Type:
Educational Exhibit
Keywords:
Abdomen, Catheter venography, Angioplasty, Arterial access, Stents, Cirrhosis, Embolism / Thrombosis
Authors:
A. Israr, R. R. Yadav, S. Singh, K. B. K. Rangan, R. V. Mall
DOI:
10.26044/ecr2022/C-19962
Background
PATHOPHYSIOLOGY:
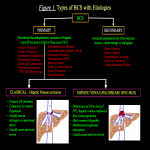
- The primary pathophysiology is thrombosis of HV, suprahepatic IVC or both – termed PRIMARY BCS [2].
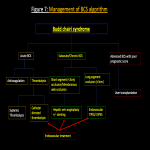
- Outflow of blood from liver may also occur due extrinsic compression from space occupying lesions, tumour thrombi, pericardial disease etc.: resulting in clinical symptoms similar to primary HVOTO – termed SECONDARY BCS[2]. Figure 1
- Acute thrombosis leading to alteration of physiological blood flow, results in acute symptoms of liver failure with rapidly developing ascites, pedal edema, abdominal wall venous distention etc. The classic ‘flip-flop’ enhancement is seen in these cases [3].
- At times the acute phase passes asymptomatically and the thrombus resolves with fibrosis and stenosis of vein [4]. This results in gradual alteration in physiological blood flow. These patients commonly present with features of portal hypertension and progress to cirrhosis. Classical intrahepatic veno-venous collaterals are seen in these cases [5].
- When the stenosed segment is short (< 3 cm), these are termed as ‘web’[2] . Long segment blocks are ≥3cm in length.
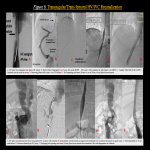
- There is wide geographic difference in presentation and underlying pathophysiology of HVOTO [6]. It was seen that in the western population, the disease tends to present more commonly in acute phase with thrombosis [7]. In eastern/asian population, the disease tends to present insidiously and commonly with fibrosis/stenosis [8]. Figure 2
- HV involvement is common in western population [9]. A combined HV and IVC involvement is common in eastern population with isolated IVC involvement common in China [2,9].
- The underlying cause in eastern population is more commonly infection (veno-caval phlebitis) and pregnancy [6]. A host of procoagulant tendencies are common etiological factors in western population [2]. It is now established that the disease is multifactorial in nature [2].
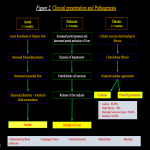
CLINICAL PRESENTATION:As a result of increased portal pressure, there is formation of ascites and venous collaterals. Chronically elevated portal pressure leads to hypoxic cell death, centrilobular necrosis and further leading to liver cirrhosis.
IMAGING DIAGNOSIS:
USG/DOPPLER: Diagnosis is based on imaging and depends on reliable demonstration of occlusion of HV, IVC or both. USG with Doppler is the most common modality applied and usually suffices for both diagnosis and treatment planning. In doubtful cases, further imaging with CT/MRI may be performed [10].
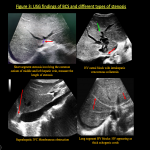
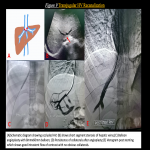
USG with Doppler typically shows [10]: Figure 3
- Reversal of flow in hepatic vein with or without loss of triphasicity;
- Length of occlusion needs to be measured;
- Intrahepatic veno-venous collaterals are pathognomonic;
- Features of portal hypertension with multiple intraabdominal and cavo-caval collaterals may be seen;
- Another specific observation is replacement of the hepatic vein by a fibrous echogenic cord;
- In acute conditions, echogenic thrombus may be demonstrable;
- As caudate lobe has independent drainage via small venules directly into intrahepatic IVC; the caudate lobe is usually hypertrophied with prominent draining veins. Enlarged caudate lobe may extrinsically compress the intrahepatic IVC;
- Focal nodules may be encountered: most commonly regenerative nodules and focal nodular hyperplasia.
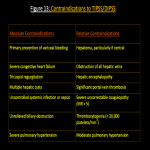
CT: CT triple phase is done when trans jugular intrahepatic portosystemic stent shunting (TIPSS) is planned for mapping the vascular anatomy [10].
- CT shows non-opacification of the hepatic veins in the venous phases, however false positive results may occur if there is insufficient time delay between contrast injection and venous phase acquisition.
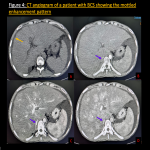
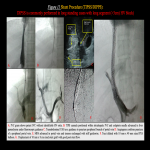
- Mottled appearance with central enhancement and peripheral hypo enhancement may be seen owing to sinusoidal and portal vein stasis. Figure 4
- Chronic BCS shows a shrunken liver with enlarged caudate lobe. Several collateralized pathways may be seen eg. left renal hemiazygos pathway, inferior phrenic, pericardiophrenic collaterals, and superficial collaterals of the abdominal wall etc. Regenerative nodules and focal nodular hyperplasia may be seen.
- Hepatic artery enlargement can be seen as it compensates for the reduced portal flow.
- Stasis of blood flow in the portal vein can produce portal vein thrombosis.
- It is essential to look out for any arterial enhancing lesion with washout as it may be an early developing hepatocellular carcinoma (HCC).
MRI: At our institute MRI is usually done if patient has contrast allergy, nephropathy or better delineate the nodules in liver. MRI helps in better delineation of the phase of BCS [10].
Acute BCS: Decreased T1-weighted and slightly elevated T2-weighted signals in the central liver accompanied with uneven increased arterial enhancement. Associated thrombus in hepatic vein or IVC.
Subacute: The periphery of liver now shows elevated T2-weighted signals with uneven increased arterial enhancement
Chronic: Enlarged caudate with atrophy of peripheral liver, collaterals, and a spider-web network pattern. Benign nodules are multiple in number, smaller sized, homogenously enhancing on arterial phase with slight hyperintensity in portal phase with no obvious washout. Malignant nodules (evolving HCC) show irregular and heterogeneous enhancement in the arterial phase and a portal phase washout.