Keywords:
Cardiac, Thorax, CT-Angiography, MR-Angiography, Contrast agent-intravenous, Embolism / Thrombosis
Authors:
E. A. Mershina1, M. A. Glazkova2, K. Mershin1, V. Sinitsyn1; 1Moscow/RU, 2Krasnogorsk/RU
Results
All the patients had CTEPH.
Patients data are presented in Table 1.
Table 1.
Patients data
|
Parameter
|
Value
|
|
Age (y.o.)
|
48.5±3.1
|
|
Mosaic attenuation pattern
|
10 (10)
|
|
Diameter of PA (mm)
|
33±7.6
|
|
PA/Ao diameter ratio
|
1,13±0,2
|
|
RV/LV diameter ratio
|
1,28±0,38
|
|
Collateral branches
|
7 (10)
|
|
PA occlusion (MRA)
|
55 (131) – 42 %
|
|
PA occlusion (CTA)
|
56 (131) - 42,
7 %
|
|
PA stenosis (MRA)
|
39 (131) - 29,7 %
|
|
PA stenosis (CTA)
|
48 (131) - 36,6 %
|
In total 131 segmental PA branches and 131 lung segments were included in the analysis.
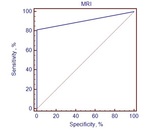
Per-segment analysis showed that sensitivity and specificity of pulmonary MRA in characterizing of PA lesions was 81,2 % and 100%,
compared with CTA (Fig. 3).
MRA and CTA were equally effective in the detection of segmental occlusions of the PA in CTEPH (55 vs 56 segmental branches) (Fig. 4,
Fig. 5). CTA was superior for the depiction of intraluminal "webs" and for the grading of PA wall thickening (48 vs 39 segmental pulmonary arteries for CTA vs MRA) (Fig. 6).
Strong correlation was obtained between CTA and MRA for detection of stenoses/occlusions of PA and presence/absence of perfusion defects (r=0.8 p<0.001 and r=0.9 p<0.001,
resp).
Right heart chamber overload could be graded using both CTA and cine-MR,
following MRA.