Keywords:
Cardiac, Thorax, CT-Angiography, MR-Angiography, Contrast agent-intravenous, Embolism / Thrombosis
Authors:
E. A. Mershina1, M. A. Glazkova2, K. Mershin1, V. Sinitsyn1; 1Moscow/RU, 2Krasnogorsk/RU
Methods and Materials
Study populations consisted of 10 patients (m/f -3/7; mean age – 34.5+-3.1) with CTEPH.
CTA and MRA were performed in all the patients.
CTA was performed at 64-row scanner using dual-energy mode (GSI technique).
The volume of the injected contrast medium was 40-7 0ml.
MRA was performed at 1,5T MR system using 10-15 ml of contrast agent (1 mmol/ml).
3-5 ml of contrast agent injected at 2,5 ml/sec were used for the dynamic perfusion study.
After that CMR protocol for PH patents was implemented (SSFP and velocity-encoding images) for RV function assessment and stroke volume calculation.
MRA with bolus injection of contrast agent using CARE-bolus technique was used for MR-angiopulmonography.
Pulmonary MR- and CT-angiograms were analyzed for changes of the PA,
including perfusion defects,
caliber irregularities,
and intravascular thrombi.
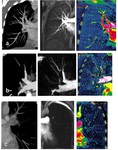
Three-point grading scale for evaluation of pulmonary perfusion was used (Fig. 1):
0-normal perfusion and no PA lesions;
1-hypoperfusion and PA stenosis;
2-absence of perfusion and PA occlusion.
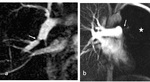
At Fig. 2 a left pulmonary artery occlusion (b) and stenoses in the branches of right pulmonary artery (a) due to "webs" and "bands" are shown.
Results of MRA were compared against CTA for analysis of pulmonary arteries (PA) patency and pulmonary perfusion.
Sensitivity,
specificity,
and diagnostic accuracy of MRA were calculated.
Receiver operator characteristic (ROC) analysis was performed to compare the diagnostic value of MRA with CTA.