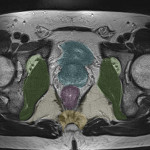
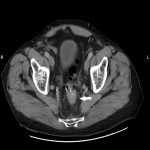
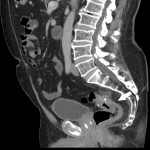
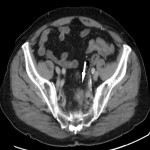
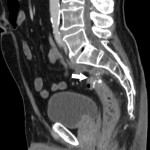
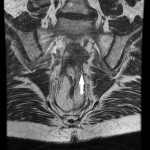
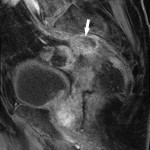
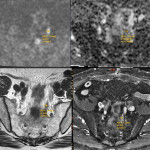
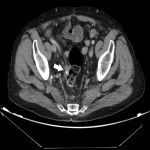
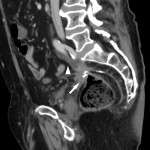
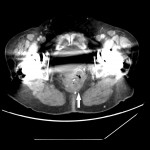
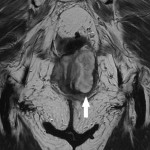
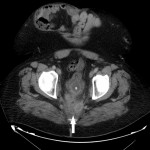
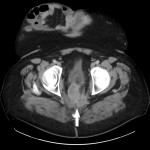
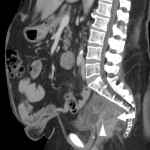
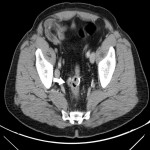
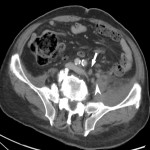
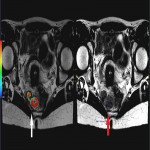
SITES OF LOCAL RECURRENCE
There are several classification systems based on anatomical compartments to systematically describe the site of recurrence of rectal tumors:
- Presacral: adjacent to the sacral bone (most common).
- Anterior: it can affect the bladder, uterus, vagina, seminal vesicles or the prostate gland.
- Anastomotic: at the staple line (best prognosis).
- Lateral: affecting the pelvic sidewall in the obturator lymph node compartment or along the iliac vessels (worst prognosis).
- Perineal: involving the perineum, anal sphincter complex or ischioanal/ischiorectal spaces.
DIFFERENT TREATMENT: DIFFERENT PATTERN OF RECURRENCE
Low anterior resection (LAR) is the standard procedure for tumors located in upper two thirds or in the lower third when there is no evidence of sphincteric invasion and an acceptable resection margin can be achieved.
This type of surgery carries an increased risk of anastomotic and presacral LR, especially in the subgroup of patients with positive lymph nodes who have not undergone neoadjuvant radiotherapy.
On the other hand, abdominoperineal resection (APR) rates continue to decrease as a better understanding of the biology of rectal cancer is progressively achieved. Still, it remains the procedure of choice in certain situations, e.g., involvement of sphincteric complex, impossibility to perform a LAR with an adequate resection margin, in older patients or in those with poor baseline functional status.
Some authors have suggested that poorer outcomes observed in APR may be associated with the surgical approach, perhaps due to how thin the mesorectum is at the level of the lower rectum or because of the close distance to the pelvic floor, resulting in higher circumferential resection margin involvement and an increased probability of LR, especially in the presacral and the lateral spaces. This interpretation is nevertheless controversial, for bulky, extensive and poorly-differentiated tumors in the lower part of the rectum usually require an APR.
Lastly, as shown by the TME trial, lateral pattern of recurrences represents about 20% of all LR and it seems that omitting radiotherapy before TME might increase the risk for this type recurrence.
FOLLOW-UP PROTOCOL
A considerable number of patients with rectal cancer will have a disease recurrence following primary therapy. This is why intensive follow-up strategies have become mandatory in order to detect early asymptomatic recurrences in the subset of stage II (T3/4 N0 M0) and stage III (T3/4 N+ M0) patients who have undergone a curative resection of with or without neoadjuvant treatment .
Many studies have shown the benefit in terms of survival of early detection of LR with imaging techniques as compared with CEA testing, as it translates in a considerable increase in overall survival given the higher probability that salvage surgery can be then performed.
In this context, CT is the modality of choice, since it can more easily rule out concomitant local metastatic deposits in the lungs and the liver. However, it is less sensitive and especially less specific than MRI when it comes to discriminating between postoperative changes and recurrence in the pelvis when used alone.
The greater cost of MRI, its lower availability and its limited value in the detection of lung metastases, however, have relegated it to a less preeminent role.
Nevertheless, MRI is recommended in patients who have undergone transanal endoscopic microsurgery (TEM) and in some patients with small residual tumors after neoadjuvant treatment. It can also be used in patients after chemorradiation who enroll in a “watch-and-wait" strategy.
As for the rest of the cases, MRI is only recommended as a problem-solving tool.
WHAT TO LOOK FOR
On CT, LR usually appears as a soft-tissue growth in or near the surgical site:
- Intramural or extramural bowel wall thickening adjacent to the anastomotic line.
- Nodule or mass invading the surrounding structures.
- Enlarged regional lymph nodes: tumors can spred along superior hemorrhoidal route towards the mesorectum and mesocolon or along the middle and inferior hemorrhoidal vessels toward the hypogastric and obturator nodes, and then to the paraaortic nodes.
Radiologists must take into account that internal iliac nodes are usually not excised so for lower rectal cancer, there is a risk that they will be left behind should the surgeon not be advised otherwise. The same applies to inguinal lymph nodes or external iliac and common iliac groups.
As for MRI features, in patients who have undergone TME, enlarging rounded intermediate signal intensity lesions should be considered suspicious, as opposed to stable lineal signal abnormalities at the resection site, as well as new areas of restricted diffusion in patients with no signs of infection or dehiscence.