A.CENTRAL NERVOUS SYSTEM
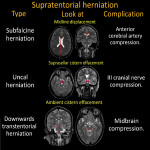
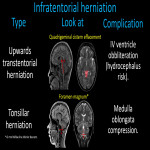
1.CEREBRAL HERNIATION
Mass effect from tumor lesions or vasogenic edema are the two main causes of cerebral herniation [3,4].
Slow growing tumors can produce minor symptoms, unlike fast growth lesions that produce sudden neurological deficit and high intracranial pressure.
Herniations may be supratentorial or infratentorial; the key to identify them is to define brain tissue displacement by looking at the midline, ventricles, and cisterns. It’s important that the radiologist reports these entities since they may have certain specific complications.
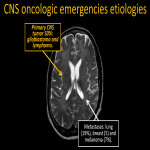
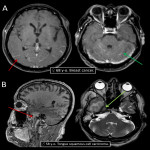
2.LEPTOMENINGEAL CARCINOMATOSIS
It usually occurs because of hematogenous dissemination from neoplasms (melanoma, breast, and lung), or by direct extension from head and neck tumors, or primary CNS neoplasms (medulloblastoma, ependymoma or lymphoma) [5,6].
Imaging findings include lineal or nodular meningeal enhancement of convexities, cranial nerves, basal cisterns, and spinal cord.
In severe cases it may result in hydrocephalus or spinal cord compression.
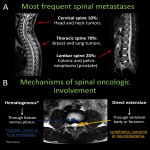
3.SPINAL CORD COMPRESSION
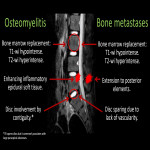
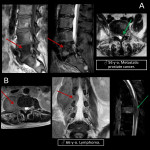
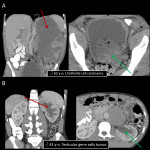
Spinal cord compression must be suspected in every oncologic patient with new ongoing lumbar pain. The spine is the most common bone metastatic location with thoracic segment being the most frequently compromised [7,8].
Spinal metastases are typically hypointense on T1w-images and hyperintense on STIR/T2w-images. Radiologists should differentiate from spondylodiscitis and must determine the grade of medullary compression and the presence of myelitis.
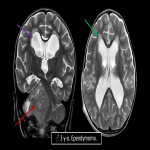
4.HYDROCEPHALUS
Generally, hydrocephalus has been classified as obstructive or non-obstructive according to CSF circulation impairment. Leptomeningeal carcinomatosis and intraventricular neoplasms are the most frequent etiologies.
Ventricular dilation could be easily depicted on images identifying ventriculomegaly proximal to the obstruction site with transependimal edema. The dilation of the temporal horns of the lateral ventricles are usually an early sign. Concomitant sulcal widening, rather than sulcal effacement, could help distinguish from volume loss.
B.THORAX
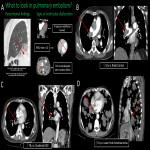
1.PULMONARY EMBOLISM (PE)
PE is one of the most common complications in oncology patients, either by hypercoagulability state, surgeries, or the tumor itself. Breast, lung, renal and hepatocellular tumors are frequently associated with this entity. AngioCT is the preferable modality as it depicts filling defects in pulmonary arteries.
Radiologists must inform parenchymal manifestations, such as lung infarct, and the presence of pulmonary hypertension or ventricular dysfunction. Tumoral emboli typically enhance with beaded peripheral arteries and sometimes avidity at PET-FDG.
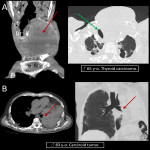
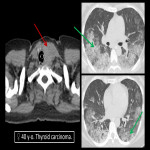
2.AIRWAY OBSTRUCTION
Obstruction is defined as narrowing >50% of the tracheal or bronchial lumen. Lung cancer is the most frequent etiology, followed by thyroid tumor, lymphoma, carcinoid tumor and adenomegalies. Symptoms change according to the site of obstruction varying from nonspecific symptoms in distal involvement to severe acute respiratory failure in proximal compromise [9]. CT with MPR reformations is the key modality to directly depict the presence of airway obstruction, severity, and etiology.
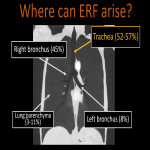
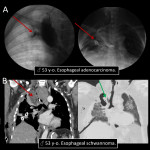
3.ESOPHAGEAL-RESPIRATORY FISTULA
The most common site of ERF is the trachea with esophagus and lung carcinoma the most frequent causes [10].
At CT images is sometimes difficult to directly depict a communicating tract, but ERF must be suspected if there are small airway disease signs. The fistula is often surrounded by focal soft tissue thickening due to inflammation or tumor itself. Fluoroscopic esophageal studies with iso-osmolar hydro-soluble iodized contrast can help confirm the site [11].
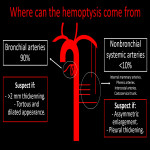
4.MASSIVE HEMOPTYSIS
Angio-invasive tumors such as lung squamous-cell carcinoma and adenocarcinoma are the most common etiologies, followed by carcinoid tumor and endobronchial metastasis from breast, kidney, or colon. Bleeding arises 90% from bronchial arteries and the most important signs are wall thickening >2 mm, with a tortuous and dilated appearance. It may also arise from collateral non-bronchial arteries originating from virtually any systemic vessel in proximity to the thorax.
Hence, it's recommended to start with enhanced CT in arterial phase first, rather than angiography for accurate detection of bleeding origin [12]. Signs of alveolar hemorrhage may also be depicted.
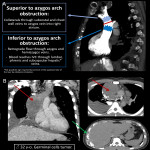
5.SUPERIOR VENA CAVA SYNDROME
Clinic presentation of SVCS is broad and includes facial and superior limb edema, stridor or neurologic alteration [13].
Etiology corresponds in 95% of cases to extraluminal compression by tumors (lung, thyroid, esophagus masses, or mediastinal adenomegalies). In other patients, there could be endoluminal obstruction by masses as leiomyosarcoma or by catheter associated thrombosis. Main image findings are filling defects, narrowing of the VCS and the presence of collateral circulation. Radiologists must establish the level of the obstruction as it could present with specific collateral circulation determining treatment approaches [14].
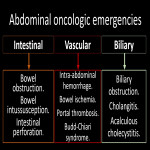
C.ABDOMEN
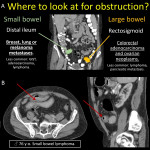
1.INTESTINAL OBSTRUCTION
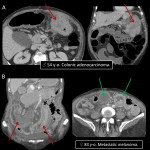
A variety of malignancies [15] as well as adhesions, radiation, or inflammatory changes could cause intestinal obstruction [16]. CT is the imaging choice to establish location, severity, etiology, complications, and treatment.
Findings include enhancing thickening of the bowel wall, proximal dilation, fecal content in small bowel, colonic “apple core” sign, and enhancing mass at transition point. Intussusception is another obstruction cause since tumors serve as leading point for bowel segment telescoping over itself. Imaging signs include target sign and mass at the leading point [17].
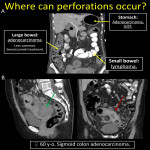
2.INTESTINAL PERFORATION
Most common site of perforation is the large intestine and it’s usually a blow-out type perforation [16]. CT studies depict pneumoperitoneum, site of perforation and ancillary findings of air contained in tumor, mural defect, irregular wall thickening and enhancement, fistulas, and abscesses [17]. Besides the multiple tumors associated with high risk of perforation, it has been also reported in patients treated with Bevacizumab [11].
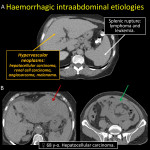
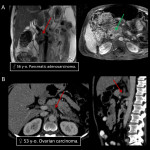
4.INTRAABDOMINAL HEMORRHAGE
Various cancers have a higher risk of spontaneous rupture and bleeding specifically those with subcapsular location, hypervascularity, and a rapid growth rate [17]. The location of hemoperitoneum (30-45 UH) helps point out the site of bleeding [15]. IV contrast depicts abnormal persistent enhancement in hemoperitoneum and the sentinel clot sign (45-70 UH) near the bleeding point.
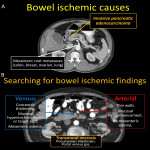
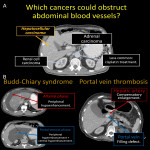
5.ACUTE VASCULAR OBSTRUCTION
Vascular obstructions may be caused by hypercoagulation status, tumor invasion or chemotherapy agents (Cisplatin). Thrombi appear as intraluminal defects on CT; bland thrombi are non-enhancing with minimal luminal expansion while tumor thrombi enhance and are located adjacent to the mass causing important dilation of the vessel [15]. Imaging signs are nonspecific and vary according to the type of ischemia.
Budd Chiari syndrome is characterized by obstruction of the hepatic outflow venous tract. DopplerUS shows hypoechoic material within venous lumen, stenosis or fibrous hyperechoic cords at the obstruction site. Subhepatic collaterals, caudate lobe hypertrophy, hepatomegaly, compensatory enlargement of the hepatic artery, and ascites with edematous parenchyma are indirect signs of obstruction. Acutely occluded veins may appear hyperattenuating on non-contrast CT [16].
6.BILIARY
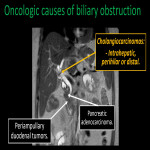
Tumors adjacent to the biliary tree may cause compression at this level. CT studies show bile duct dilation, extension and etiologies [15].
MRI can aid in staging of cholangiocarcinoma and pancreatic adenocarcinoma.
Complications from this pathology include cholangitis, septicemia, cholecystitis and hepatic abscesses. Cholangitis may derive in gallbladder perforation, pyogenic hepatic abscesses, portal vein thrombosis, and biliary peritonitis [16]. Images show thickening of the biliary duct walls, with CT and MRI showing possible geographic areas of parenchymal enhancement[15]. Cholecystitis is seen as a distended gallbladder with thickened wall and mucosal hyperenhancement [17].
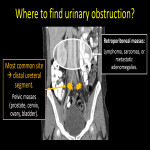
7.GENITOURINARY OBSTRUCTION
Pelvic and retroperitoneal tumors may cause compression over the urinary tract. CT allows assessment of hydronephrosis, ureter and retroperitoneum. Imaging is also used for assessing nephrostomy tubes or ureteral stenting, their position and possible complications (displacement, bleeding, and infections) [18].
CT Urography characterizes obstruction, tumor, and complications showing a decreased enhancement of renal parenchyma in corticomedular and nephrogenic phases with subsequent persistent nephrogram.