymphoma, showing tumor metastases in the right kidney (yellow arrow).

Fig. 12: Synovial sarcoma of the left kidney in a 35 year-old patient. Abdominal CT scan with axial (a) and coronal (c) reconstructions before contrast administration and postcontrast in corticomedullary phase (b,d,e). CT shows a very large, invasive kidney mass with minimal enhancement in the postcontrast phases. Photomicrograph (hematoxylin-eosin, x 100) of the surgically removed tumor (f).
Among benign tumors, metanephric adenoma (Fig.13) should be emphasized, due to its similarity with P-RCC.

Fig. 13: Metanephric adenoma of the right kidney in a 48 year-old patient. Coronal T2-weighted (a), axial DWI b0 (b), b1000 (c), ADC map (d), T1-weighted (e), T1-VIBE before gadolinium administration (f), in the postcontrast corticomedullary phase (g), excretory phase (h), and fat-suppressed T2 (i) . MR shows a well-defined lesion with restriction on DWI sequences (b,c,d) and late minimal enhancement after gadolinium administration in the excretory phase. Photomicrograph (hematoxylin-eosin, x 100) of the surgically removed tumor (j), showing small cells with minimal cytoplasm disposed in a tubular pattern.
Some presentations of urothelial carcinoma can occasionally mimic RCC (Fig.14). Certain specific imaging features of UC suggest the diagnose, such as the existence of a filling defect on the excretory phase, the presence of secondary hydronephrosis (usually associated with advanced forms), and the calyceal epicenter of the tumor.

Fig. 14: Urothelial carcinoma of the left kidney in an 80 year-old patient. Abdominal CT scan before contrast administration in axial reconstruction (a). Postcontrast in corticomedullary phase in axial (b) and coronal (d) reconstructions. Early excretory phase in sagittal (c) and coronal (e) reconstructions. An ill-defined lesion is seen, which induces a filling defect on the excretory phase. Photomicrograph (hematoxylin-eosin, x 100) of the surgically removed tumor (f) shows the typical infiltrative features of urothelial carcinoma.